2.2: Otology Outreach Surgery in Developing Countries Under Local and Regional Anesthesia- Techniques and Pitfalls
- Page ID
- 15434
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
OTOLOGY OUTREACH SURGERY IN DEVELOPING COUNTRIES UNDER LOCAL & REGIONAL ANESTHESIA: TECHNIQUES & PITFALLS
Richard Wagner, Greg Torr
This chapter describes some techniques to safely perform middle ear and mastoid surgery in outreach ear surgery programs and discusses tips and pitfalls. It should be read in conjunction with the chapter: Local and regional anesthesia techniques for otologic (ear) surgery which provides a more detailed account of local anesthesia technique for ear surgery.
When surgeons travel to developing countries to do outreach ear surgery, they often lack the convenience of having a qualified anesthetist, trained recovery room staff, adequate monitoring equipment for safe general anesthesia, and are faced with long lines of patients requiring ear surgery. It is under such circumstances that ear surgery is ideally done under local or regional anesthesia.
Performing otology procedures under local, as opposed to general anesthesia has many advantages and can be described as “God’s Gift to Otology”. It allows one to perform middle ear surgery and monitor vestibulocochlear function without expensive (and often unavailable) equipment, along with reducing risks associated with general anesthesia.
It is critical that the surgeon has both the level of experience and comfort to perform middle ear surgery under local anesthesia with sedation. Although rather rare (<1% of cases), situations do arise when even an experienced surgeon must abandon an operation or convert from local to general anesthesia to complete the surgery.
Even qualified anesthetists may lack experience with using only a limited range of drugs to provide IV sedation. Under such circumstances it may be important that the surgeon assist the anesthetist to select the appropriate drugs that will provide sufficient hours of analgesia and sedation.
Caveat: Intravenous sedation can be a dangerous practice if performed without adequate monitoring or if the sedation practitioner is unfamiliar with the agents presented to him/her.
Rationale of ear surgery under local anesthesia with sedation
Safety: Patient safety is the priority when performing surgery. Safety of properly administered local anesthesia with intravenous sedation is well established providing that the attending surgeon have both the experience and confidence in the practice of local/regional anesthesia and sedation.
Reliability: As long as patients are selected according to the criteria listed below and reliable drugs are administered, the methods described provide a reliable alternative to general anesthesia in >90% of cases.
Anesthetic technique and safety: In developing countries there is a greater risk of anesthetic-related complications or deaths due to frequent use of non-physicians to administer anesthesia, inadequate monitoring equipment, and unreliable drugs. It is the surgeon’s responsibility to manage the operating theater and to lead the surgical team, which includes communicating with the anesthetist and agreeing on drugs to use to achieve adequate levels of anesthesia of sufficient duration.
Comorbidities: Unrecognized and untreated comorbidities can cause complications 2 and even deaths. In patients with known comorbidities, local anesthesia with sedation is a safer technique to employ.
Shorter recovery room time: Patients are essentially awake immediately after the surgery and go to the recovery room for observation to ensure that there is no rebound respiratory compromise and that vital signs are stable. Intravenous sedation therefore requires a shorter recovery room time than general anesthesia and patients are generally ready for discharge after being observed for 30 minutes.
Intraoperative monitoring of vestibular, cochlear and facial nerve function: A patient in a semiconscious state can respond to questions during surgery; hence the surgeon can assess the ossicular chain reconstruction intraoperatively. With stapes surgery, vestibular function can be ascertained and errors such as inserting a too long piston can be avoided. While removing bone from the facial ridge during canal wall down mastoidectomy, the facial nerve can be monitored by watching the face and by asking the patient to smile or open the eyes.
The Patient
Not all patients are suited to ear surgery under local anesthesia with IV sedation.
Age: Patients should be at least 18 years old to understand the concept of undergoing ear surgery while awake. Younger children tend to be too anxious and are less understanding. Older patients can cause problems as sedative drugs dosages need adjustment and a cautious titrated approach is advised to avoid excessive sedation.
Prior surgery: Patients who have had prior ear surgery frequently do not tolerate revision surgery under local anesthesia. This may be because fibrosis and scarring inhibit delivery of lidocaine to the surgical field to ensure adequate anesthesia.
Mental status: Very fearful or anxious patients, or those with underlying mental conditions are not considered ideal candidates.
Counseling and consent
Once a patient has been counseled about risks, benefits and surgical options, then administration of anesthesia is discussed. The surgeon counsels the patient about the diminished risks of local anesthesia compared to general anesthesia, and the benefits in terms of being able to monitor cochleovestibular function during surgery and to optimize hearing outcome.
Fasting
The patient should be starved for a minimum of 6 hours (adults) prior to surgery, even if general anesthesia is not anticipated.
Monitoring during middle ear surgery
Patients receiving IV sedation and local anesthesia for middle ear surgery need to be carefully monitored. A pulse oximeter, EKG machine, and blood pressure monitor need to be used. However, in developing countries there is often not a functioning anesthetic machine, there may not be inhalational agents, or monitoring equipment, trained anesthetists or nurse anesthetists.
Pulse oximetry: Pulse oximetry is critical to monitor blood oxygen saturation. Oxygen saturation should be maintained at 90- 100%. When supplemental oxygen is not available, careful monitoring is even more critical to avoid over-sedation, depressed breathing, hypoxia and hypercarbia. One may even have to assist ventilation with an Ambu bag. Treatment of low oxygen saturation with supplemental oxygen is only a short term solution and can mask a greater problem... that of hypoventilation and hypercarbia. If it is possible, rather communicate with the patient and encourage deep breathing maneuvers.
Blood pressure: Hypertensive patients require medication to make them normotensive. It occurs more commonly with patients who have undiagnosed hypertension and should be detected during preoperative medical screening. Hypertension can be severely exacerbated by systemic absorption of the adrenaline/epinephrine in the dental cartridges of Lignocaine/Lidocaine. In such cases consideration might have to be given to using local anesthetic without adrenaline/epinephrine, or to postpone surgery until the patient is normotensive.
EKG monitoring: The pulse and EKG tracing may reveal tachycardia following injection of epinephrine. The tachycardia is usually short-lived, and usually settles after 3-5 minutes. Alternatively, a gentle massage of the carotid artery may help. Rarely a short-acting beta-blocker can be administered.
Resuscitation equipment
Equipment for resuscitation in the event of an adverse reaction to any of the local anesthetics, sedatives and/or antibiotics must not only be present and in working order, but the practitioner needs to familiarize him/her with their use and function. These include a powerful suction machine and airway suction device e.g. Yankhauer sucker, a working laryngoscope (and spare bulbs and batteries), endotracheal tubes of appropriate sizes, and an Ambu bag.
Drugs
Emergency drugs that must be available include Adrenaline/Epinephrine, Atropine, steroids and antihistamines.
Drugs are employed to achieve analgesia such that patients do not feel pain and to achieve sedation such that they are less aware of the surgery and anxiety is minimal. You have to plan to have the correct drugs available to use, or adapt your anesthetic technique to the drugs that are available.
Lidocaine (1% or 2%) is appropriate for local analgesia. Its analgesic effect lasts 2-4 hours (majority of middle ear surgeries take 98% of cases, which is well below the maximum adult dose of lidocaine of 7 mg/kg.
Adrenaline (epinephrine) provides hemostasis and a dry surgical field. Half a ml (half an ampoule) of adrenaline 1:1000 is added to 9 mL of lidocaine drawn up into a 10 mL syringe to achieve a concentration of lidocaine:epinephrine of 1:30,000. It is well tolerated by patients; although rarely a patient might develop tachycardia which usually subsides within <5 minutes.
Systemic analgesia is administered intravenously in combination with the injection of lidocaine & epinephrine, e.g. Fentanyl, morphine sulphate, or Meperidine (Demerol). With all systemic analgesics it is imperative to monitor the patient’s breathing and oxygen saturation. The choice of intravenous analgesic often depends on its availability. Because the 1st author most frequently encounters fentanyl on his travels, it is his 1st-line agent. In the average person weighing 130-150 lbs (59- 68 kg), he starts by titrating 50 µg of fentanyl. A further 50 bolus can be given if the patient tolerates this well without hypoventilation. For patients with a body mass closer to 200 pounds (91 kg) he uses up to 125-150 µg of fentanyl (titrated). In countries like American Samoa where the body mass index is of the highest in the world, it is not unusual to administer up to 300 µg of Fentanyl. With Demerol, the author generally administers about 75 mg for an average sized person; for morphine sulfate, he administers 7.5-10 mg.
Benzodiazepines are used to reduce anxiety. The author generally uses diazepam (valium) or Midazolam (Versed). The author prefers diazepam because of its slower onset and longer action. Diazepam is however frequently not available, while Midazolam is generally available in developing countries. Midazolam has a much more rapid induction and shorter duration of action but has a higher risk of respiratory depression.
Note that a combination of Benzodiazepines and Opioids can be additive, especially in patients that are drug/medication-naïve. Caution should be exercised when administering these medications and a titrated approach is advised, starting with smaller doses and working up to those stated above.
Reversal agents: It is strongly advised that the operator familiarizes him/herself with Opioid and Benzodiazepine reversal agents and their use and doses in the event of over-sedation.
- Naloxone: 1 ampoule = 0.4 mg. Dilute into 4 mL with saline and titrate 1 mL/0.1 mg IVI every 2-3 minutes until the patient recovers consciousness and (airway) reflexes.
- Flumazenil: Comes as a 0.1 mg/mL preparation. Dosage 0.2mg IVI titrated every 2 minutes until consciousness is regained.
- Overdosing with either of these drugs can cause hypertension and severe pain.
Microscopes

Figure 1: Older model Zeiss (OPMI-1) operating microscope with incandescent bulb

Figure 2: OPMI-1 incandescent light bulb
In many developing countries it is difficult to secure a functioning operating microscope. Frequently we find an old Zeiss microscope that uses an incandescent light bulb (Figures 1, 2). One should enquire what microscope is to be used and ensure that spare light bulbs are available or bring light bulbs along. Even though these microscopes work well, the light intensity is poor when compared to new microscopes.
The objectives should be 10x power and a 250 mm lens is preferred. A 300 or 200 mm lens can also be used as long as one refocuses the eyepieces to their limits to adjust for the best depth of field. To provide live video for teaching one should take along a beam splitter; video adapter; C-mount coupler; video camera, and appropriate video cables. The camera is attached to a computer monitor or TV depending on the output connection. (VGA, HDMI, DVI, S-video) (Figure 3). It is therefore important to contact your host to find out what monitors are available.
Endoscopic ear surgery
The author favors the microscope, but endoscopic surgical techniques may have advantages for middle ear surgery in outreach settings as the equipment is compact and portable. See chapter: Endoscopic cholesteatoma, tympanoplasty and middle ear surgery. However, one requires a very cooperative patient as the head has to be kept very still throughout the procedure to avoid the endoscope injuring the ear should the head suddenly move. It should also be noted that patients in developing countries usually have much more advanced ear disease because the diagnoses are usually delayed. Therefore, especially in patients with cholesteatoma, a canal-walldown modified or radical mastoidectomy is generally preferred and is performed easier with a microscope than an otoscope.
Operating room setup and positioning (Figure 3)

Figure 3: Operating room setup & camera system
Sterilizing surgical instruments
Depending on what is available in the country one is visiting, instruments may be sterilized by a variety of methods e.g. autoclaving with steam vapor; or soaking instruments in alcohol, “cidex” or in acetone. Irrespective of the sterilization technique, instruments should be rinsed in a sterile saline solution before use.
Surgical equipment
The instruments listed below are the author’s preference and are adequate to allow one to perform tympanoplasty, mastoidectomy, canalplasty, temporal bone resection, and other middle ear surgeries.
| Knife handle |
| Weitlaner self-retaining retractors (2) |
| Adson forceps w/ teeth |
| Iris scissors curved |
| Iris scissors straight |
| Senn retractor |
| Joseph Skin Hook, 2 prong |
| Beckmann nasal speculum |
| Suction tips 10, 14, 18 ,20 F |
| House double-ended large spoon curette sizes 2 x 3.2 mm & 1.6 x 2.6 mm |
| Freer elevator |
| Ear speculum 4, 5, 6, 7, 8 mm |
| Bellucci scissors |
| Hartmann forceps |
| Malleus nipper |
| Cup forceps |
| Cutting block |
| Needle holder |
| Suture scissors |
| Round knife 2.5 & 1.0 mm |
| Annulus elevator |
| Rosen pick |
| Fish rasp (right & left) |
| Sickle knife |
| 45o pick |
Table 1: List of ear instruments required
Audiology
It is imperative that all patients have an audiogram done before ear surgery. It should ideally be done by someone trained to test hearing, because an untrained tester will e.g. not understand how to mask and will therefore get erroneous results.
Surgical steps of middle ear surgery under local anesthesia with sedation
A time window of 1-2 hours should be available to complete surgery by using 5-9 mL of local anesthetic solution and a titrated intravenous dose of up to 150 ug of fentanyl or up to 10 mg of morphine. Should a patient require more sedation or analgesia during surgery, either drug can be given depending on the needs.
Induce IV analgesia and sedation
- Administer IV analgesia & sedation (Fentanyl & valium as described above)
- Wait for the drugs to take effect (within 5 minutes)
- Assess that adequate sedation has been achieved by asking the patient to respond to simple questions or commands (e.g. “squeeze my hand”)
- Note: If the eyelid reflex is lost the patient is too deeply sedated and is bordering on general anesthesia!
- The patient should be rousable by speech or gentle touch.
- Proceed to injecting local anesthesia
Auricular block
- Mix 0.5 mL (half ampoule) of adrenaline 1:1000 and 9 mL of lidocaine in a 10 mL syringe
- Use a 27-gauge needle (small gauge causes less pain and tissue trauma)
- Start injecting the local anesthetic
- Note any pain reaction from the patient
Three sites are injected to achieve an adequate ear block
1. Postauricular injection
- Begin infiltrating at the level of the external auditory canal

Figure 4: Begin infiltrating at level of external auditory canal
- Slowly inject about 0.5 mL of local anesthetic to form a small blister under the skin (Figure 4)
- Rotate the needle superiorly and advance it under the skin to the top of the helix
- Inject 2-3 mL solution while slowly advancing the needle inferior to the site of the original blister; as this is done, the area of infiltration should puff up
- Using the initial injection site, insert the needle under the concha so that the tip is close to the external auditory canal skin at the level of the spine of Henle

Figure 5: Infiltrate local ana=esthetic in a radial fashion
- Infiltrate local anesthetic in a radial fashion approximately 3 times, infiltrating 1-1.5 mL of anesthetic (Figure 5)
2. Intracanal injection (Figures 6a, b)

Figure 6a: Canal injection

Figure 6b: Axial view of canal injection
- Insert the largest ear speculum that fits into the ear canal, and view the canal with the operating microscope
- Infiltrate the canal skin with 3 to 4 injections of solution; each injection is 0.25-0.40 mL
- Initiate the 1st injection at the junction of the medial 1/3 of the canal lacking appendages, and the lateral 2/3 at the 9 o’clock position where there is hair and subcutaneous tissue.
- Commence the injection at the level of the most medial hair cells
- Then advance the needle a few millimeters onto the bone with its bevel down before infiltrating
- As the infiltration is done, blanching of the stria vascularis is seen
- Commence the 2nd injection at a 12 o’clock position
- Commence the 3rd injection at a 6 o’clock position
- The 6 and 12 o’clock injections provide anesthesia for the canal cuts that are made when elevating the conchomeatal flap
3. Preauricular injection (Figure 7)
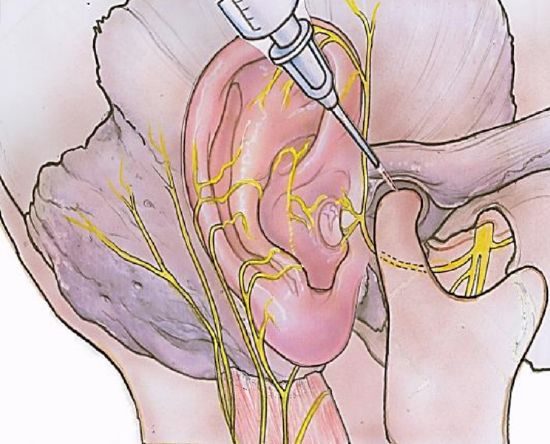
Figure 7: Preauricular injection to block the auriculotemporal nerve
- This injection provides anesthesia to the anterior canal, which is supplied by the auriculotemporal division of the trigeminal nerve
- Insert the needle at a 45o angle in front of the tragus
- Advance the needle towards the angle of the mandible
- Commence infiltration after the needle has reached its maximum depth and inject 0.5-0.75 mL solution as the needle is advanced outward
Middle ear surgery technique
It is critical that a surgeon performing ear surgery has both the experience and comfort to perform middle ear surgery under local anesthesia with IV sedation. Under ideal circumstances an experienced ear surgeon is able to perform tympanoplasty (underlay or overlay), stapes surgery, modified or radical mastoid surgery, lateral temporal bone resection, and even endolymphatic sac decompression under IV sedation and local anesthesia.
Consumables checklist for outreach surgery
- 4/0 Monocryl sutures
- Gelfoam (Johnson & Johnson)
- Xeroform gauze
- Quinolone antibiotic solution
- Silastic sheeting - I use surgical gloves
- Kerlix gauze bandages (3 or 4”)
- Syringes
- Needles
- Lidocaine
- Adrenaline
- Systemic analgesic
- Analgesics for postoperative pain relief
Cleaning solutions
Microscope and audiovisual equipment: Check on available microscope and spare bulbs
ENT clinic equipment
- Tuning forks
- Jobson-Horne
- Otoscopes
- Suture scissors
- Etc.
Ear surgery instrumentation
Pearls & Pitfalls
- Critical to carefully select patients
- Preoperative audiogram imperative (unless impossible to obtain)
- It is important to monitor patients during surgery with EKG, oximeter, and blood pressure monitor
- More important is a human monitor. If a qualified anesthetist is not available, then either the surgeon (yourself) or a trusted nurse must watch the patient and monitor and encourage him/her to breathe deeply when needed.
- Inject atraumatically using the smallest needle possible, but no smaller than a 27-gauge, keeping the bevel facing down
- Be sure that the drugs that you are using are not fake or adulterated; I have frequently encountered such medications in developing countries that do not function properly
- When you notice a patient becoming more awake, notify the anesthetist
- If the patient experiences pain while operating in the middle ear, irrigate the middle ear down the canal with 2 mL of 1-2% lidocaine without epinephrine, leaving it in the middle ear for 2 minutes before suctioning it out
- If mucosal bleeding from the middle ear persists, irrigate the middle ear with 2 mL pure epinephrine down the canal and leave it there for 2 minutes before suctioning it from the middle ear cleft
- Be prepared to handle any and all complications you may encounter, such as repairing a CSF leak, and repairing the facial nerve if injured
- Power failures are common in some developing countries, especially in rural settings, and should be anticipated. If the drill stops functioning / power fails after a mastoidectomy has been commenced, then the surgeon may have to resort to a hammer and gouge technique to compete the surgery: See chapters: Hammer and gouge for cholesteatoma; Hammer and gouge for acute mastoiditis
Pointers for teams planning outreach surgery in resource limited countries
When the author works in developing countries, his visits are coordinated through an NGO, a local doctor or through a medical society. Irrespective of who is the host, it is imperative that the following rules be followed:
- The primary goal should be to share knowledge and skills by teaching local doctors about ear disease and surgery
- Arrange for local doctors to schedule patients and manage follow up
- If there is no local ENT doctor to participate in the program, it is imperative that one identifies another doctor to take responsibility for postoperative care, using telemedicine for advice
- In the absence of a microscope one may be required to bring along a portable operating microscope
- In the absence of a locally based microscope it is impossible for the local doctor to do microscopic post-operative ear care. In such cases the surgery must be tailored in such way to make it possible for the local doctor to manage ears postoperatively without a microscope:
- With tympanoplasty, pack the ear canal with resorbable Gelfoam; with a modified meatoplasty, place gauze e.g. Xeroform in the lateral canal and instruct the doctor to remove the gauze at 10-12 days and then begin placing Ciprofloxacin eardrops (5 gtts bid) over the Gelfoam and to wait 3-4 weeks before doing otoscopy to ensure healing has occurred
- When performing canal-wall-down open cavity mastoidectomy, the author places temporalis fascia over the reconstructed area, then Gelfoam. This is followed by a strip of surgical glove which serves as an inert barrier so that when the doctor subsequently removes the gauze from the mastoid cavity, the surgical reconstruction is not disrupted. Once the gauze and strip of glove are removed, ciprofloxacin eardrops (5 gtts bid) are placed over the Gelfoam. Otoscopy is performed 3-4 weeks later to ensure healing has taken place
6. It is imperative to continue to communicate with the doctor who is managing the patients postoperatively, also to advise how to manage delayed complications such as swelling, discharge, facial paralysis, vestibular dysfunction, or hearing loss. The author does this through Skype, although other platforms such as FaceTime, Viber etc. can be used
Wishing to do otology outreach surgery?
Visit the following webpage to team up with established outreach programmers: http://www.entdev.uct.ac.za/support/
Recommended reading
- Local and regional anesthesia techniques for otologic (ear) surgery
- Endoscopic cholesteatoma, tympanoplasty and middle ear surgery
- Hammer and gouge for cholesteatoma
- Hammer and gouge for acute mastoiditis
- ENT Outreach in Africa: Rules of Engagement
Authors
Richard Wagner MD, FACS
Director
Global ENT Outreach
Coupeville, WA, 98239, USA
rwagner@geoutreach.org
Greg Torr MBChB, FCA (SA)
Anesthetist
Cape Town, South Africa
gregtorr@mweb.co.za
Editor
Johan Fagan MBChB, FCS(ORL), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za


