3.3: Epithelial Tissue
- Page ID
- 63376
- Explain the structure and function of epithelial tissue
- Distinguish between tight junctions, anchoring junctions, and gap junctions
- Distinguish between simple epithelia and stratified epithelia, as well as between squamous, cuboidal, and columnar epithelia
- Describe the structure and function of endocrine and exocrine glands and their respective secretions
Most epithelial tissues are essentially large sheets of cells covering all the surfaces of the body exposed to the outside world and lining the outside of organs. Epithelium also forms much of the glandular tissue of the body. Skin is not the only area of the body exposed to the outside. Other areas include the airways, the digestive tract, as well as the urinary and reproductive systems, all of which are lined by an epithelium. Hollow organs and body cavities that do not connect to the exterior of the body, which includes, blood vessels and the heart, are lined by endothelium (plural = endothelia), which is a type of epithelium.
Epithelial cells derive from all three major embryonic layers. The epithelia lining the skin, parts of the mouth and nose, and the anus develop from the ectoderm. Cells lining the airways and most of the digestive system originate in the endoderm. The epithelium that lines vessels in the lymphatic and cardiovascular system derives from the mesoderm and is called an endothelium.
Characteristics of Epithelial Tissues
All epithelia share some important structural and functional features:
- Cellularity: This tissue is highly cellular, with no extracellular material present between cells. Adjoining cells are held tightly together by specialized intercellular connections between their cell membranes called.
- Polarity: The epithelial cells exhibit polarity with differences in structure and function between the exposed surface of the cell and the attached surface adjacent to the underlying body structures.
- Attachment: The basal surface of an epithelium is anchored to the underlying connective tissue by a complex structure of collagen and proteoglycans that is produced jointly by both tissues.
- Avascularity: Epithelial tissues are nearly completely avascular. No blood vessels cross the basement membrane to enter the tissue and nutrients must come by diffusion or absorption from underlying tissues or the surface.
- Regeneration: Many epithelial tissues are capable of rapidly replacing damaged and dead cells by quickly and continuously undergoing mitosis. Sloughing off of damaged or dead cells is a characteristic of surface epithelium and allows our airways and digestive tracts to rapidly replace damaged cells with new cells.
- Innervation: Many sensory receptors are attached to the basal cells or are present in the underlying connective tissue to detect changes in the environment at both the external and internal surfaces of the body.
Generalized Functions of Epithelial Tissue
- Physical Protection: Epithelial tissues provide the body’s first line of protection from physical, chemical, and biological wear and tear.
- Selective Permeability: The cells of an epithelium can act as gatekeepers of the body controlling permeability and allowing selective transfer of materials across a physical barrier. All substances that enter the body must cross an epithelium. Some epithelia often include structural features that allow the selective transport of molecules and ions across their cell membranes.
- Secretion: Many epithelial cells are capable of producing substances and releasing (secreting) them onto their apical surfaces. The epithelium of the small intestine releases digestive enzymes, for example. Cells lining the respiratory tract secrete mucous that traps incoming microorganisms and particles. A glandular epithelium may contain many secretory cells, such as the alpha and beta cells of the pancreas that produce hormones.
- Sensation: Some epithelial tissues also provide sensation. Nerve supply to epithelial tissues can alert the body to pressure, pain, and temperature from external or internal stimuli. This can help the body to maintain homeostasis or avoid harmful situations in the environment.
Epithelium Structure
Since epithelia are located at all free surfaces they separate the outside of the body from the inside of the body and have distinct structural specializations that allow them to fulfill this unique role. Both the individual cells and the sheet of cells exhibit a characteristic polarity: they have an apical surface that is exposed and is in contact with the outside as well as a basal surface that is attached to an underlying proteinaceous layer called the basement membrane. This membrane allows the epithelial cells to hook onto one side of it and the underlying connective tissue, called the lamina propria, to attach to the other (Figure \(\PageIndex{1}\)). This keeps the epithelium firmly anchored in place and helps prevent distortions and tearing.
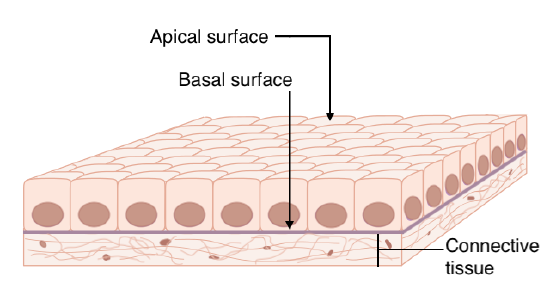
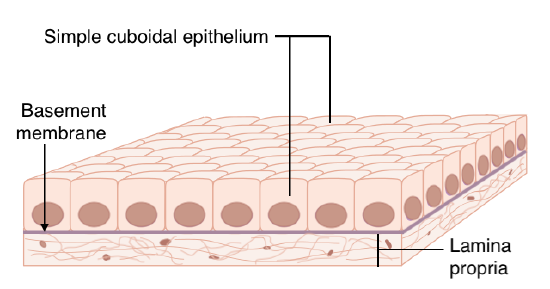
Epithelial cells also have a polarized distribution of organelles and membrane-bound proteins between their basal and apical surfaces. Particular structures found in some epithelial cells are an adaptation to specific functions. Certain organelles are segregated to the basal sides, whereas other organelles and extensions, such as cilia, when present, are on the apical surface. The transport channels within the cell membranes also differ between the two sides. For example, if you want to absorb a glucose molecule you have ingested you need two transporters - one to bring the molecule into the cell on the apical side and another to kick it out of the cell so it can enter into the bloodstream. If both transporters were exactly the same you could only, for example, move sugar into the cell!
Cell to Cell Junctions
Cells of epithelia are closely connected and are not separated by intracellular material. Three basic types of connections allow varying degrees of interaction between the cells: tight junctions, anchoring junctions, and gap junctions (Figure \(\PageIndex{2}\)).
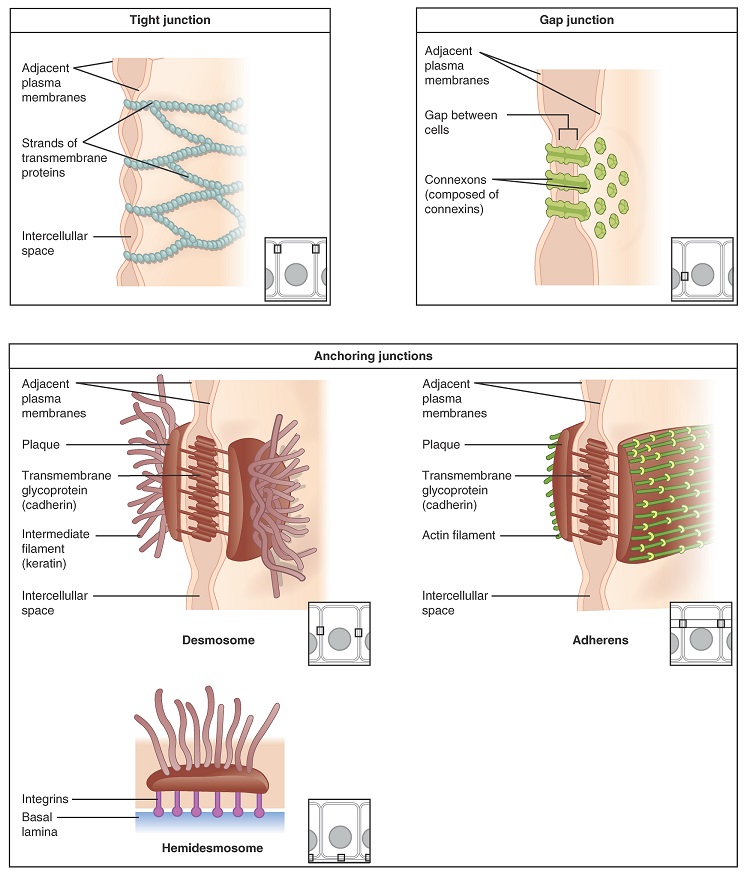
At one end of the spectrum is the tight junction, which separates the cells into apical and basal compartments. Tight junctions essentially "stitch" adjacent cell together, forming an impermeable barrier. An anchoring junction includes several types of cell junctions that help stabilize epithelial tissues. Anchoring junctions are common on the lateral and basal surfaces of cells where they provide strong and flexible connections. There are three types of anchoring junctions: desmosomes, hemidesmosomes, and adherens. Desmosomes occur in patches on the membranes of cells. The patches are structural proteins on the inner surface of the cell’s membrane. The adhesion molecule, cadherin, is embedded in these patches and projects through the cell membrane to link with the cadherin molecules of adjacent cells. These connections are especially important in holding cells together. Hemidesmosomes, which look like half a desmosome, link cells to the extracellular matrix, for example, the basal lamina. While similar in appearance to desmosomes, they include the adhesion proteins called integrins rather than cadherins. Adherens junctions use either cadherins or integrins depending on whether they are linking to other cells or matrix. The junctions are characterized by the presence of the contractile protein actin located on the cytoplasmic surface of the cell membrane. The actin can connect isolated patches or form a belt-like structure inside the cell. These junctions influence the shape and folding of the epithelial tissue.
In contrast with the tight and anchoring junctions, a gap junction forms an intercellular passageway between the membranes of adjacent cells to facilitate the movement of small molecules and ions between the cytoplasm of adjacent cells. These junctions allow electrical and metabolic coupling of adjacent cells, which coordinates function in large groups of cells.
Classification of Epithelial Tissues
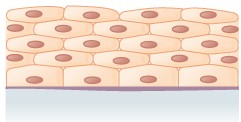
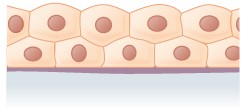
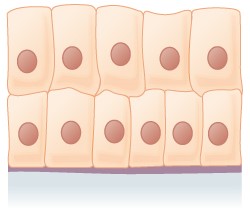
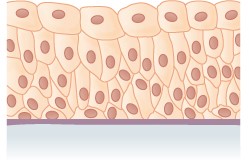
Epithelial tissues are classified according to the shape of the cells and number of the cell layers formed (Figure \(\PageIndex{3}\)). Cell shapes can be squamous (flattened and thin), cuboidal (boxy, as wide as it is tall), or columnar (rectangular, taller than it is wide). Similarly, the number of cell layers in the tissue can be one—where every cell rests on the basal lamina—which is a simple epithelium, or more than one, which is a stratified epithelium and only the basal layer of cells rests on the basal lamina with the remaining layers attaching to the more basal cells. Pseudostratified (pseudo- = “false”) describes tissue with a single layer of irregularly shaped cells that give the appearance of more than one layer. Transitional describes a form of specialized stratified epithelium in which the shape of the cells can vary.
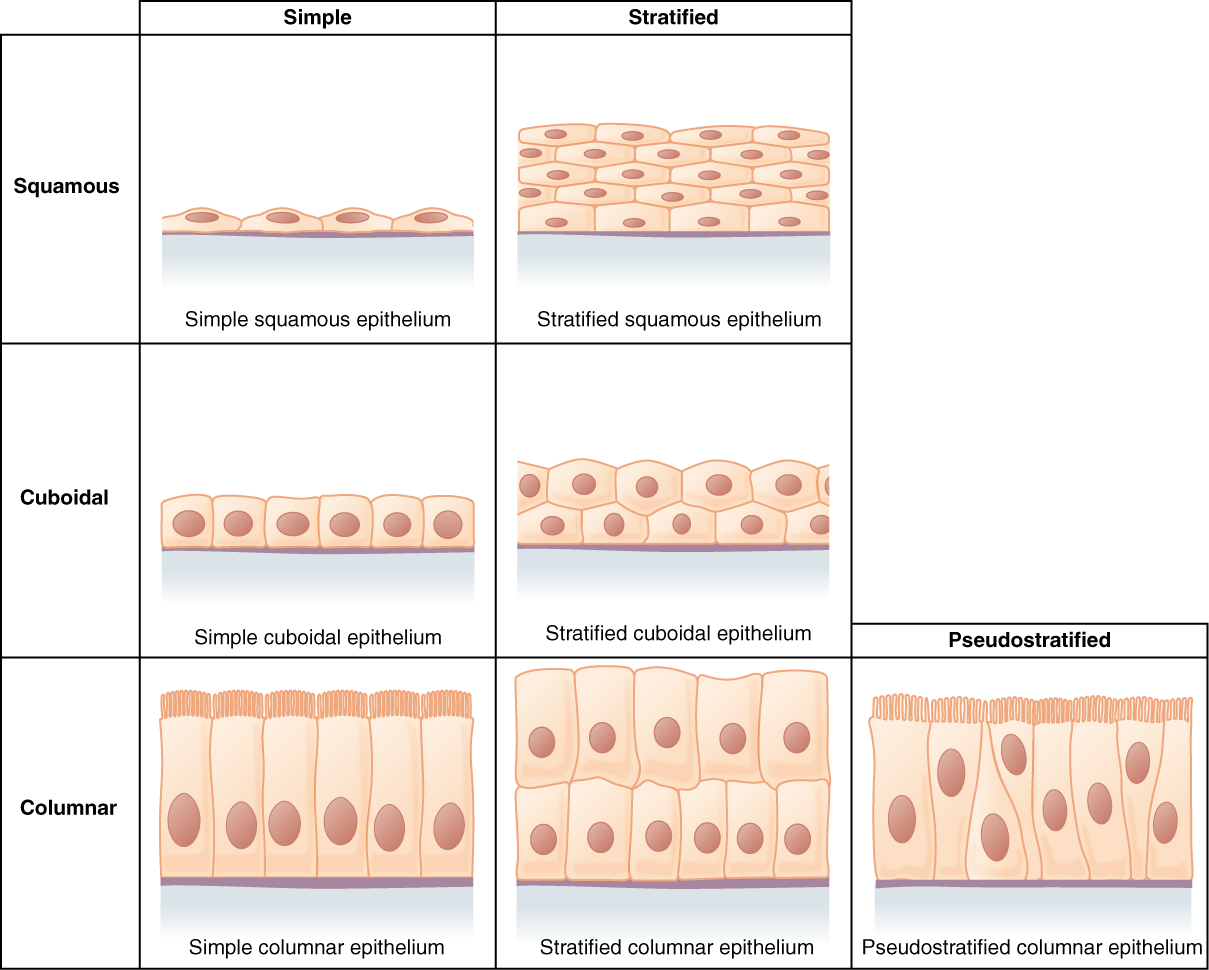
Simple Epithelia
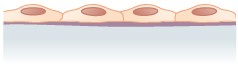
The shape of the cells in the single cell layer of simple epithelium reflects the functioning of those cells. The cells in simple squamous epithelium (Figure \(\PageIndex{3}\)) have the appearance of thin scales. Squamous cell nuclei tend to be flat, horizontal, and elliptical, mirroring the form of the cell. The endothelium is the epithelial tissue that lines vessels of the lymphatic and cardiovascular system, and it is made up of a single layer of squamous cells. Simple squamous epithelium, because of the thinness of the cell, is present where rapid passage of chemical compounds is observed. The alveoli of lungs where gases diffuse, segments of kidney tubules, and the lining of capillaries are also made of simple squamous epithelial tissue. The mesothelium is a simple squamous epithelium that forms the surface layer of the serous membrane that lines body cavities and internal organs. Its primary function is to provide a smooth and protective surface. Mesothelial cells are squamous epithelial cells that secrete a fluid that lubricates the mesothelium.
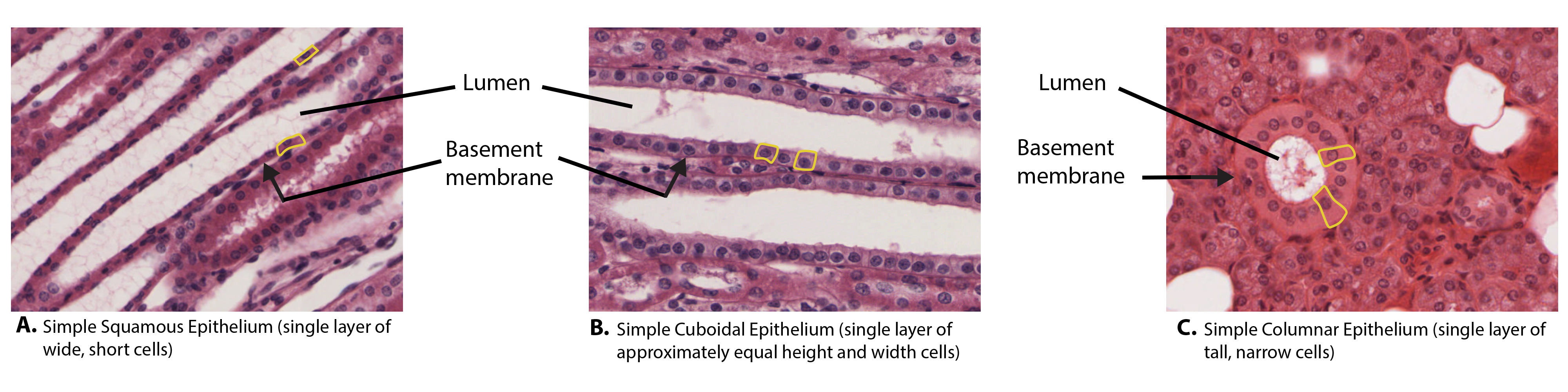
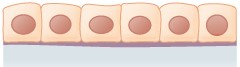
In simple cuboidal epithelium (Figure \(\PageIndex{3}\)), the nucleus of the box-like cells appears round and is generally located near the center of the cell. These epithelia are active in the secretion and absorption of molecules. Simple cuboidal epithelia are observed in the lining of the kidney tubules and in the ducts of glands.
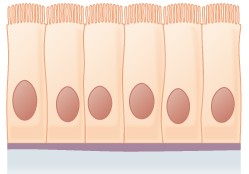
In simple columnar epithelium (Figure \(\PageIndex{3}\)), the nucleus of the tall column-like cells tends to be elongated and located in the basal end of the cells. Like the cuboidal epithelia, this epithelium is active in the absorption and secretion of molecules. Simple columnar epithelium forms the lining of some sections of the digestive system and parts of the female reproductive tract. Ciliated columnar epithelium is composed of simple columnar epithelial cells with cilia on their apical surfaces. These epithelial cells are found in the lining of the Fallopian tubes and parts of the respiratory system, where the beating of the cilia helps remove particulate matter.
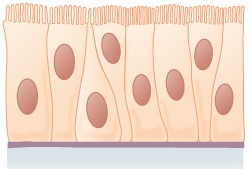
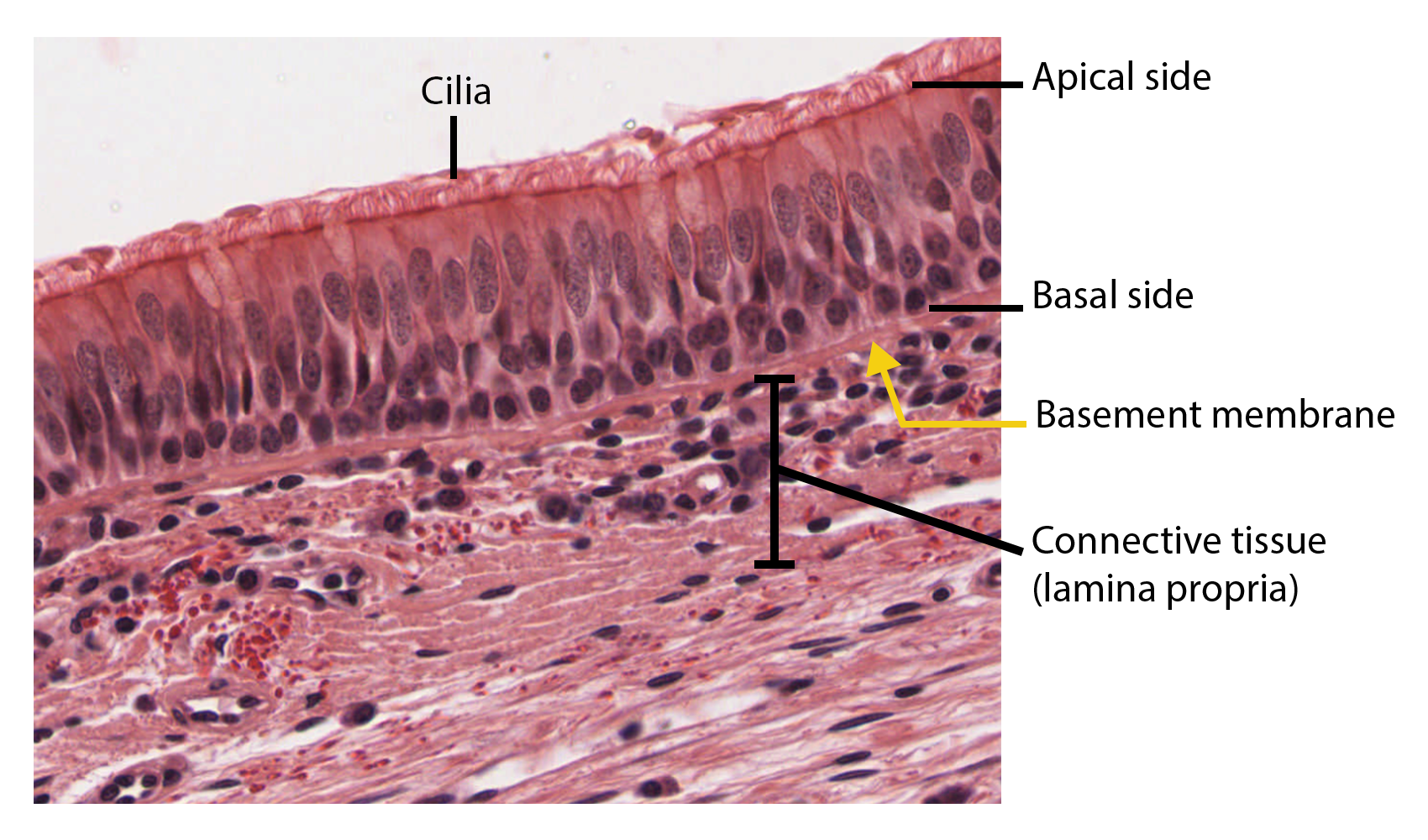
Pseudostratified columnar epithelium (Figure \(\PageIndex{4}\)) is a type of epithelium that appears to be stratified but instead consists of a single layer of irregularly shaped and differently sized columnar cells. In pseudostratified epithelium, nuclei of neighboring cells appear at different levels rather than clustered toward the basal side. The arrangement gives the appearance of stratification; but in fact all the cells are in contact with the basement membrane, although some do not reach the apical surface. Pseudostratified columnar epithelium is found in the respiratory tract, where some of these cells have cilia.
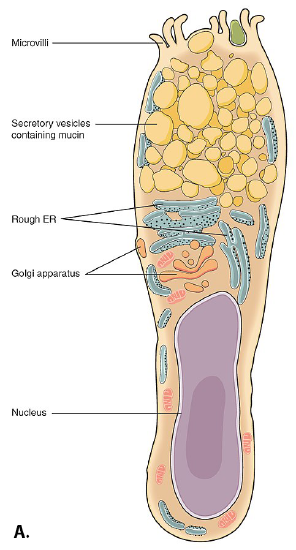
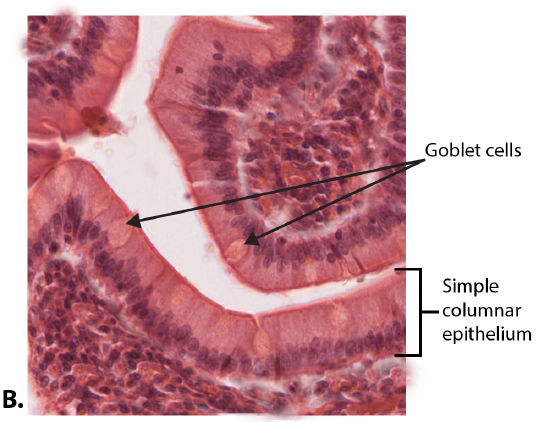
Both simple and pseudostratified columnar epithelia can include additional types of cells interspersed among the epithelial cells. For example, a goblet cell is a mucous-secreting unicellular “gland” interspersed between the columnar epithelial cells of mucous membranes (Figure \(\PageIndex{5}\)).
Stratified Epithelia
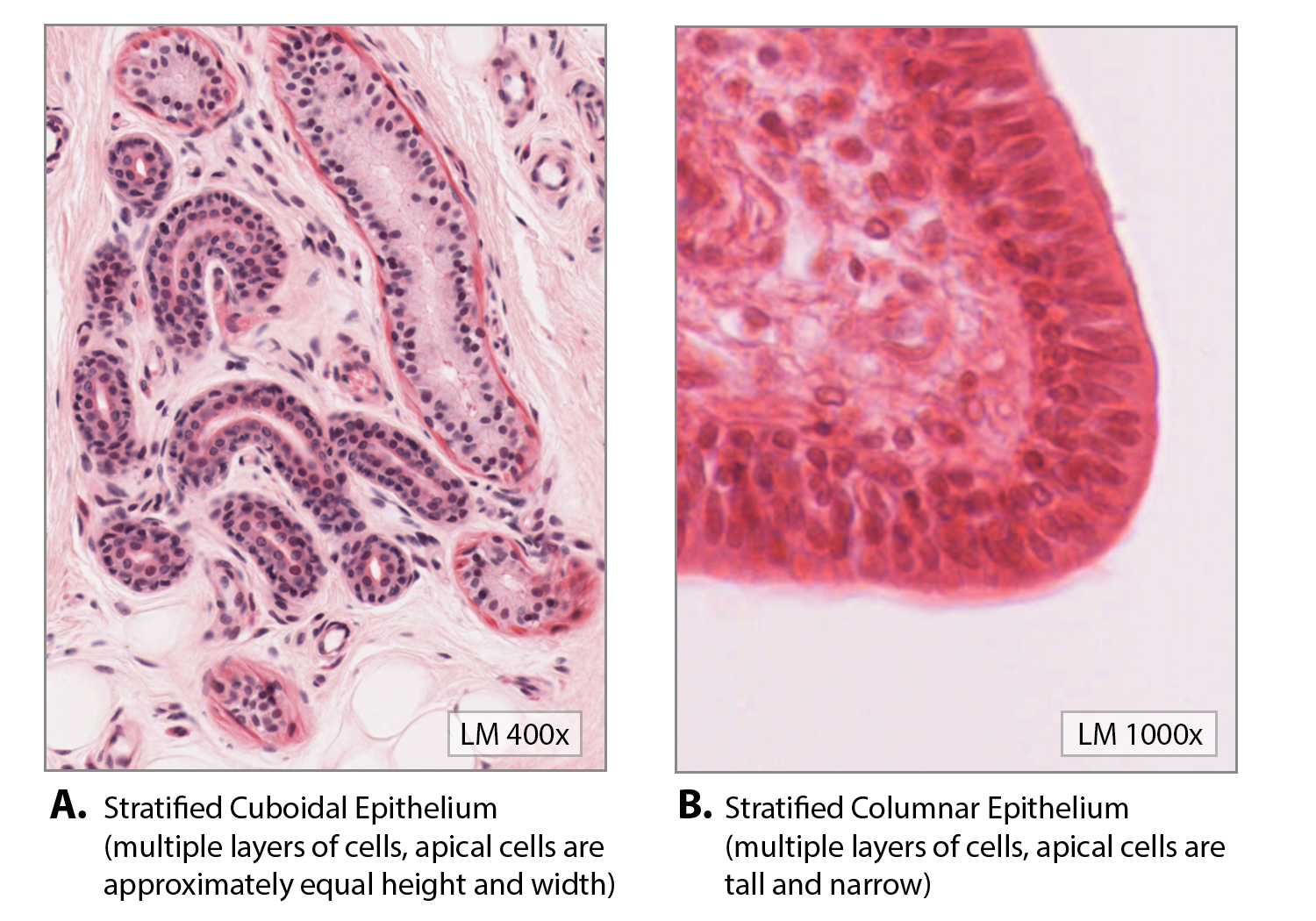
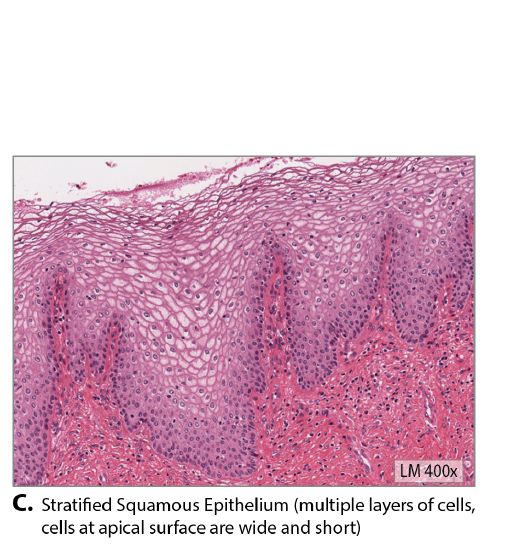
A stratified epithelium consists of several stacked layers of cells. This epithelium protects against physical and chemical wear and tear. The stratified epithelium is named by the shape of the most apical layer of cells, closest to the free space. Stratified squamous epithelium (Figure \(\PageIndex{6}\)) is the most common type of stratified epithelium in the human body. The apical cells are squamous, whereas the basal layer contains either columnar or cuboidal cells. The top layer may be covered with dead cells filled with the protein keratin. The epidermis of mammalian skin is an example of this dry, keratinized, stratified squamous epithelium. The lining of the oral cavity is an example of an non-keratinized, stratified squamous epithelium.
Stratified cuboidal epithelium and stratified columnar epithelium (Figure \(\PageIndex{6}\)) can be found in certain glands and ducts, but both are uncommon in the human body.
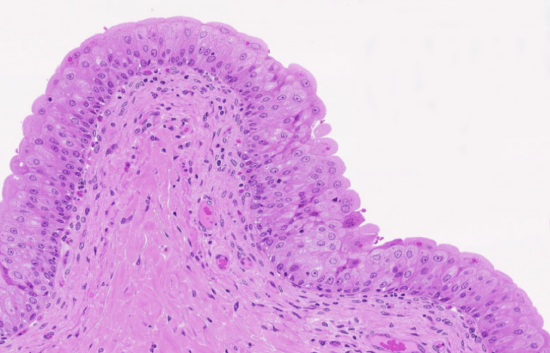
Another kind of stratified epithelium is transitional epithelium (Figure \(\PageIndex{7}\)), so-called because of the gradual changes in the shapes of the apical cells as the bladder fills with urine. It is found only in the urinary system, specifically the ureters and urinary bladder. When the bladder is empty, this epithelium is convoluted and has cuboidal apical cells with convex, umbrella shaped, apical surfaces. As the bladder fills with urine, this epithelium loses its convolutions and the apical cells transition from cuboidal to squamous. It appears thicker and more multi-layered when the bladder is empty, and more stretched out and less stratified when the bladder is full and distended.
| Tissue | Location | Function |
|---|---|---|
|
Simple Squamous Epithelium
|
Air sacs of lungs and lining of the heart, blood vessels, and lymphatic vessels. | Allows material to pass through by diffusion and filtration, and secretes lubricating substance |
|
Simple Cuboidal Epithelium
|
In ducts and secretory portions of small glands and in the kidney tubules | Secretes and absorbs |
|
Simple Columnar Epithelium
|
Ciliated tissues are in bronchi, uterine tubes, and uterus Smooth (nonciliated tissues) are in the digestive tract, gallbladder |
Absorbs; it also secretes mucous and enzymes May have goblet cells |
|
Pseudostratified Columnar Epithelium
|
Ciliated tissue lines the trachea and much of the upper respiratory tract |
Secretes mucus, ciliated tissue moves mucus Has goblet cells |
|
Stratified Squamous Epithelium
|
Lines the esophagus, mouth, and vagina; forms epidermis of the skin |
Protects against abrasion |
|
Stratified Cuboidal Epithelium
|
Sweat glands, salivary glands, and the mammary glands | Protective tissue |
|
Stratified Columnar Epithelium
|
The male urethra and the ducts of some glands | Secretes and protects |
|
Transitional Epithelium
|
Lines the bladder, urethra, and the ureters | Allows the urinary organs to expand and stretch |
Glandular Epithelium
A gland is a structure made up of one or more cells modified to synthesize and secrete chemical substances. Most glands consist of groups of epithelial cells. A gland can be classified as an endocrine gland, a ductless gland that releases secretions directly into surrounding tissues and fluids (endo- = “inside”), or an exocrine gland whose secretions leave through a duct that opens directly, or indirectly, to the external environment (exo- = “outside”).
Endocrine Glands
The secretions of endocrine glands are called hormones. Hormones are released into the interstitial fluid, diffused into the bloodstream, and delivered to targets, in other words, cells that have receptors to bind the hormones. The endocrine system is part of a major regulatory system coordinating the regulation and integration of body responses. A few examples of endocrine glands include the anterior pituitary, thymus, adrenal cortex, and gonads (ovaries and testes).
Exocrine Glands
Exocrine glands release their contents through a duct that leads to the epithelial surface. Mucous, sweat, saliva, and breast milk are all examples of secretions from exocrine glands. They are all discharged through tubular ducts. Secretions into the lumen of the gastrointestinal tract, technically outside of the body, are of the exocrine category.
Glandular Structure
Exocrine glands are classified as either unicellular or multicellular. The unicellular glands are scattered single cells, such as goblet cells, found in the mucous membranes of the small and large intestine.
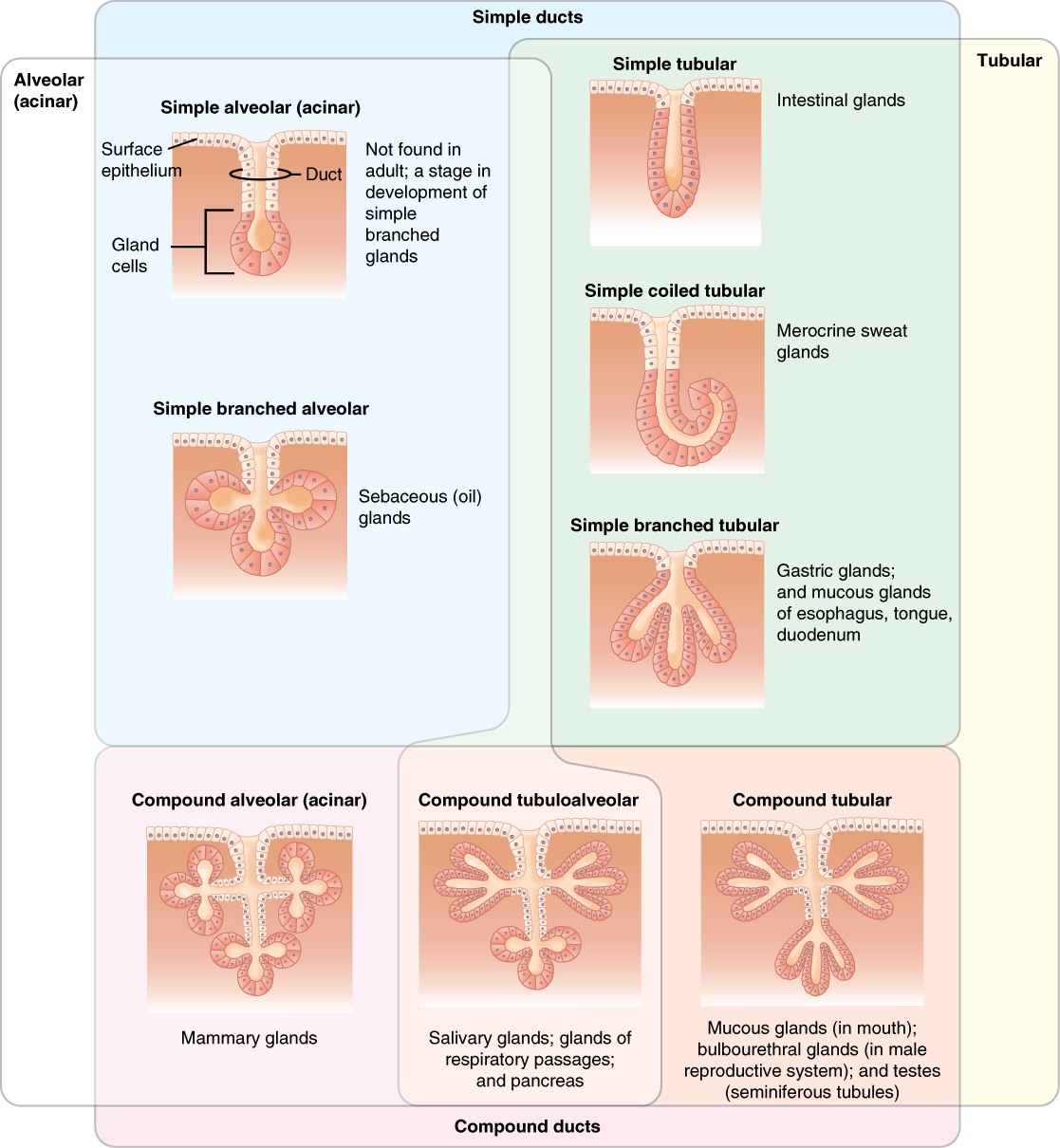
The multicellular exocrine glands known as serous glands develop from simple epithelium to form a secretory surface that secretes directly into an inner cavity. These glands line the internal cavities of the abdomen and chest and release their secretions directly into the cavities. Other multicellular exocrine glands release their contents through a tubular duct. The duct is single in a simple gland but in compound glands is divided into one or more branches (Figure \(\PageIndex{8}\)). In tubular glands, the ducts can be straight or coiled. Examples of tubular glands include simple tubular (e.g. intestinal glands), simple coiled tubular (e.g. merocrine sweat glands), simple branched tubular (e.g. gastric glands, and mucous glands of the esophagus, tongue, and duodenum), and compound tubular (e.g. mucous gland of the mouth, and bulbourethral glands and the seminiferous tubules of the testes, both of which are found in the male reproductive system). Glands that contain a duct that form pockets are alveolar (acinar), such as the exocrine portion of the pancreas. An example of an alveolar (acinar) gland includes simple alveolar, which are only found in the early stages of development as precursors to simple branched glands. Other examples include simple branched alveolar (e.g. sebaceous (oil) glands), and compound alveolar (e.g. mammary glands). Combinations of tubes and pockets are known as tubuloalveolar (tubuloacinar) compound glands. In a branched gland, a duct is connected to more than one secretory group of cells.
Methods and Types of Secretion
Exocrine glands can be classified by their mode of secretion and the nature of the substances released, as well as by the structure of the glands and shape of ducts (Figure \(\PageIndex{9}\)). Merocrine secretion is the most common type of exocrine secretion. The secretions are enclosed in vesicles that move to the apical surface of the cell where the contents are released by exocytosis. For example, watery mucous containing the glycoprotein mucin, a lubricant that offers some pathogen protection is a merocrine secretion. The eccrine glands that produce and secrete sweat are another example.
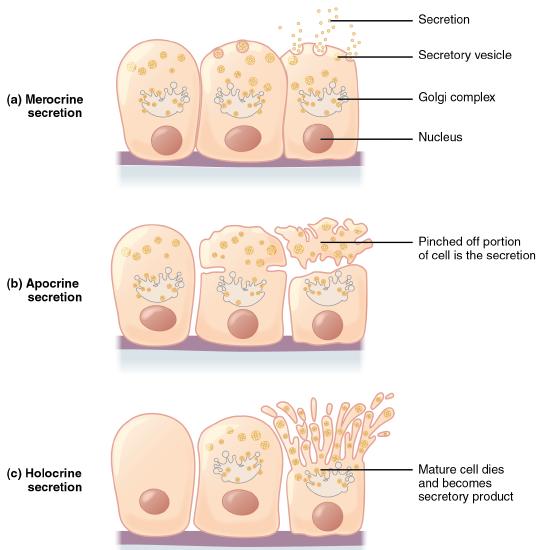
Apocrine secretion accumulates near the apical portion of the cell. That portion of the cell and its secretory contents pinch off from the cell and are released. Some sweat glands of the axilla region are classified as apocrine glands. Both merocrine and apocrine glands continue to produce and secrete their contents with little damage caused to the cell because the nucleus and golgi regions remain intact after secretion.
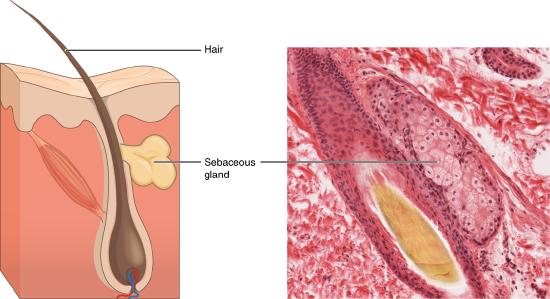
In contrast, the process of holocrine secretion involves the rupture and destruction of the entire gland cell. The cell accumulates its secretory products and releases them only when it bursts. New gland cells differentiate from cells in the surrounding tissue to replace those lost by secretion. The sebaceous glands that produce the oils on the skin and hair are holocrine glands/cells (Figure \(\PageIndex{10}\)).
Glands are also named after the products they produce. The serous gland produces watery, blood-plasma-like secretions rich in enzymes such as alpha amylase, whereas the mucous gland releases watery to viscous products rich in the glycoprotein mucin. Both serous and mucous glands are common in the salivary glands of the mouth. Mixed exocrine glands contain both serous and mucous glands and release both types of secretions.
Concept Review
In epithelial tissue, cells are closely packed with little or no extracellular matrix except for the basal lamina that separates the epithelium from underlying tissue. The main functions of epithelia are protection from the environment, coverage, secretion and excretion, absorption, and filtration. Cells are bound together by tight junctions that form an impermeable barrier. They can also be connected by gap junctions, which allow free exchange of soluble molecules between cells, and anchoring junctions, which attach cell to cell or cell to matrix. The different types of epithelial tissues are characterized by their cellular shapes and arrangements: squamous, cuboidal, or columnar epithelia. Single cell layers form simple epithelia, whereas stacked cells form stratified epithelia. Very few capillaries penetrate these tissues.
Glands are secretory tissues and organs that are derived from epithelial tissues. Exocrine glands release their products through ducts. Endocrine glands secrete hormones directly into the interstitial fluid and blood stream. Glands are classified both according to the type of secretion and by their structure. Merocrine glands secrete products as they are synthesized. Apocrine glands release secretions by pinching off the apical portion of the cell, whereas holocrine gland cells store their secretions until they rupture and release their contents. In this case, the cell becomes part of the secretion.
Review Questions
Q. In observing epithelial cells under a microscope, the cells are arranged in a single layer and look tall and narrow, and the nucleus is located close to the basal side of the cell. The specimen is what type of epithelial tissue?
A. columnar
B. stratified
C. squamous
D. transitional
- Answer
-
Answer: A
Q. Which of the following is the epithelial tissue that lines the interior of blood vessels?
A. columnar
B. pseudostratified
C. simple squamous
D. transitional
- Answer
-
Answer: C
Q. Which type of epithelial tissue specializes in moving particles across its surface and is found in airways?
A. transitional
B. stratified columnar
C. pseudostratified ciliated columnar
D. stratified squamous
- Answer
-
Answer: C
Q. The ________ exocrine gland stores its secretion until the glandular cell ruptures, whereas the ________ gland releases its apical region and reforms.
A. holocrine; apocrine
B. eccrine; endocrine
C. apocrine; holocrine
D. eccrine; apocrine
- Answer
-
Answer: A
Critical Thinking Questions
Q. The structure of a tissue usually is optimized for its function. Describe how the structure of individual cells and tissue arrangement of the intestine lining matches its main function, to absorb nutrients.
- Answer
-
A. Columnar epithelia, which form the lining of the digestive tract, can be either simple or stratified. The cells are long and narrow, which provide protection while still allowing for secretion and absorption.
Glossary
- anchoring junction
- mechanically attaches adjacent cells to each other or to the basement membrane
- apical
- that part of a cell or tissue which, in general, faces an open space
- apocrine secretion
- release of a substance along with the apical portion of the cell
- basement membrane
- in epithelial tissue, a thin layer of fibrous material that anchors the epithelial tissue to the underlying connective tissue; made up of the basal lamina and reticular lamina
- cell junction
- point of cell-to-cell contact that connects one cell to another in a tissue
- endocrine gland
- groups of cells that release chemical signals into the intercellular fluid to be picked up and transported to their target organs by blood
- endothelium
- tissue that lines vessels of the lymphatic and cardiovascular system, made up of a simple squamous epithelium
- exocrine gland
- group of epithelial cells that secrete substances through ducts that open to the skin or to internal body surfaces that lead to the exterior of the body
- gap junction
- allows cytoplasmic communications to occur between cells
- goblet cell
- unicellular gland found in columnar epithelium that secretes mucous
- holocrine secretion
- release of a substance caused by the rupture of a gland cell, which becomes part of the secretion
- merocrine secretion
- release of a substance from a gland via exocytosis
- mesothelium
- simple squamous epithelial tissue which covers the major body cavities and is the epithelial portion of serous membranes
- mucous gland
- group of cells that secrete mucous, a thick, slippery substance that keeps tissues moist and acts as a lubricant
- pseudostratified columnar epithelium
- tissue that consists of a single layer of irregularly shaped and sized cells that give the appearance of multiple layers; found in ducts of certain glands and the upper respiratory tract
- serous gland
- group of cells within the serous membrane that secrete a lubricating substance onto the surface
- simple columnar epithelium
- tissue that consists of a single layer of column-like cells; promotes secretion and absorption in tissues and organs
- simple cuboidal epithelium
- tissue that consists of a single layer of cube-shaped cells; promotes secretion and absorption in ducts and tubules
- simple squamous epithelium
- tissue that consists of a single layer of flat scale-like cells; promotes diffusion and filtration across surface
- stratified columnar epithelium
- tissue that consists of two or more layers of column-like cells, contains glands and is found in some ducts
- stratified cuboidal epithelium
- tissue that consists of two or more layers of cube-shaped cells, found in some ducts
- stratified squamous epithelium
- tissue that consists of multiple layers of cells with the most apical being flat scale-like cells; protects surfaces from abrasion
- tight junction
- forms an impermeable barrier between cells
- transitional epithelium
- form of stratified epithelium found in the urinary tract, characterized by an apical layer of cells that change shape in response to the presence of urine
Contributors and Attributions
OpenStax Anatomy & Physiology (CC BY 4.0). Access for free at https://openstax.org/books/anatomy-and-physiology