1.14: Neuropharmacology II - Anxiolytics and Antidepressants
- Page ID
- 10636
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)Depression is a frequent problem, affecting up to 5% of the population. Common presentations include low mood, loss of energy, disinterest in activities. May also include weight loss, sleep disturbance, or psychosis. Should be considered in patients with atypical dementia and chronic pain
Diagnosis of Depression - DSM-IV
- Five of the following present during the same 2-week period and represent a change from previous functioning:
- depressed mood
- markedly diminished interest or pleasure in all, or almost all, activities
- significant weight loss when not dieting or weight gain
- insomnia or hypersomnia
- psychomotor agitation or retardation
- fatigue or loss of energy
- feelings of worthlessness or excessive or inappropriate guilt
- diminished ability to think or concentrate, or indecisiveness
- recurrent thoughts of death, recurrent suicidal ideation or a suicide attempt
- The symptoms cause clinically significant distress or impairment in social, occupational, or other important areas of functioning.
- The symptoms are not due to the direct physiological effects of a substance (e.g., a drug of abuse, a medication) or a general medical condition (e.g., hypothyroidism).
- The symptoms are not better accounted for by Bereavement
Pathophysiology of depression
- At present, mechanism is unknown - may be more than one mechanism.
- No useful biomarkers or imaging abnormality during life
- Study of postmortem brain has not revealed any consistent structural or neurochemical abnormality
- Majority of the currently available medications were discovered empirically
- Most current theories are based on “amine hypothesis”
Biogenic amines


Classes of Antidepressants
- Tricyclics and heterocyclics
- Selective serotonin reuptake inhibitors (SSRI’s)
- Bupropion
- Nonselective MAO inhibitors
- Non-pharmacological therapy
- ECT
- Psychotherapy
Tricyclics and heterocyclics - Clinical pharmacology
- Large family of structurally related compounds
- Multiple pharmacological actions
- Therapeutic effect probably due to ability to block reuptake of serotonin and/or norepinephrine
- All may be sedating, although some much more than others
- Many of these drugs have anticholinergic (anti-muscarinic) actions - leads to somnolence, dry mouth, urinary retention
Tricylics and heterocyclics - pharmacokinetics and toxicity
- All are primarily metabolized by the liver, and undergo first pass metabolism
- Biochemical half-lives range from 4 to more than 24 hours, but clinical response is much slower - typically several weeks of therapy is required to observe any clinical improvement
- Overdose of tricylics (more than 1 gram) is often lethal due to cardiac conduction disturbances. Great care must be taken when these drugs are prescribed for potentially suicidal patients.
Some commonly used tricylics and heterocyclics
- Amitriptiline (Elavil®)
- Inhibits serotonin & NE reuptake
- Prominent anticholinergic effects
- Metabolite is nortriptyline
- Desipramine (Norpramine®)
- Inhibits NE reuptake
- Mild anticholinergic effects
- Trazodone (Desyrel®)
- Heterocyclic
- Inhibits serotonin reuptake
- Minimal anticholinergic effects
- Sedating
Selective Serotonin Reuptake Inhibitors (SSRI’s)
- Act by inhibition of presynaptic reuptake of serotonin in central synapses.
- Not as sedating as many of the tricylic compounds
- Also do not have the anticholinergic side effects of the tricyclics
- Some are potent inhibitors of P450 enzyme systems, and may lead to drug interactions
Some commonly used SSRI’s
- Fluoxetine (Prozac®)
- Sertaline (Zoloft®)
- Citalopam (Celexa®)
- Paroxetine (Paxil®)
- All are potent inhibitors of serotonin reuptake
- Adverse effects: anxiety, tremor
- Overdose of SSRI alone is rarely lethal
- Should not be administered with nonselective MAO inhibitors
- Suicide as an adverse effect?
Bupropion
- Structurally related to the tricyclics, but seems to have a different therapeutic mechanism, related to altered release of NE
- Not sedating or anticholinergic, but does sometime induce hallucinations or seizures
- Also effective in treating tobacco addiction
MAO Inhibitors
- Non-selective, irreversible enzyme inhibitors - long duration of action
- Therapeutic effect is due to is enhancement of CNS amine levels
- Major adverse effects are due to excessive accumulation of amines in the circulation
- Tyramine: the “cheese effect.”
- Drug interactions: SSRI’s, sympathomimetics
- Safe in carefully controlled circumstances, but “real world” use may lead to serious adverse effects.
Treatment of depression
- Many patients will not report symptoms of depression unless asked specifically
- Patients who are depressed may be suicidal - it is essential to inquiry about their intentions
- The response of an individual patient to a particular antidepressant cannot be predicted, and treatment often requires sequential trials of several drugs
- In severely depressed patients, ECT often produces a rapid improvement and may be the best initial treatment
Sedatives and hypnotics
- Used to reduce anxiety, or induce sleep
- Very commonly prescribed
- Two principal chemical classes:
- Benzodiazepines
- Barbiturates
- Both work by enhancing activity of the inhibitory neurotransmitter, GABA
GABA (γ-aminobutyric acid)

- Principal inhibitory transmitter of the mammalian brain
- Receptors:
- GABAA: ligand gated ion channels, regulate chloride ion, at least 15 different subunit proteins
- GABAB : G-protein coupled receptors
Effects of benzodiazepines and barbiturates on GABA Receptors

- Both drugs bind to GABAA receptor subunits, but at different sites.
- Neither one binds to the agonist site
- Benzodiazepines increase the frequency of channel opening, but do not alter conductance or duration of opening
- Barbiturates prolong the duration of channel opening
Benzodiazepines
- More than a dozen benzodiazepines are marketed in the US
- They are distinguished primarily by their profiles of distribution and half-life.

- Toxicity is mainly excessive sedation.
- After chronic use, withdrawal seizures may occur, especially with short half-life agents
- Flumazenil: a benzodiazepine antagonist, blocks effects of other benzodiazepines
Barbiturates
- Also distinguished largely by half-life and duration of action.
- Toxicity is excessive sedation, but unlike benzodiazepines, often leads to respiratory depression which may be fatal.
- Biochemical half lives range from 3 hours (methohexital) to 100 hours (phenobarbital)
- Redistribution is a key mechanism regulating duration of the biological effect of barbiturates (and benzodiazepines) when administered rapidly.
Redistribution
- Redistribution is a mechanism which limits the duration of action
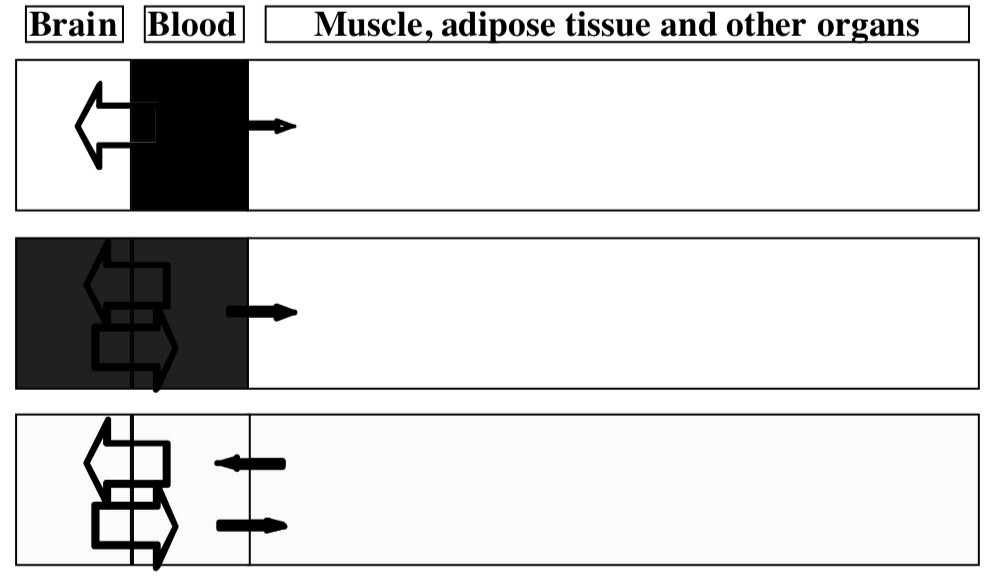
- Effect is greatest when:
- Agent is administered rapidly (e.g., intravenous)
- Agent is highly lipophilic
- Can lead to very short duration of action (minutes) even though biochemical half life is longer (hours).
Clinical use of sedatives
- Anxiolytic use
- Usually a medium to long acting benzodiazepine, such as diazepam, administered orally.
- Hypnotic use
- Usually a short to medium acting benzodiazepine, such as temazepam, administered orally - but note that all hypnotics lose efficacy if taken daily.
- Sedative use (for surgical procedures)
- A short acting benzodiazepine, such as midazolam
- A short acting barbiturate, such as thiopental
- Administered intravenously, and action terminated by redistribution.
Tolerance, cross-tolerance, and addiction
- Chronic use of sedatives of either class (benzodiazepine or barbiturate) induces tolerance to all members of the class, and cross-tolerance to members of the other class.
- Both also induce tolerance to ethanol, which acts in part through GABA receptors.
- Both benzodiazepines and barbiturates may produce dependence and are susceptible to abuse. Potentially lethal actions of the barbiturates makes them particularly problematic when abused.
- Rapid withdrawal from either class of sedatives may lead to anxiety, agitation, and seizures


