12.6: Spinal Cord and Spinal Nerves
- Page ID
- 35889
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)By the end of this section, you will be able to:
- Describe the structures that protect and supply the spinal cord
- Describe the structures of the spinal cord and their functions
- Explain the arrangement of gray and white matter in the spinal cord
- Compare and contrast how white and gray matter process information
- Describe the sensory and motor components of spinal nerves and the plexuses that they pass through
- Explain what a dermatome is and its clinical significance
The spinal cord is continuous with the brain and transmits sensory information from the periphery of the body to the brain, and motor information from the brain to the periphery. It is also a center for coordination of reflexes, as well as control of reflexes independently from the brain. Along the spinal cord, spinal nerves emerge that carry both sensory and motor information.
Protective Coverings of the Spinal Cord
The spinal cord, as the brain, is protected by meninges, which are continuous with the cranial meninges. From outermost to innermost, the spinal meninges are: dura mater, arachnoid mater and pia mater. The spinal meninges are similar to the cranial ones, except for the dura mater. The spinal dura mater consists of a single layer of connective tissue, differing from the cranial dura mater. Moreover, at each intervertebral foramen, the dura mater extends and fuses with the connective tissue that covers spinal nerves.
One space between the spinal meninges also differs slightly from the ones present around the brain. The epidural space between the periosteum and dura mater is a real space around the spinal cord and houses areolar and adipose connective tissues, and blood vessels (shown in Figure \(\PageIndex{2}\)). Epidural anesthesia is injected in this space. The subarachnoid space is filled with circulating CSF, which also provides a liquid cushion to the brain and spinal cord. Similar to clinical blood work, a sample of CSF can be withdrawn to find chemical evidence of neuropathology or metabolic traces of the biochemical functions of nervous tissue. Because the spinal cord does not extend through the lower lumbar region of the vertebral column, a needle can be inserted through the dura and arachnoid layers to withdraw CSF. This procedure is called a lumbar puncture and avoids the risk of damaging the central tissue of the spinal cord.
Blood Supply to the Spinal Cord
The spinal cord is supported by an extensive collateral supply and drainage of blood. Three longitudinal spinal arteries supply the anterior and posterior regions of the spinal cord. The anterior and posterior spinal arteries are connected by cross-connections of pia mater called the arterial vasocorona which encircles the cord and supplies the lateral portion of the spinal cord. The blood supply is reinforced by numerous arteries that pass through the intervertebral foramina and divide into anterior and posterior radicular arteries and have variable connections with the spinal arteries. Numerous veins and venous plexuses surround the spinal cord and drain the blood from it. These veins share the same names as the arteries that supply the spinal cord.
Spinal Cord
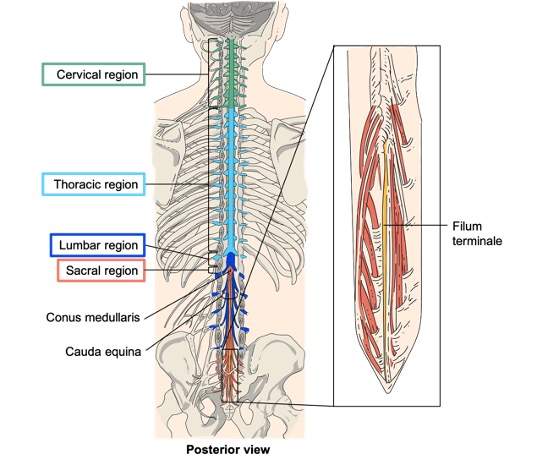
The description of the CNS is concentrated on the structures of the brain, but the spinal cord is another major organ of the system. The length of the spinal cord is divided into regions that correspond to the regions of the vertebral column. As shown in Figure \(\PageIndex{1}\), immediately inferior to the medulla oblongata is the cervical region of the spinal cord that contains motor neurons whose axons, together with sensory axons, extend into cervical spinal nerves. Inferior to the cervical region is the thoracic region, that contains neurons for the thoracic spinal nerves. The lumbar region is a short segment that contains neurons for the lumbar spinal nerves. Finally the sacral region contain neurons for the sacral nerves. The spinal cord is not the full length of the vertebral column because the spinal cord does not grow significantly longer after the first or second year, but the skeleton continues to grow. For this reason, the names of the spinal cord regions and vertebral regions to not match up. The lumbar and sacral spinal cord segments are found between vertebral levels T9 and L2. The spinal cord ends around the L1/L2 vertebral level, forming a tapered structure known as the conus medullaris, which corresponds to the sacral spinal cord. The nerves that emerge from the spinal cord pass through the intervertebral foramina at the corresponding vertebral segments. For example, lumbar nerves exit the vertebral canal at the respective lumbar vertebrae. As the vertebral column grows, these nerves grow with it and result in a long bundle of nerves inferior to the conus medullaris that resembles a horse’s tail and therefore is named the cauda equina. Within the cauda equina, there is a thin strand of pia mater called filum terminale that helps anchoring the conus medullaris to the coccyx. At each intervertebral foramen, the spinal dura mater extends between vertebrae and surrounds the spinal nerves.
The spinal cord has a diameter of approximately 3/4 of an inch (just less than 2 cm) and its length ranges between 16 to 18 inches (41-45 cm). However, its diameter changes between the different regions because the ratio of white and gray matter changes to reflect the functions of the different regions. The cervical and lumbar regions of the spinal cord show a larger diameter compared to the rest of the regions. The cervical enlargement and lumbar enlargement represent an increased amount of neurons in the gray matter and axons in the white matter that serve the upper limbs and lower limbs, respectively.
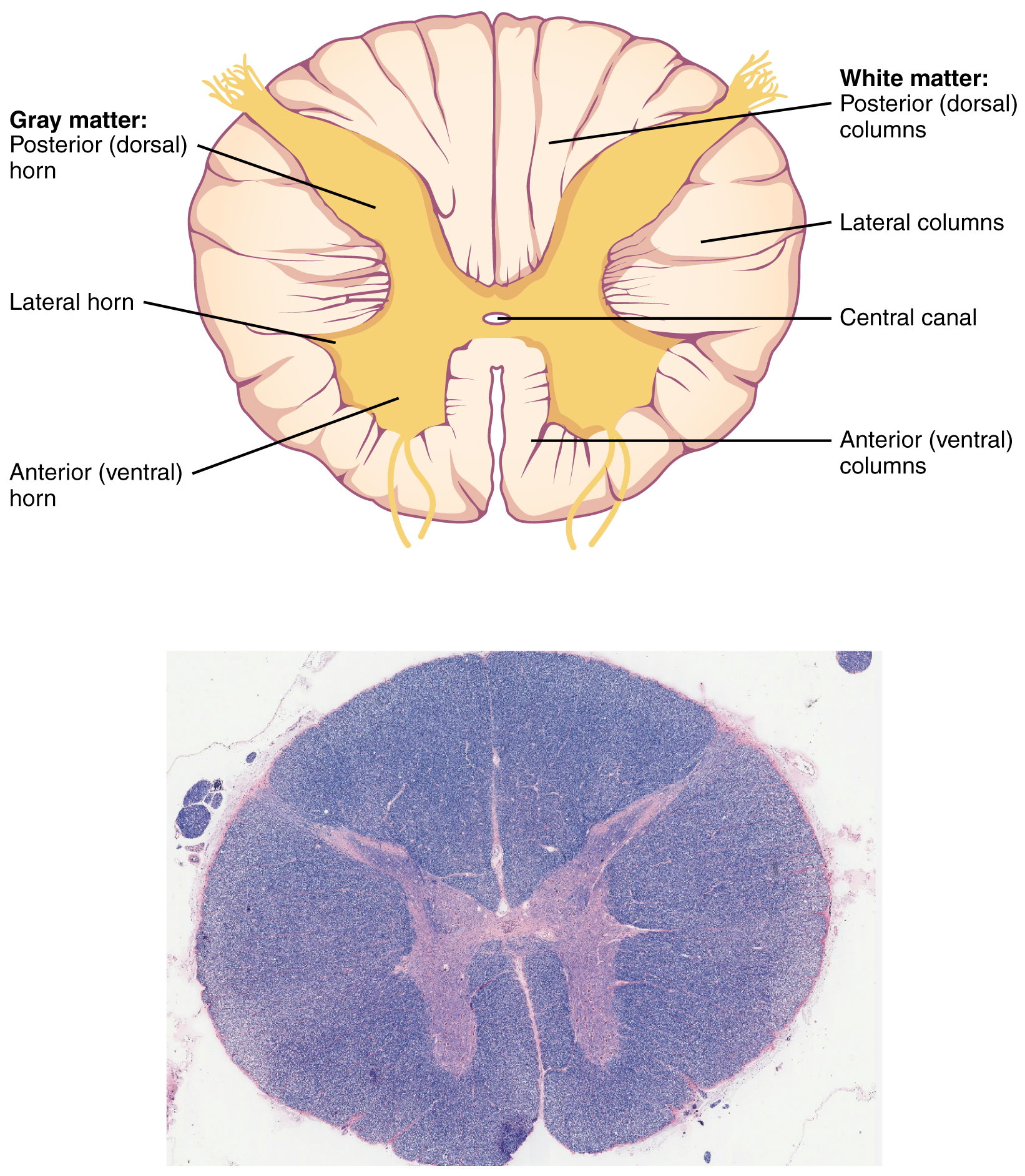
Whereas the brain develops out of expansions of the neural tube into primary and then secondary vesicles, the spinal cord maintains the tube structure and is only specialized into certain regions. As the spinal cord continues to develop in the newborn, anatomical features mark its surface. Viewed in cross section, the anterior midline is marked by the anterior median fissure, and the posterior midline is marked by the posterior median sulcus. As shown in Figure \(\PageIndex{2}\), axons coming from the dorsal (posterior) root ganglion enter the posterior side through the dorsal (posterior) nerve root, which marks the posterolateral sulcus on either side. The axons emerging from the anterior side do so through the ventral (anterior) nerve root. Note that it is common to see the terms dorsal (dorsal = “back”) and ventral (ventral = “belly”) used interchangeably with posterior and anterior, particularly in reference to nerves and the structures of the spinal cord. You should learn to be comfortable with both. The posterior and anterior nerve roots fuse together to form the spinal nerves. In the central region of the spinal cord, a central canal is the continuation of the fourth ventricle of the brain and contains cerebrospinal fluid (CSF).

On the whole, the posterior regions are responsible for sensory functions and the anterior regions are associated with motor functions. This comes from the initial development of the spinal cord, which is divided into the basal plate and the alar plate. The basal plate is closest to the ventral midline of the neural tube, which will become the anterior face of the spinal cord and gives rise to motor neurons. The alar plate is on the dorsal side of the neural tube and gives rise to neurons that will receive sensory input from the periphery.
Gray Horns
In cross-section, the gray matter of the spinal cord has the appearance of an ink-blot test, with the spread of the gray matter on one side replicated on the other—a shape reminiscent of a bulbous capital “H.” As shown in Figure \(\PageIndex{3}\), the gray matter is subdivided into regions that are referred to as horns. The posterior horn is responsible for sensory processing and contain the axons of sensory neurons and the cell bodies of interneurons. The axons of sensory neurons are bundled into the posterior nerve root and are coming directly from the posterior root ganglion which contains cell bodies of sensory neurons. The lateral horn, which is only found in the thoracic, upper lumbar, and sacral regions, is a central component of the autonomic nervous system and contains cell bodies of autonomic motor neurons which innervate cardiac muscle, smooth muscle and glands.The anterior horn contains the cell bodies of somatic motor neurons that control skeletal muscles. The somatic motor neurons are the largest neurons of the body and are classified as multipolar neurons. The fibers that cause contraction of skeletal muscles are the axons of these neurons, which exit the spinal cord through the anterior nerve root. The posterior and anterior nerve roots fuse to form the spinal nerve, which contains mixed sensory and motor information.The motor neuron that causes contraction of the big toe, for example, is located in the sacral spinal cord. The axon that has to reach all the way to the belly of that muscle may be a meter in length. The neuronal cell body that maintains that long fiber must be quite large, possibly several hundred micrometers in diameter, making it one of the largest cells in the body. The neurons of the spinal cord are organized into functional groups called nuclei representing their respective functions (somatic sensory, visceral sensory, somatic motor and autonomic motor). Surrounding the central canal, a horizontal line of gray matter called the gray commissure connects the left and right sides of the spinal cord.
White Columns
Just as the gray matter is separated into horns, the white matter of the spinal cord is separated into columns. Ascending tracts of nervous system fibers in these columns carry sensory information up to the brain, whereas descending tracts carry motor commands from the brain. Looking at the spinal cord longitudinally, the columns extend along its length as continuous bands of white matter. Between the two posterior horns of gray matter are the posterior columns. The posterior columns are composed of axons of ascending tracts. Between the two anterior horns, and bounded by the axons of motor neurons emerging from that gray matter area, are the anterior columns. The white matter on either side of the spinal cord, between the posterior horn and the axons of the anterior horn neurons, are the lateral columns. The anterior and lateral columns are composed of many different groups of axons of both ascending and descending tracts—the latter carrying motor commands down from the brain to the spinal cord to control output to the periphery. The anterior columns are connected by a bundle of axons called white commissure that crosses the central region of the spinal cord.
Dorsal Root Ganglion
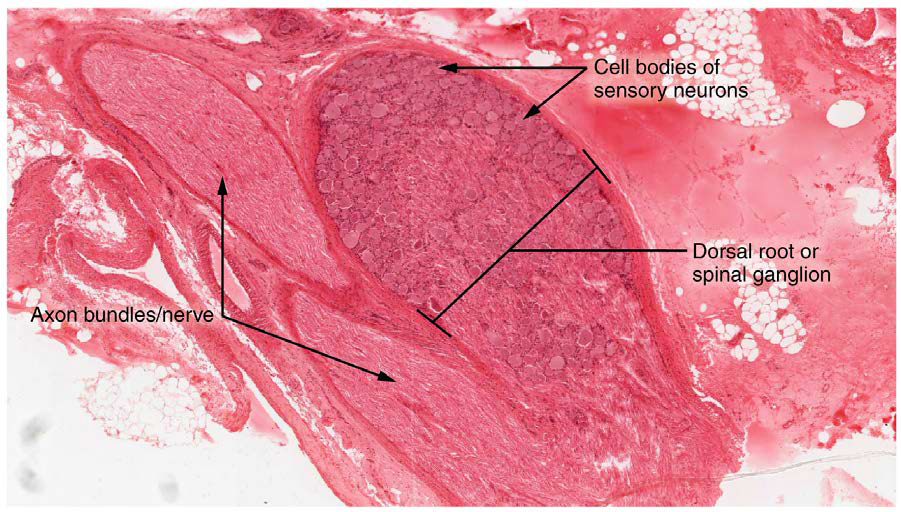
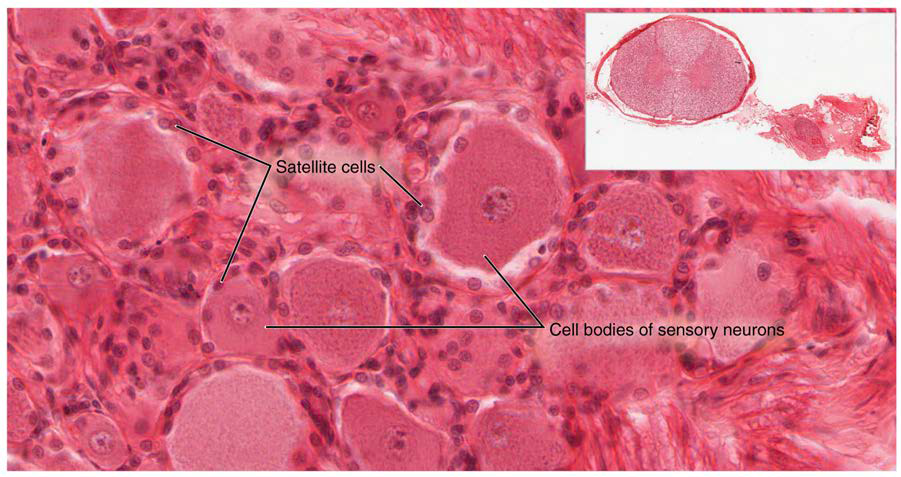
A ganglion (ganglia for plural) is a group of neuron cell bodies in the peripheral nervous system. Ganglia can be categorized, for the most part, as either sensory ganglia or autonomic ganglia, referring to their primary functions. The most common type of sensory ganglion is a dorsal (posterior) root ganglion. These ganglia are the cell bodies of neurons with axons that are sensory endings in the periphery, such as in the skin, and that extend into the CNS through the dorsal nerve root. The ganglion is an enlargement of the nerve root. Under microscopic inspection, it can be seen to include the cell bodies of the neurons, as well as bundles of fibers that are the posterior nerve root (Figure \(\PageIndex{4}\)). The cells of the dorsal root ganglion are unipolar cells. Also, the small round nuclei of satellite cells can be seen surrounding—as if they were orbiting—the neuron cell bodies (Figure \(\PageIndex{5}\)).
Spinal Nerves
The nerves connected to the spinal cord are the spinal nerves. The arrangement of these nerves is much more regular than that of the cranial nerves. All of the spinal nerves are combined sensory and motor axons that separate into two nerve roots. The sensory axons enter the spinal cord as the dorsal nerve root. The motor fibers, both somatic and autonomic, emerge as the ventral nerve root.
There are 31 spinal nerves, named for the level of the spinal cord at which each one emerges. There are eight pairs of cervical nerves designated C1 to C8, twelve thoracic nerves designated T1 to T12, five pairs of lumbar nerves designated L1 to L5, five pairs of sacral nerves designated S1 to S5, and one pair of coccygeal nerves. The nerves are numbered from the superior to inferior positions, and each emerges from the vertebral column through the intervertebral foramen at its level. The first nerve, C1, emerges between the first cervical vertebra and the occipital bone. The second nerve, C2, emerges between the first and second cervical vertebrae. The same occurs for C3 to C7, but C8 emerges between the seventh cervical vertebra and the first thoracic vertebra. For the thoracic and lumbar nerves, each one emerges between the vertebra that has the same designation and the next vertebra in the column. The sacral nerves emerge from the sacral foramina along the length of that unique vertebra.
Spinal nerves extend outward from the vertebral column to innervate the periphery. The nerves in the periphery are not straight continuations of the spinal nerves, but rather the reorganization of the axons in those nerves to follow different courses. Axons from different spinal nerves will come together into a systemic nerve. This occurs at four places along the length of the vertebral column, each identified as a nerve plexus, whereas the other spinal nerves directly correspond to nerves at their respective levels. In this instance, the word plexus is used to describe networks of nerve fibers with no associated cell bodies.
After exiting the intervertebral foramen, each spinal nerve splits into two branches called rami (ramus for singular) (Figure \(\PageIndex{6}\)). On the posterior side, the dorsal ramus is a short nerve that innervates the deep muscle and skin of the back. On the anterior side, the ventral ramus splits into multiple branches that eventually can form nerve plexuses. The ventral ramus innervates the anterior and lateral portions of the trunk, the upper and the lower limbs. Spinal nerves are also associated with other branches called rami communicantes which are formed by the gray and white rami and connect the spinal nerve to the autonomic ganglia.
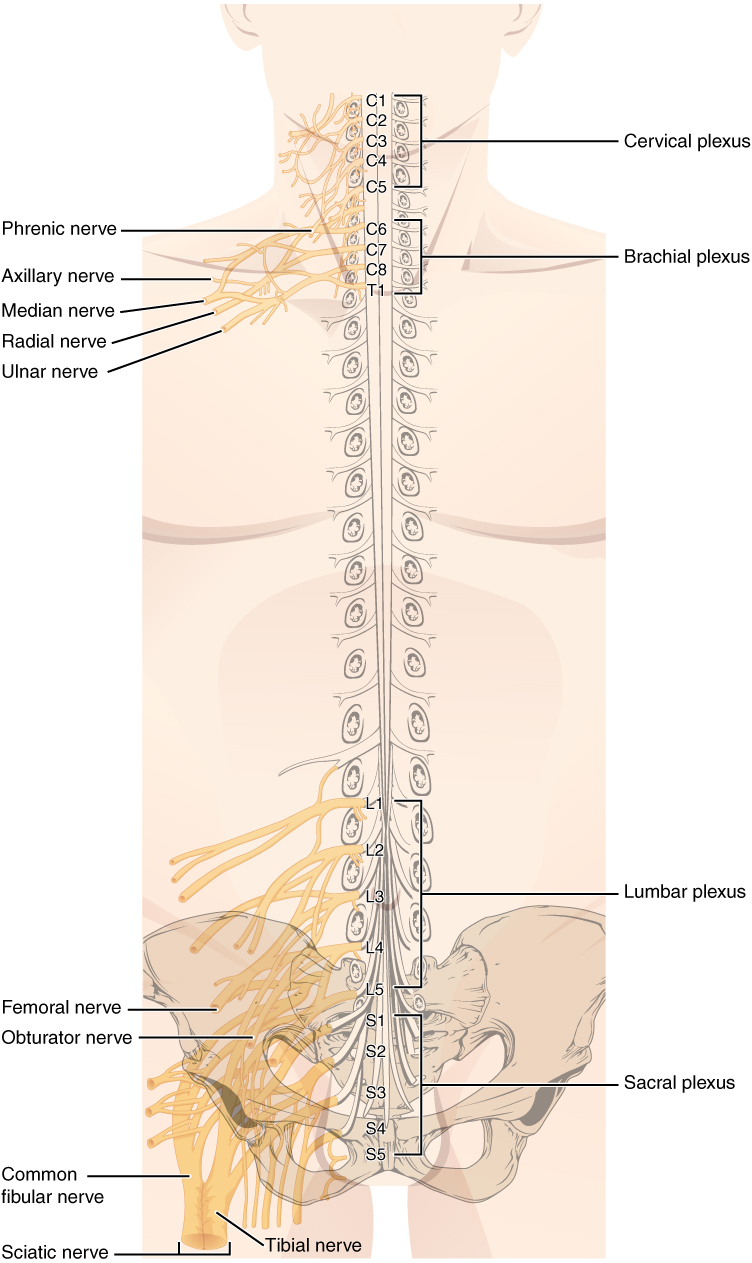
Of the four nerve plexuses, two are found at the cervical level, one at the lumbar level, and one at the sacral level (Figure \(\PageIndex{7}\)). The cervical plexus is composed of axons from spinal nerves C1 through C5 and branches into nerves in the posterior neck and head, as well as the phrenic nerve, which connects to the diaphragm at the base of the thoracic cavity.
The other plexus from the cervical level is the brachial plexus. Spinal nerves C5 through T1 reorganize through this plexus to give rise to the nerves of the arms, as the name brachial suggests. The ventral rami of the brachial plexus rearrange to form the superior, middle and inferior trunks. At the clavicle, the trunks split into an anterior division and posterior division, which innervate the anterior and posterior parts of the upper limbs, respectively. At the axilla, the divisions converge to form the posterior, medial and lateral cords. Finally, the cords split into five terminal branches: the axillary, median, musculocutaneous, radial and ulnar nerves. The axillary nerve innervates the deltoid and teres minor muscles, and receives sensation from the superolateral side of the arm. The median nerve innervates the most anterior forearm muscles as well as muscles that move the thumb. It receives sensation from the palmar region and dorsal tips of the lateral 3 and a half digits. The musculocutaneous nerve innervate the anterior arm muscles and receives sensation from the lateral region of the forearm. The radial nerve innervates muscles and receives sensation from the posterior arm and forearm, including the dorsal region of the lateral three digits (not including their tips). The ulnar nerve innervates anterior forearm muscles as well as intrinsic hand muscles. It receives sensation from the dorsal and palmar regions of the medial one and a half digits.
The lumbar plexus arises from all the lumbar spinal nerves (L1 to L5) and gives rise to nerves innervating the pelvic region and the anterior leg. The femoral nerve is one of the major nerves from this plexus, which gives rise to the saphenous nerve as a branch that extends through the anterior lower leg. The femoral nerve innervates anterior thigh muscles and receives sensory information from the anterior and medial aspects of the thigh.
The sacral plexus comes from the lower lumbar nerves L4 and L5 and the sacral nerves S1 to S4. The most significant systemic nerve to come from this plexus is the sciatic nerve, which is a combination of the tibial nerve and the fibular nerve. The sciatic nerve extends across the hip joint and is the largest and longest nerve of the body. Through the tibial and fibular nerves, the sciatic nerve innervates the muscles and receives sensation of the posterior thigh and lower leg. It is most commonly associated with the condition sciatica, which is the result of compression or irritation of the nerve or any of the spinal nerves giving rise to it.
Spinal nerves of the thoracic region, T2 through T11, are not part of the plexuses but rather emerge and give rise to the intercostal nerves found between the ribs, which articulate with the vertebrae surrounding the spinal nerve. The intercostal nerves innervate the intercostal muscles and receive sensation from the skin of the anterior and lateral sides of the thoracic region. The last nerves (T7 to T12) also innervate the abdominal muscles and their overlying skin.
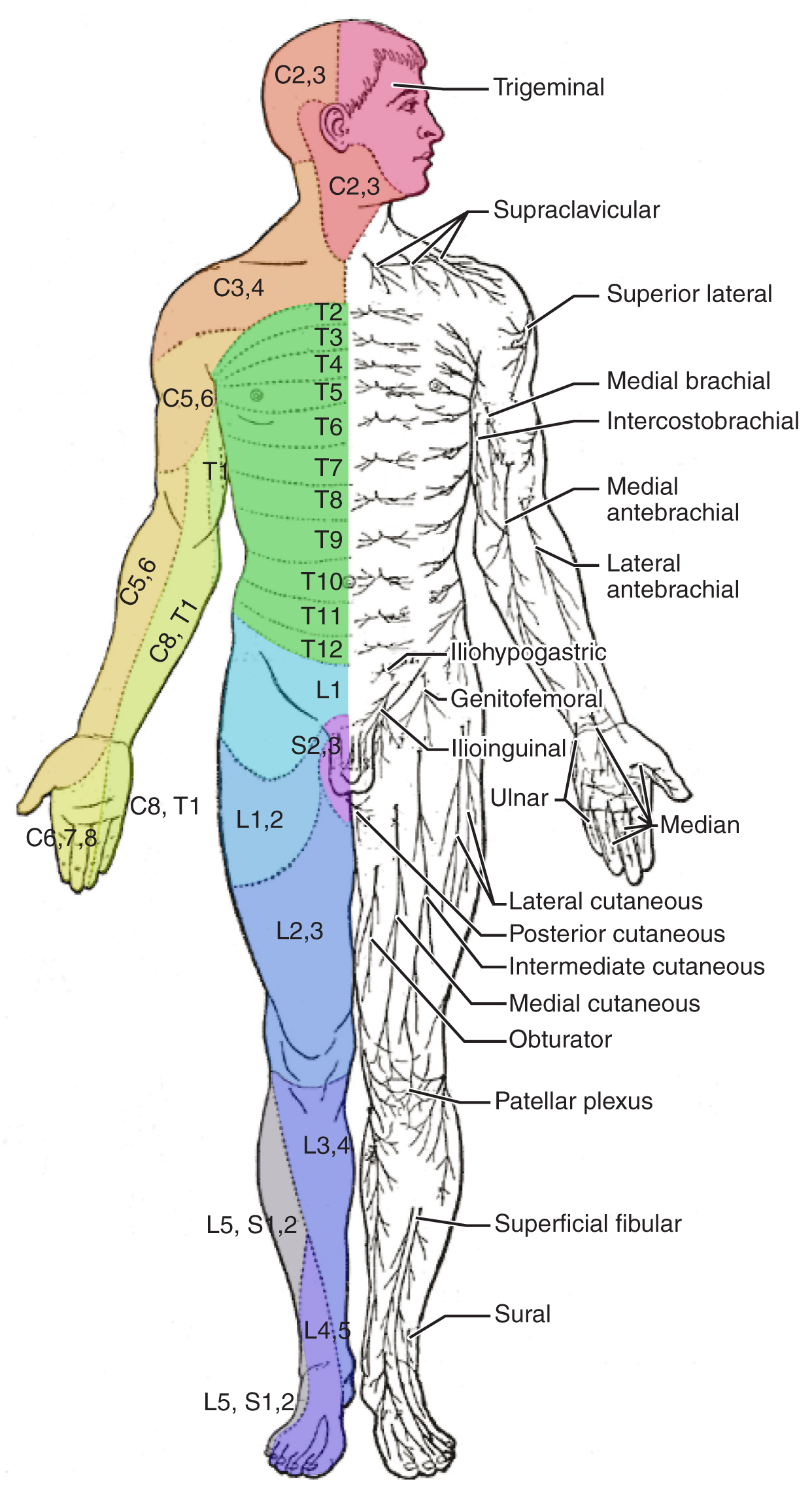
Dermatomes
The spinal nerves, which contain sensory fibers with endings in the skin, connect with the skin in a topographically organized manner, illustrated as dermatomes (Figure \(\PageIndex{8}\)). For example, the fibers of eighth cervical nerve innervate the medial surface of the forearm and extend out to the fingers. All spinal nerves except C1 innervates a region on the skin. Dermatomes are important in a clinical setting as they can help identify potential damage to spinal nerves. In a sensory exam, the dermatome of a specific area is tested for sensation (for example the stroking of a cotton ball) to evaluate the functioning of the spinal nerve connected to that dermatome. Dermatomes are also associated with referred visceral pain, as the spinal nerves innervated the regions of the skin also innervate internal organs. Pain from the internal organ can then be mistakenly referred to a dermatome. For example, myocardial infarction is perceived as referred pain in the chest, left shoulder and left arm. This is because the sensory fibers that innervate the cardiac tissue travel through the T1-T4 spinal nerves, which also innervate the medial and anterior side of the body.
Concept Review
The spinal cord is covered and protected by the spinal meninges, similar to the cranial ones. However, the spinal dura mater presents only one layer of tissue. Moreover, the epidural space is a real space that houses areolar and adipose connective tissues, and blood vessels.
The spinal cord is divided into segments that take the same name as the vertebral regions. However, the sacral spinal cord ends at the vertebral lumbar level (L1/L2) with the conus medullaris, while the spinal nerves continue exiting at their respective region of the vertebral column. Inferior to the conus medullaris, the spinal nerves form a bundle called the cauda equina. The spinal cord presents two enlargements at the cervical and lumbar level.
In cross section, the gray matter is deep within the spinal cord and is separated into horns. The sensory axons coming from the posterior root ganglia enter the spinal cord through the posterior nerve root and synapse in the posterior horn, where interneurons are found. Autonomic motor neurons are found in the lateral horns, while somatic motor neurons are found in the anterior horns. Motor neurons send their axons out of the spinal cord through the anterior nerve root. The posterior and anterior root fuse to form the spinal nerve, which contains mixed sensory and motor information. The white matter is separated into columns which contain axons of sensory and motor neurons. The posterior columns contain ascending sensory tracts which are bundles of axons going towards the brain. The lateral and anterior column contain ascending sensory tracts as well as descending motor tracts, which carry the motor responses from the brain. Overall, the posterior regions of the spinal cord are responsible for ascending sensory information, while the anterior regions are responsible for descending motor information.
Spinal nerves are all mixed nerves with both sensory and motor fibers. Spinal nerves emerge from the spinal cord and reorganize through plexuses, which then give rise to systemic nerves. Thoracic spinal nerves are not part of any plexus, but give rise to the intercostal nerves directly.
Review Questions
Q. What region of the spinal cord contains motor neurons that direct the movement of skeletal muscles?
A. anterior horn
B. posterior horn
C. lateral horn
D. alar plate
- Answer
-
A
Glossary
- anterior column
- white matter between the anterior horns of the spinal cord composed of many different groups of axons of both ascending and descending tracts
- anterior division
- anterior branches of the brachial plexus originating from the trunks
- anterior horn
- gray matter of the spinal cord containing multipolar motor neurons, sometimes referred to as the ventral horn
- anterior median fissure
- deep midline feature of the anterior spinal cord, marking the separation between the right and left sides of the cord
- arachnoid mater
- middle layer of the meninges named for the spider-web–like trabeculae that extend between it and the pia mater
- arterial vasocorona
- blood supply to the spinal cord formed by pial anastomoses between the anterior and posterior spinal arteries on the surface of the spinal cord
- ascending tract
- central nervous system fibers carrying sensory information from the spinal cord or periphery to the brain
- axillary nerve
- systemic nerve of the arm that arises from the brachial plexus
- brachial plexus
- nerve plexus associated with the lower cervical spinal nerves and first thoracic spinal nerve
- cauda equina
- bundle of spinal nerve roots that descend from the lower spinal cord below the first lumbar vertebra and lie within the vertebral cavity; has the appearance of a horse's tail
- central canal
- hollow space within the spinal cord that is the remnant of the center of the neural tube
- cervical enlargement
- region of the ventral (anterior) horn of the spinal cord that has a larger population of motor neurons for the greater number of and finer control of muscles of the upper limb
- cervical plexus
- nerve plexus associated with the upper cervical spinal nerves
- cervical region
- region of the spinal cord where cervical spinal nerves originate from
- conus medullaris
- tapered end of the spinal cord at the lumbar vertebral level, corresponding to the sacral region of the spinal cord
- cord
- branch of the brachial plexus originating from the divisions
- dermatome
- topographical area of skin in which sensory nerves end
- descending tract
- central nervous system fibers carrying motor commands from the brain to the spinal cord or periphery
- dorsal (posterior) nerve root
- axons entering the posterior horn of the spinal cord
- dorsal ramus
- dorsal branch of a spinal nerve that forms from the dorsal root of the nerve after it emerges from the spinal cord
- dorsal root ganglion
- cluster of cell bodies in the dorsal root of a spinal nerve containing sensory neurons
- dura mater
- tough, fibrous, outer layer of the meninges that is attached to the inner surface of the cranium and vertebral column and surrounds the entire CNS
- epidural space
- area between the dura mater and the above structures
- femoral nerve
- systemic nerve of the anterior leg that arises from the lumbar plexus
- fibular nerve
- systemic nerve of the posterior leg that begins as part of the sciatic nerve
- filum terminale
- thin strand of pia mater that helps anchoring the conus medullaris to the coccyx
- gray commissure
- horizontal line of gray matter that connects the left and right sides of the spinal cord
- intercostal nerve
- systemic nerve in the thoracic cavity that is found between two ribs
- lateral column
- white matter of the spinal cord between the posterior horn on one side and the axons from the anterior horn on the same side; composed of many different groups of axons, of both ascending and descending tracts, carrying motor commands to and from the brain
- lateral horn
- region of the spinal cord gray matter in the thoracic, upper lumbar, and sacral regions that is the central component of the autonomic nervous system
- lumbar enlargement
- region of the ventral (anterior) horn of the spinal cord that has a larger population of motor neurons for the greater number of muscles of the lower limb
- lumbar plexus
- nerve plexus associated with the lumbar spinal nerves
- lumbar puncture
- procedure of taking fluid from the spine in the lumbar vertebral region through a hollow needle
- lumbar region
- region of the spinal cord where lumbar spinal nerves originate from
- median nerve
- systemic nerve of the arm, located between the ulnar and radial nerves
- musculocutaneous nerve
- systemic nerve of the arm, located lateral to the other nerves of the brachial plexus
- nerve plexus
- network of nerves without neuronal cell bodies included
- phrenic nerve
- systemic nerve from the cervical plexus that innervates the diaphragm
- pia mater
- thin, innermost membrane of the meninges that directly covers the surface of the CNS
- posterior columns
- white matter of the spinal cord that lies between the posterior horns of the gray matter, sometimes referred to as the dorsal column; composed of axons of ascending tracts that carry sensory information up to the brain
- posterior division
- posterior branches of the brachial plexus originating from the trunks
- posterior horn
- gray matter region of the spinal cord in which sensory input arrives, sometimes referred to as the dorsal horn
- posterior median sulcus
- midline feature of the posterior spinal cord, marking the separation between right and left sides of the cord
- posterolateral sulcus
- feature of the posterior spinal cord marking the entry of posterior nerve roots and the separation between the posterior and lateral columns of the white matter
- radial nerve
- systemic nerve of the arm, the distal component of which is located near the radial bone
- radicular arteries
- blood supply to the spinal cord that runs along the posterior and anterior roots of the spinal nerves
- ramus
- branch of a spinal nerve
- rami communicantes
- structures that provide a short connection from an autonomic ganglion to the spinal nerve
- sacral plexus
- nerve plexus associated with the lower lumbar and sacral spinal nerves
- sacral region
- region of the spinal cord where sacral spinal nerves originate from
- saphenous nerve
- systemic nerve of the lower anterior leg that is a branch from the femoral nerve
- sciatic nerve
- systemic nerve from the sacral plexus that is a combination of the tibial and fibular nerves and extends across the hip joint and gluteal region into the upper posterior leg
- sciatica
- painful condition resulting from inflammation or compression of the sciatic nerve or any of the spinal nerves that contribute to it
- spinal arteries
- blood supply to the anterior and posterior regions of the spinal cord
- spinal nerve
- one of 31 nerves connected to the spinal cord
- systemic nerve
- nerve in the periphery distal to a nerve plexus or spinal nerve
- terminal branch
- branch of the brachial plexus originating from the cords
- thoracic region
- region of the spinal cord where intercostal nerves originate from
- tibial nerve
- systemic nerve of the posterior leg that begins as part of the sciatic nerve
- trunk
- branch of the brachial plexus originating from the spinal roots
- ulnar nerve
- systemic nerve of the arm located close to the ulna, a bone of the forearm
- ventral (anterior) nerve root
- axons emerging from the anterior or lateral horns of the spinal cord
- ventral ramus
- ventral branch of a spinal nerve that forms from the ventral root of the nerve after it emerges from the spinal cord
- white commissure
- bundle of myelinated axons that crosses the central region of the spinal cord
Contributors and Attributions
OpenStax Anatomy & Physiology (CC BY 4.0). Access for free at https://openstax.org/books/anatomy-and-physiology


