4.8: Endoscopic Transnasal Optic Nerve Decompression Technique
- Page ID
- 48896
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
ENDOSCOPIC TRANSNASAL OPTIC NERVE DECOMPRESSION
Boštjan Lanišnik, Janez Ravnik
This chapter focuses on the indications, decision making and surgical technique of endoscopic transnasal optic nerve decompression and presents some controversies relating to decompression for traumatic optic neuropathy. Endoscopic optic nerve decompression can be performed with little or no morbidity. It is done mainly for traumatic optic neuropathy. Other indications include skull base tumors e.g. meningiomas growing into the optic canal. or fibroosseous lesions of the skull base. Endoscopic optic nerve decompression is most suited to pathology located medial to the optic nerve. Lateral fractures of the sphenoid wing e.g. of the clinoid, are more easily accessed through a pterional approach.
Surgical Anatomy
Optic canal
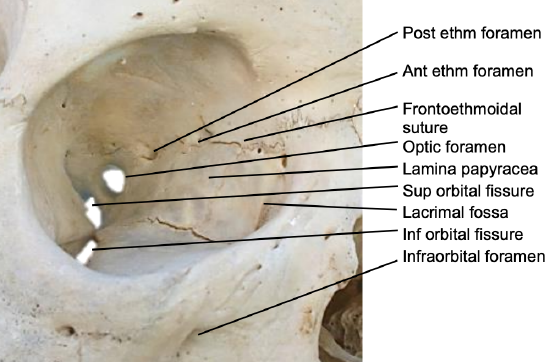
Figure 1: Right medial orbital wall
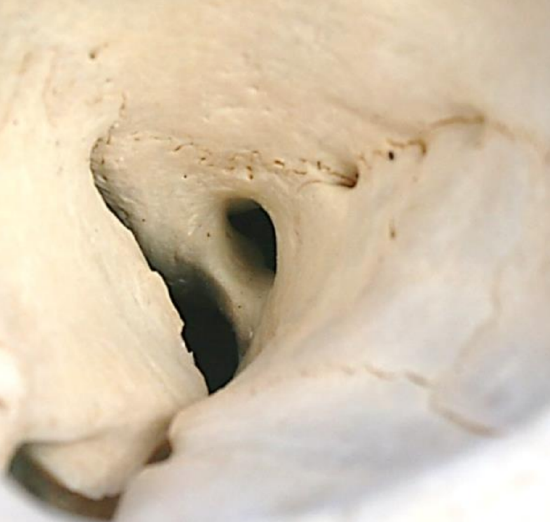
Figure 2: Close-up of right orbit demonstrating the position of the optic canal relative to the posterior ethmoidal foramen, superior orbital fissure and optic strut
The optic nerve enters the optic canal at the superomedial corner of the orbital apex. The canal is about 10 mm in length and contains the optic nerve, ophthalmic artery and sympathetic plexus. Laterally it is separated from the superior orbital fissure by a bony bridge called the optic strut (Figures 1, 2).
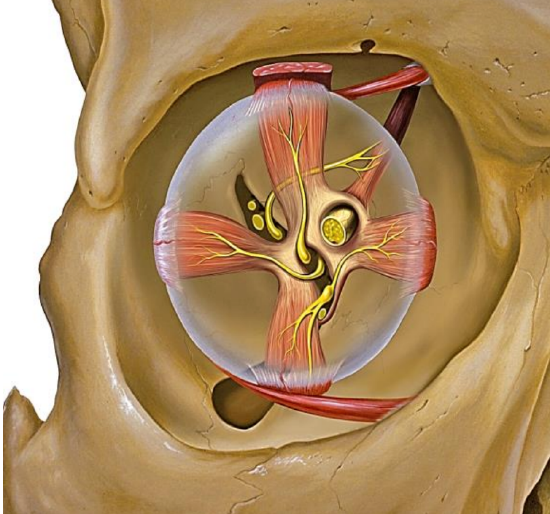
Figure 3: Eye muscles attach to Annulus of Zin 1
The tendinous Annulus of Zinn is attached at the upper, medial and lower margins of the optic canal (12 to 6 o’clock). It is the insertion for the extraocular muscles i.e. superior, medial, inferior and lateral rectus (Figure 3).
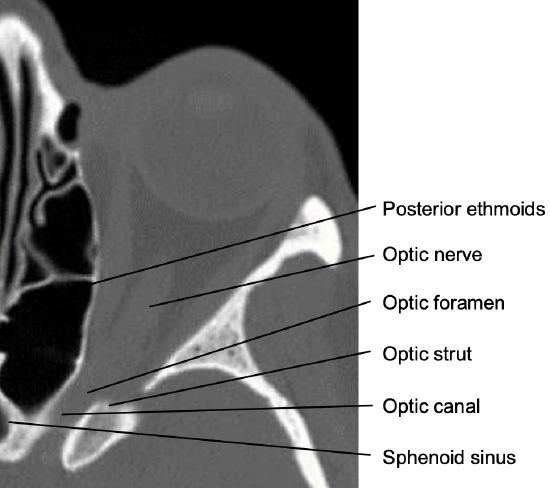
Figure 4: Note the posteromedial course of the optic canal
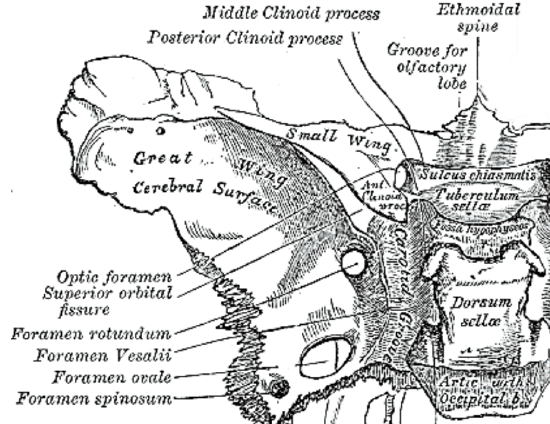
Figure 5: Relationships of optic canal to sphenoid and clinoid
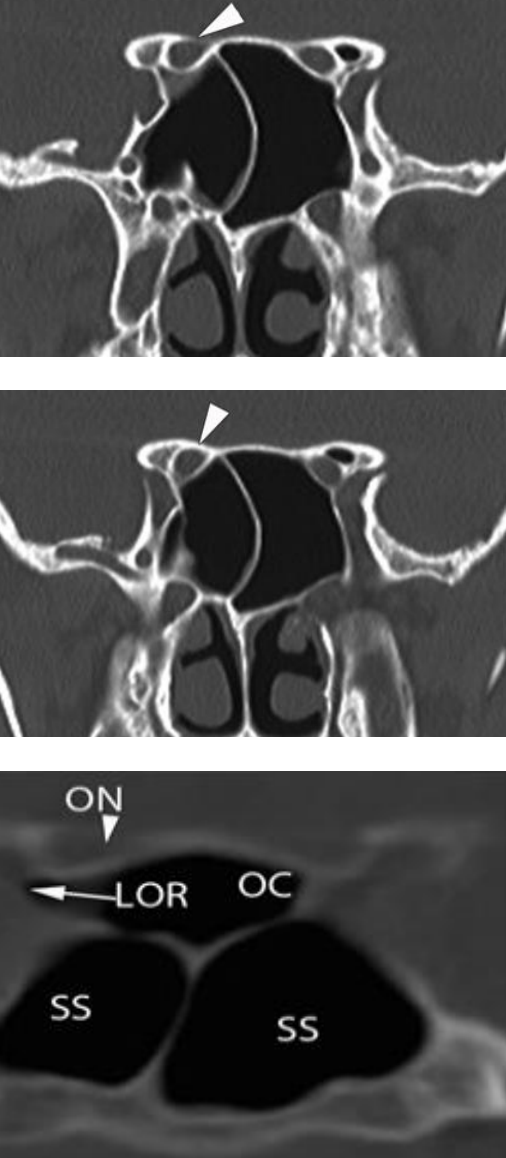
Figure 6: Coronal CTs and intraoperative photograph demonstrating the relations of the optic (ON) to the lesser wing of the sphenoid bone, the sphenoid bone, and the sphenoid sinus (SS) or alternatively into the Onodi cell (OC) of the posterior ethmoid
The optic canal courses in a posteromedial direction (Figure 4). The walls are formed by the body of the sphenoid and the lesser sphenoid wing. At the intracranial end it is shielded laterally by the anterior clinoid. The lateral wall of the optic canal is formed by the optic strut that blends superolaterally into anterior clinoid (Figures 4, 5, 6). The superior wall is formed by the anterior root of the lesser wing of the sphenoid bone; the medial wall is formed by the sphenoid bone (Figure 5).
This wall projects into the upper lateral wall of the sphenoid sinus or alternatively into the Onodi cell of the posterior ethmoid (Figure 6).
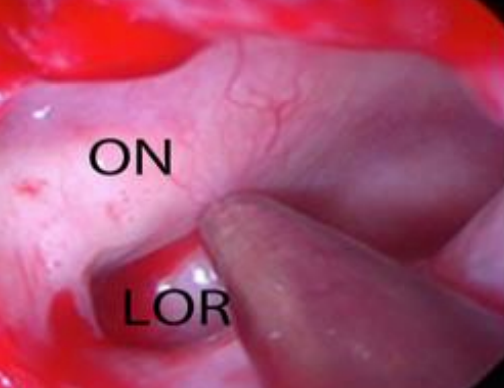
Figure 7: Left Optic nerve (ON) and lateral optico-carotid recess (LOR)
Ophthalmic artery (Figure 8)
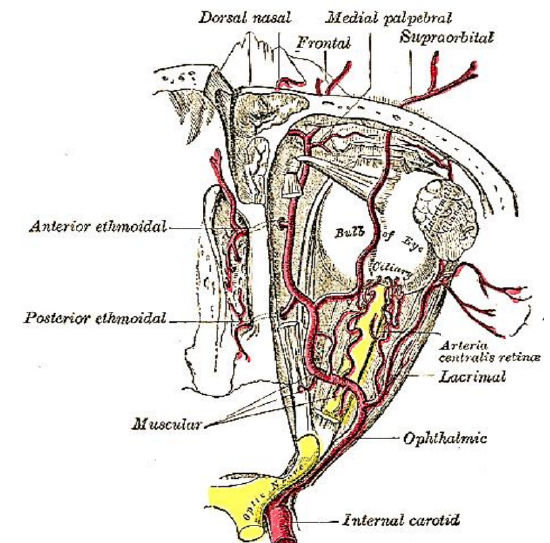
Figure 8: Ophthalmic artery gives rise to anterior and posterior ethmoidal arteries and the supratrochlear and supraorbital arteries
The ophthalmic artery arises from the medial aspect of the anterior loop of the internal carotid artery (ICA) just above the cavernous sinus. Intracranially it is located medially and below the optic nerve. In the optic canal the artery passes within the optic nerve sheath and below the optic nerve.
There are variations of the position of the ophthalmic artery within the canal. It can be found anywhere between 3 and 6 o’clock, so caution must be exercised when incising the optic nerve sheath.
Optic nerve
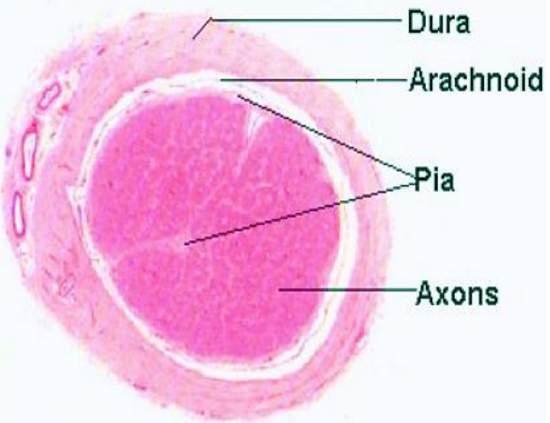
Figure 9: Cross-section of optic nerve
The optic nerve exits the orbit via the optic canal and courses posteromedially to the optic chiasm where there is a partial decussation (crossing over) of its fibers from the temporal visual fields of both eyes (Figure 9). Unlike peripheral nerves that contain epi-, peri- and endoneurium, the optic nerve is ensheathed in all three meningeal layers i.e. dura, arachnoid, and pia mater (Figure 9). The reason for this different structure is that the optic nerves are part of the central nervous system as they are outpouchings of the diencephalon (optic stalks) during embryonic development. Because fiber tracts of the central, as opposed to the peripheral nervous system are incapable of regeneration, optic nerve damage produces irreversible blindness.
Traumatic optic neuropathy (TON): classification and terminology
TON refers to injury to the optic nerve due to craniofacial trauma. Injury may be direct e.g. penetrating trauma and physical disruption of optic nerve continuity, or indirect when trauma forces are transmitted to the optic nerve with no/minimal disruption of the surrounding structures.
TON can be classified according to the location of the injury: head of optic nerve, intraorbital segment, intracanalicular segment or intracranial segments. The two most common sites of indirect TON are the intracanalicular segment (optic nerve sheath is adherent to the periosteum) and intracranial segment (in close proximity to the dural rings).
The optic nerve can be decompressed at other levels as well, e.g. the intracranial segment and the optic chiasm. Compressive symptoms at these levels are predominantly caused by tumors such as meningiomas and pituitary adenomas. Decompression of these segments requires transplanum and transsellar approaches that are not discussed in this chapter.
Controversies relating to optic nerve decompression in TON
Nerve decompression is a controversial procedure when performed for TON. It is performed only for indirect TON, since direct TON with optic nerve disruption is by definition an irreversible injury. There is a close association between initial visual acuity and final results. Patients who are blind and have no light perception when first examined have extremely poor or no chance of benefiting from decompression. Fractures of the optic canal as well as fragment impingement also carry a worse prognosis in some studies, although not in all.
Despite there being no scientific evidence that decompressing the optic nerve for indirect TON improves visual outcomes it is still performed in selected cases. The International Optic Nerve Trauma Study was intended to be a randomized control trial, but because of failure to recruit enough patients it was converted into an observational study. There was no statistically significant difference in visual acuity outcomes between the observational, steroid and surgical groups.
Role of corticosteroids in TON
Steroids have been used for spinal cord injury since the 1990s after the NASCIS 2 and 3 studies which demonstrated some benefits relating to neurological symptoms if methylprednisolone (MP) was administered within 8 hours of a spinal cord injury with initial a bolus of 30 mg/kg of MP, followed by infusion of 5.4 mg/kg/hr for the next 23 hours. Both studies were heavily criticized for their designs and questionable benefit of MP on improvement of the neurological deficits. Revised recommendations by the American Association of Neurological Surgeons (AANS) recommended against the use of steroids in the first 24 to 48 hours after spinal cord injury.
After publishing the results of the MRC CRASH study showing potential harmful effects of steroids in craniofacial trauma patients, the use of steroids for TON has become more limited, since most patients with TON have some form of concomitant intracranial injury.
A Cochrane Review by Yu-Wai-Man and Griffiths in 2011 compared 31 eligible double-blinded placebo-controlled, randomized trials of high-dose intravenous steroids in patients with indirect TON. The authors concluded that there is a high rate of spontaneous visual recovery and that there is no convincing data that would suggest any added benefit of steroids over observation alone. Nevertheless, many practitioners still use steroids as conservative management of the TON, but the decision must made on a case-by-case basis.
Indications & contraindications for optic nerve decompression
Optic nerve decompression is generally always indicated if continuity of the optic nerve is not disrupted and there is evidence of worsening of visual acuity.
Indications for optic nerve decompression include (from Palmer JN, Chiu AG)
- Traumatic optic neuropathy
- Graves’ ophthalmopathy associated with optic neuropathy
- Idiopathic intracranial hypertension
- Fibro-osseous lesions
- Neoplasms (sinonasal tumor, meningioma, orbital apex tumor)
Contraindications for optic nerve decompression include
- Complete disruption of the nerve or chiasm
- Complete atrophy of the nerve
- Carotid-cavernous fistula
- Medical comorbidities precluding general anesthesia
TON is one of the most frequent indications for optic nerve decompression. Because of the poor chance of a blind patient regaining useful vision after decompression we consider decompression only in cases where there is a displaced fracture of the canal, but there is no evidence that the nerve was severed. In patients with preserved light perception we always consider surgical decompression with/or without steroids.
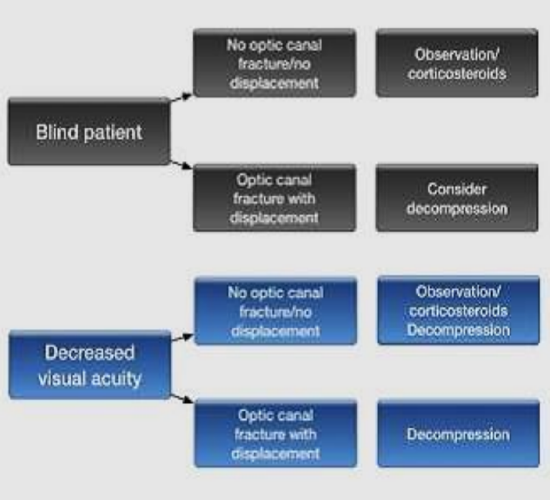
Table 1: Management algorithm for TON
With all the controversies of the surgical procedure as well as corticosteroids, we use the following algorithm for TON (Table 1).
Timing of intervention is also controversial, but logic dictates that decompression should be done as soon as possible after optic neuropathy is diagnosed, especially if it is of sudden onset. In patients with TON and fractures of the sphenoid wing and anterior clinoid that are displaced, lateral decompression via pterional approach must be considered.
Clinical presentation of optic neuropathy
A patient’s history will reveal the etiology of an optic neuropathy e.g. trauma, tumor, or surgery. Patients will also report how quickly the vision has deteriorated e.g. slowly over months with skull base tumors, and rapidly following trauma. In comatose patients it is difficult to establish whether a patient has TON, since there are no reliable electrophysiological tests that can be used.
Technique of transnasal optic nerve decompression
Standard instruments used for endoscopic sinus surgery are required e.g. through-cut, dissecting instruments as well as powered instrumentation. One can use a regular high-speed diamond drill usually with a 4 mm fine diamond burr, or special powered instruments with a hand piece that allows simultaneous irrigation and suction. It is important to use abundant irrigation during drilling to avoid thermal damage to the nerve.
Surgical technique
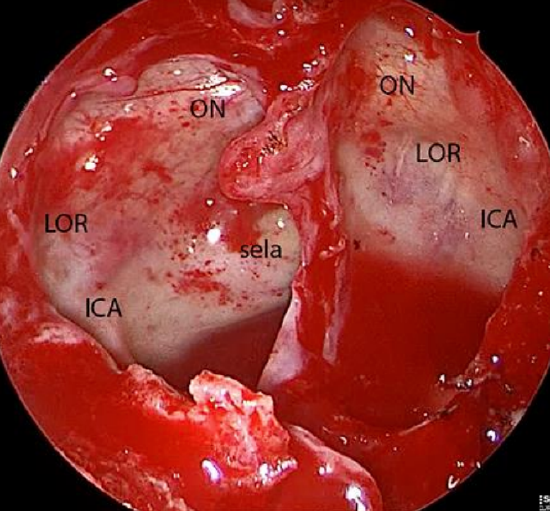
Figure 10: Lamina papyracea exposed up to face of sphenoid
- Perform a posterior ethmoidectomy with a wide antrostomy; for less experienced surgeons it is best to perform a complete ethmoidectomy and expose the lamina papyracea (Figure 10)
- Perform a wide sphenoidotomy with the anterior sphenoid wall resected to the skull base and to the lamina papyracea; this helps one to identify the orbital axis and orbital apex
- Identify the orbital apex and optic canal
- The easiest and safest way to achieve this is to resect the lamina papyracea posteriorly, starting 10-15 mm anterior to the face of the sphenoid
- One can sometimes remove the lamina papyracea with a Freer elevator, but if it is too thick, then a high-speed drill is first used to thin it to an egg-shell thickness
- Take care not to injure the periorbita and the underlying extraocular muscles; if the periorbita are injured, fat protrudes into the field of view; it is safe to carefully bipolar small pieces of fat
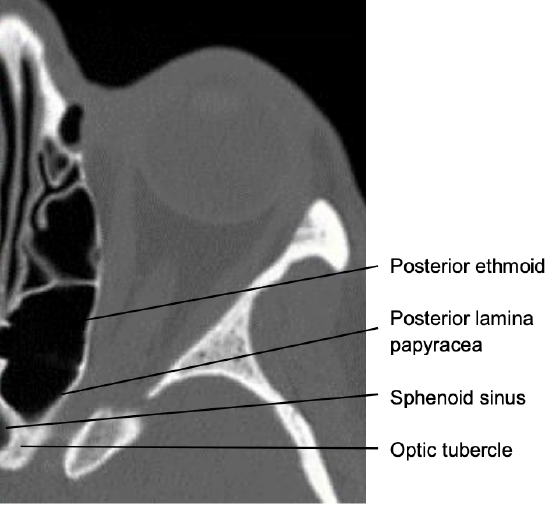
Figure 11: Note the posteromedial course of the optic canal
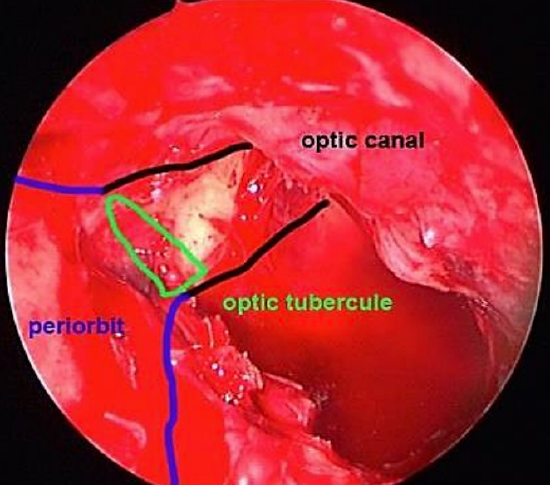
Figure 12: Lamina papyracea has been removed; periorbita exposed; wide sphenoidotomy; optic tubercle visible
4. After the posterior lamina papyracea has been removed, follow the periorbita posteriorly to where they converge at the orbital apex; the thick bone between posterior ethmoid and sphenoid is known as the optic tubercle (Figures 11, 12)
5. The Annulus of Zinn (Figure 3) is attached to the superior, inferior and medial margins of the orbital junction with the optic canal and can be identified after complete resection of the lamina papyracea at the level of the optic tubercle
6. The Annulus of Zinn (Figure 3) is attached to the superior, inferior and medial margins of the orbital junction with the optic canal and can be identified after complete resection of the lamina papyracea at the level of the optic tubercle
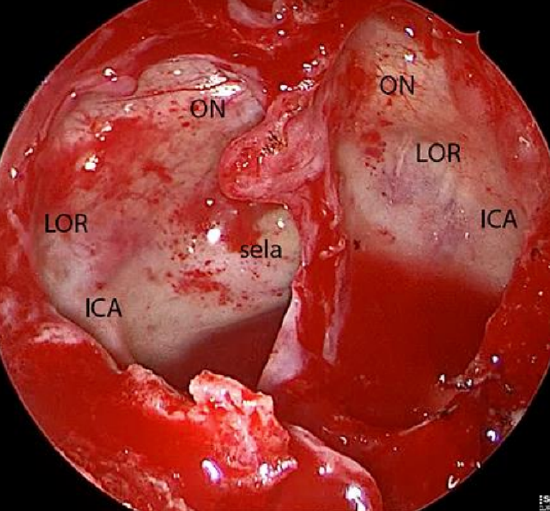
Figure 13: Endoscopic view of right and left sphenoid sinuses demonstrating the optic nerve (ON), internal carotid artery (ICA) and lateral optic-carotid recess (LOR)
7. Identify the bony protrusion of the optic canal in the sphenoid sinus; it is a continuation of the optic tubercle (Figure 13)
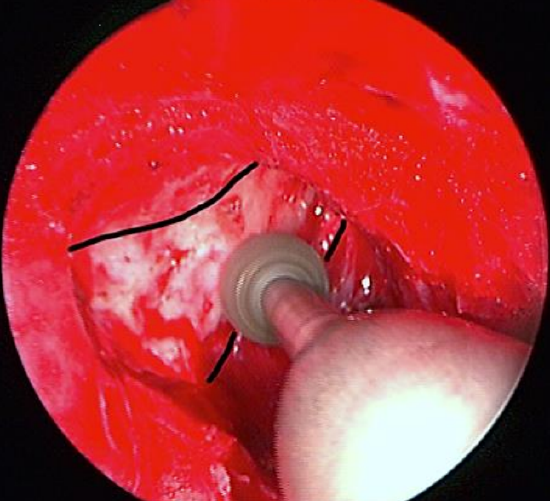
Figure 14: Thinning the bone down to an eggshell thickness with a high-speed drill
8. Use a diamond burr attached to a high speed drill or a powered endonasal hand piece to thin the bone down to an egg-shell thickness (Figure 14)
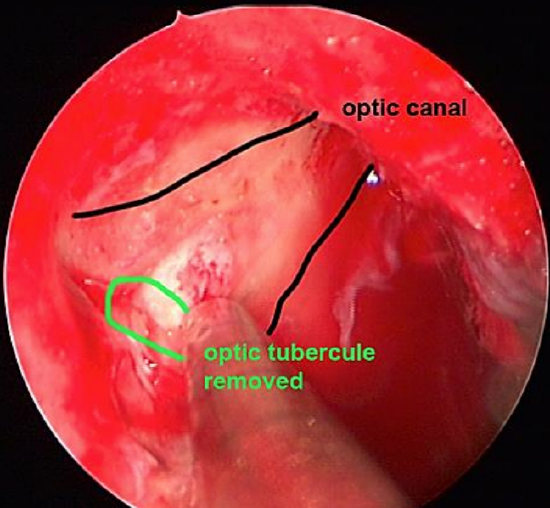
Figure 15: Thinning the bone down to an eggshell thickness with a high-speed drill
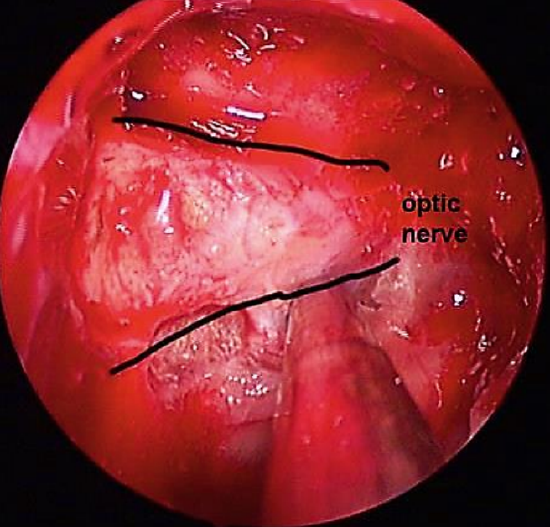
Figure 16: Optic nerve exposed
9. Remove the thinned bone with a Freer or Beale elevator and expose the optic nerve sheath (Figures 15, 16)
10. Incise the optic nerve sheath along the optic nerve and through the Annulus of Zinn. Place the incision(s) at the superomedial quadrant, as the ophthalmic artery is located in the inferomedial quadrant of the optic canal
11. Pack the nose and surgical cavity with hemostatic material; in case of bleeding, lightly pack the nose with sponges. Remove the packing on Day 1 or 2
12. Postoperative care: Instruct the patient to irrigate the nose with saline and corticosteroid drops. The authors advocate systemic antibiotics while the packing is in place (in the absence of a CSF leak)
References
- "Eye orbit anterior" by Patrick J. Lynch, medical illustrator. Licensed under CC By 2.5 via Wikimedia Commons - http://commons.wikimedia.org/wiki/Fi...t_anterior.jpg
Authors
Boštjan Lanišnik, MD, PhD
Dept. for ENT-Head and Neck Surgery
University Medical Center Maribor Ljubljanska 5
SI-2000 Maribor, Slovenia
blanisnik@me.com
Janez Ravnik, MD,PhD
Department of Neurosurgery
University Medical Center Maribor
Slovenia
jravnik@planet.si
Editor
Johan Fagan MBChB, FCS(ORL), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za


