5.18: Thoracodorsal Artery Scapular Tip Flap for Head and Neck Reconstruction
- Page ID
- 53290
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
THORACODORSAL ARTERY SCAPULAR TIP (TDAST) FLAP FOR HEAD AND NECK RECONSTRUCTION
Douglas Chepeha
The thoracodorsal artery scapular tip flap is the osseous (bone) component of the latissimus dorsi flap. The thoracodorsal artery supplies the scapular tip and the latissimus dorsi muscle (with overlying skin). Therefore, the scapular tip can be harvested as an independent osseous paddle or with the latissimus dorsi muscle or with the latissimus dorsi muscle and overlying skin or in some combination with the serratus muscle. There are many possible combinations of skin, muscle and bone paddles that make this arterial donor system valuable for head and neck reconstruction. In addition, the thoracodorsal arterial system can be combined with the circumflex scapular arterial system (both arteries arise from the subscapular system or are directly adjacent to one another) to further increase the skin and bone paddle options. Although it would not always be ideal, this donor site could be used to reconstruct all defects in the head and neck.
The scapular tip and lateral border have a unique shape. The tip of the scapula is the shape of the maxillary infrastructure when inset in an axial plane. It also mimics the rim of the orbit, depending on the extent of the defect, and can be inset in axial or coronal planes. The lateral border of the tip of the scapula is the shape of a hemimandible and is well suited for mandibular reconstruction. For posterior mandibular reconstruction the tip can be used for the angle and inset in a sagittal plane to reconstruct the ramus. For anterior defects it can be inset axially in a manner similar to maxillary reconstruction or it can be osteotomized and inset in a coronal orientation.
In this chapter we address the use of the bone paddle supplied by the thoracodorsal artery.
Benefits of TDAST
- Long vascular pedicle 1,2
- Triangular 3-dimensional shape 2
- Bone paddle easily shaped without osteotomy to reconstruct the infrastructure of the maxilla 3
- Bone is surrounded by attached muscle that can be used to help close defects of maxillary and mandibular alveolus bone
- Can be harvested as a chimeric flap with a variety of skin and muscle paddle options 3-5
- Independently mobile skin paddle 2,3
- Thoracodorsal artery and vein are large vessels and most commonly connect to larger subscapular vessels
Caveats of TDAST
- Overall harvest is manageable but one must exercise caution with the identification of the angular branch and its connection to either the thoracodorsal artery or the serratus artery
- Shorter bone length (12 cm) than fibula 6-8
- If the angular branch does not appear to supply the superior aspect of the lateral border of the scapula, then the circumflex scapular artery may have to be harvested to ensure vascularity
- Wide skin donor sites can be hard to close and can limit shoulder mobility
- The skin donor sites may be thicker than the forearm, anterolateral thigh and the lateral arm flaps depending on body habitus and gender
- Reduced shoulder mobility 9,10
- Prior ipsilateral thoracotomy may limit skin paddle donor options
- Two-team surgery if a hydraulic arm holding device is not used 11
Anatomy
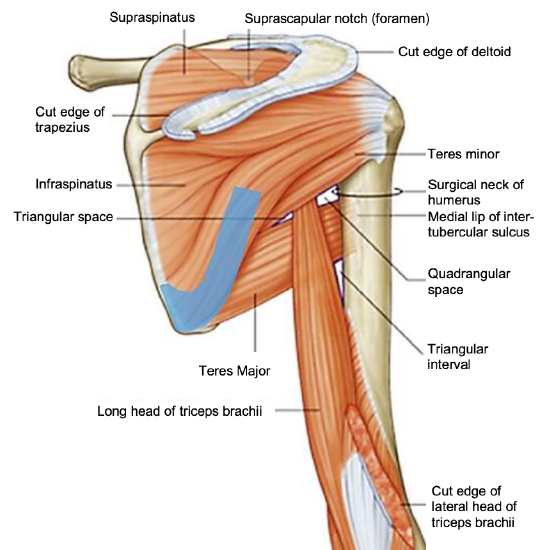
Figure 1: Posterior view of shoulder and arm
Harvesting the scapular tip involves transecting a portion of, or all the origins of the infraspinatus, subscapularis, teres major, the insertion of the serratus and, if a skin paddle is harvested, dissection and possible harvesting of the latissimus dorsi flap. Several of these muscles are part of the four muscles that form the rotator cuff that stabilizes the glenohumeral joint (Figure 1).
Rotator Cuff and Muscle Anatomy
Four muscles originate from the scapula and stabilize the glenohumeral joint (Figure 1):
- Supraspinatus and infraspinatus muscles originate in fossae above and below the scapular spine and attach to the greater tubercle of the humerus. The supraspinatus initiates the first 15º abduction of the arm, whereas the infraspinatus allows lateral rotation of the arm on the glenohumeral joint
- Teres minor arises from the lateral edge of the scapula and attaches to the greater humeral tubercle. It also allows lateral rotation of the arm
- Subscapularis arises from the subscapular fossa (the part of the scapula that faces anteriorly toward the thorax) and inserts into the lesser tubercle of the humerus. It rotates the humerus medially on the glenohumeral joint.
- Teres major is encountered surgically but is not a rotator cuff muscle. It arises from the inferior angle of the scapula and attaches to the anterior surface of the humerus, on the medial lip of the intertubercular sulcus. It allows medial rotation and adduction of the humerus on the glenohumeral joint. The long head of the triceps brachii is also encountered in this region as it originates in the infraglenoid tubercle of the scapula. It serves as an accessory adductor, an extensor of the forearm and a stabilizer of the glenohumeral joint
Vascular Anatomy
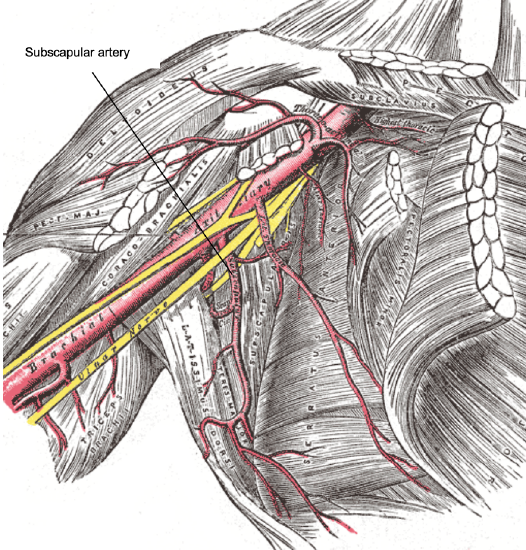
Figure 2: Origin of subscapular artery from axillary artery
The subscapular artery arises from the third part of the axillary artery (Figure 2).
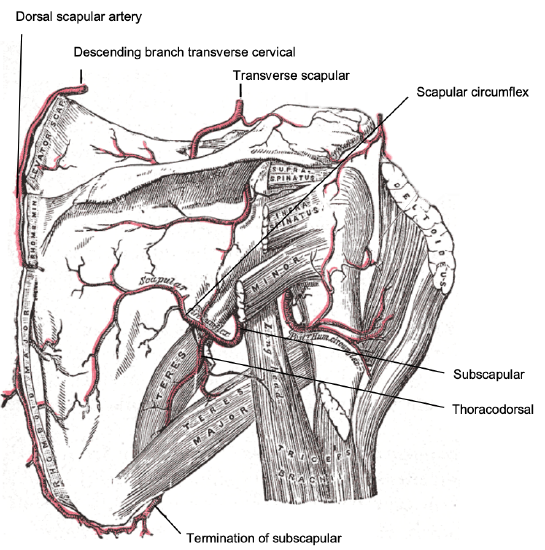
Figure 3: Vascular anatomy around the scapula
It gives rise to two branches: the thoracodorsal artery, and circumflex scapular artery (Figure 3). The thoracodorsal artery and/or thoracodorsal vein can arise from the axillary vein, separate from the subscapular artery and/or the subscapular vein 12
The thoracodorsal artery arises from the subscapular artery, descending, roughly parallel to the lateral boarder of the scapula in an envelope of adipose tissue that emanates from the axilla (Figure 3). The thoracodorsal artery passes between the teres major and the thoracic cage (Figure 2) 12. The thoracodorsal artery supplies the latissimus dorsi, serratus anterior, and scapular tip 13.
The thoracodorsal artery gives rise to a direct cutaneous branch, the serratus artery, the angular artery to the scapular tip, the descending branch within the latissimus muscle and the transverse branch within the latissimus muscle. The direct cutaneous branch is present 47% of the time (reference Taylor 1984) and supplies the skin inferior to the axilla. The serratus branch supplies the serratus muscle that can be used for myogenous reconstruction or as an innervated subunit.
The angular branch to the scapular tip arises from the thoracodorsal branch 6 within 1.5 cm of the serratus artery branch or from the serratus branch within 1.5 cm of its branchpoint with the thoracodorsal artery. The origin of the vein and artery of the angular artery pedicle can be divided between the thoracodorsal branch and the serratus branch. The total length of the dissected pedicle and bone paddle (distance from the axilla to the scapular tip) can be as long as 27 cm 1,2,14. This is likely to be an overestimate; the total length is closer to 20 cm.
The descending and transverse thoracodorsal branches are within the latissimus muscle and can be used to supply some or all of a myogenous paddle, a myocutaneous paddle, or a cutaneous perforator (if present), and can be dissected through the muscle.
The circumflex scapular artery (Figure 3) travels through the triangular space 3 created by the teres major inferiorly, teres minor superiorly, and long head of triceps anteriorly (Figure 1). It divides into a terminal descending branch to the bone of the lateral border of the scapula; the circumflex scapular artery continues toward the skin and divides into transverse cutaneous and descending cutaneous branches. The terminal descending branch supplies the lateral border of the scapula and the maximal bone length is 12 cm. The transverse cutaneous branch can be used to create a scapular cutaneous paddle 3. The descending cutaneous branch is used to create parascapular cutaneous paddle 3.
Nerve Anatomy
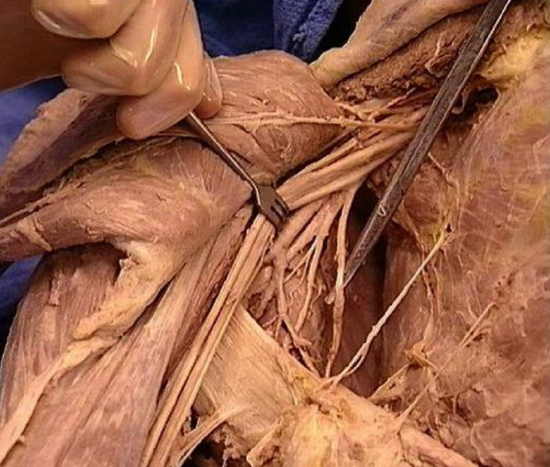
Figure 4: Anterior view of right thoracodorsal nerve
The thoracodorsal nerve (Figures 4, 11) runs along the pedicle to the latissimus muscle. The nerve is about 2 mm in diameter. When harvesting the scapular tip, it should not be sacrificed and is a good guide for the direction of the pedicle and can help open the space over the pedicle. In the axilla, the cords of the brachial plexus run immediately superior to the axillary artery and vein. Care should be taken not to put traction on these nerves.
Preoperative Evaluation
No specific vascular testing is required. If a patient has a history of shoulder dislocation, rotator cuff tear, rotator cuff surgery, arthroscopy, joint replacement or brachial plexus injury one should avoid using the flap. Consideration must be given to the patient’s occupation and recreational activities, as lifting heavy weights above the head is affected 2.
Informed Consent
Preoperative counseling should address general complications related to autogenous transplant including scarring, delayed wound healing, donor or recipient site hematomas, seromas, infection and transplant failure.
Specific complications include reduced shoulder mobility that makes full abduction and lifting heavy object above the head more difficult 15. Larger bone paddles are associated with greater shoulder disability.
Surgical Setup
The surgical setup is very similar to the setup described in the chapter on latissimus dorsi flaps.
Patient Positioning
A key advance is to avoid repositioning by putting the patient in a semidecubitus 2 and using a beanbag to secure the patient’s donor site about 20 degrees above the plane of the bed. Ensure that the entire scapula is accessible. Access to the scapula can be improved by abduction or medial rotation with the shoulder in an adducted position. Unfortunately, this setup still does not make 2-team surgery straightforward.
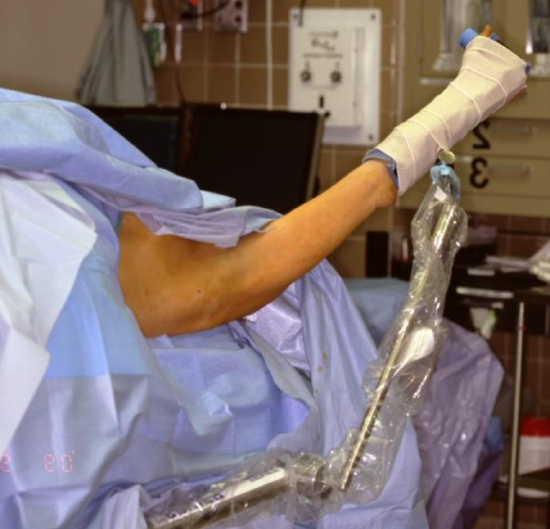
Figure 5: The patient’s left arm and thorax are shown with the arm in a position of elevation for the thoracodorsal artery transplant (TDAST)
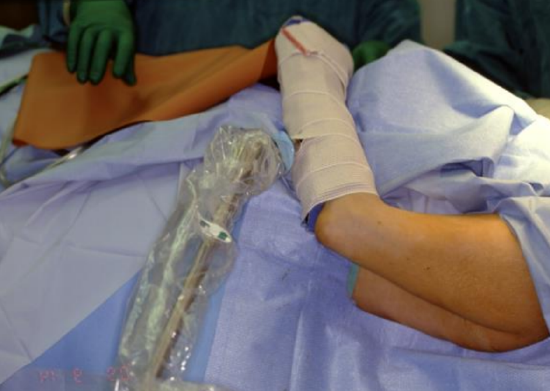
Figure 6: The patient’s left arm and thorax are shown, with the arm in a resting position. To reduce the likelihood of a tourniquet effect on the arm, avoid wrapping the arm tightly, minimize the time the arm is wrapped and be mindful of a positive fluid balance during the procedure
A positioning device can be used to hold the arm in position 11 (Figure 5). These devices are in common use for rotator cuff repair and are available at many hospitals with orthopedic programs. Take care to put the arm in the device for the duration of the elevation and closure to avoid a tourniquet effect on the forearm (Figure 6).
- Rotate the ipsilateral pelvis and bend the knee; this will help keep the thorax off the surgical table
- To prevent compression of the brachial plexus the contralateral clavicle (nonoperative shoulder) needs to be at 90 degrees to the cervical spine. A shoulder roll will not help prevent brachial plexus compression. The purpose of a shoulder roll is to lift the thorax off the operative table when the patient is in a fully decubitus position so that the clavicle does not compress the brachial plexus
- Protect the contralateral (non-operative side) superficial peroneal nerve, radial nerve, ulnar nerve and brachial plexus
- Secure the patient to the operating table with a belt and tape over the pelvis to prevent him/her sliding off the table
- Place the patient on a gel mat over a beanbag. Be sure that there is an edge (or lip) on the beanbag ipsilaterally and contralaterally to hold the patient in position
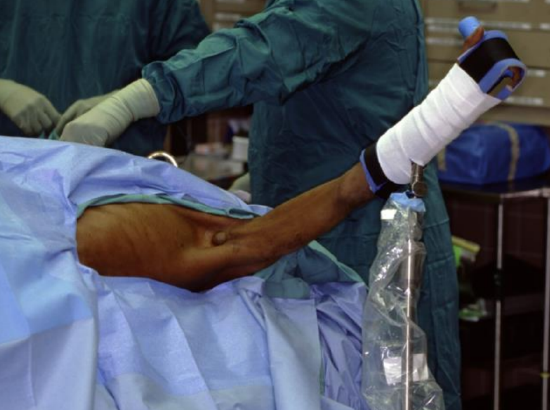
Figure 7: For patients who have a rounded thoracic cage, a scapula that has a lateral position and a flexible neck may undergo harvest on the side contralateral to the head and neck extirpation site (note lipoma in axilla)
- Some patients can undergo a contralateral scapular tip harvest if they have a very rounded thorax in cross-section, their scapula is in a very lateral position and they have mobile necks (Figure 7). In such cases, 2-team surgery is easier to accomplish
Surgical Steps
Surface Markings
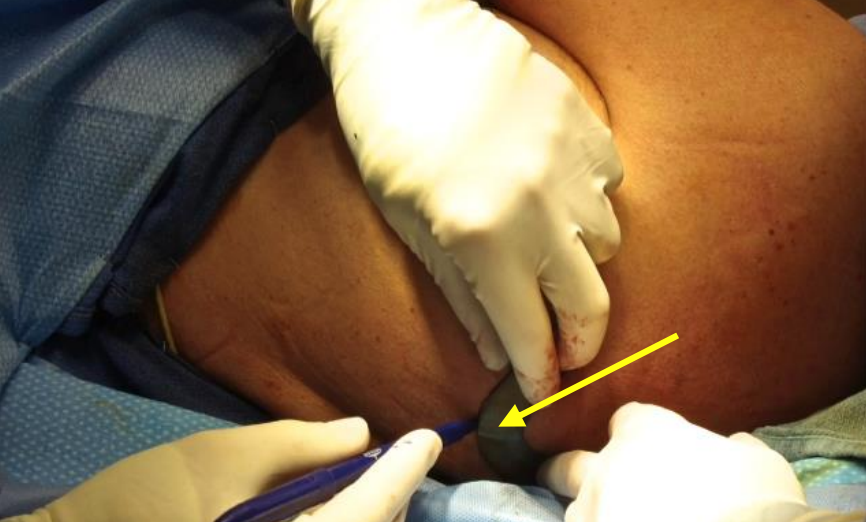
Figure 8: Patient is turned to left side with left arm superiorly and harvesting on the left thorax. Locate and mark the scapular tip by palpation. The arm is in a neutral position at the upper right of the photo. Arrow points to bone paddle
- To safely locate the bone paddle the latissimus muscle and scapular tip have be palpated and marked out prior to incision. This is usually straightforward (Figure 8)
- The anterior edge of the latissimus muscle is marked by the midaxillary line. It is best to mark the midaxillary line prior to prepping because the pelvis is usually covered by the belt that secures the patient to the operating table
- Locate the midaxillary line by drawing a line from the middle of the axilla to a point on the pelvis that is equidistant between the anterior and posterior superior iliac spines
- Identify the latissimus muscle. It forms the posterior axillary fold as it crosses from the thorax to insert onto the humerus. The superior aspect of the latissimus muscle curves across the tip of the scapula as it heads to the origin of the muscle from thoracic vertebrae 6-12
- Locate the scapular tip at the inferior aspect of the scapula, and mark it with the shoulder adducted (arm at patient’s side)
Raising the Bone Paddle - Anterior versus Posterior Approach
The scapular tip can be approached either from the anterior, or the posterior aspect of the latissimus muscle. The anterior approach is the most commonly used. There is no distinct advantage of an anterior versus a posterior approach.
Anterior approach
- Considered easier and more flexible
- Easier to dissect all the branches of the thoracodorsal vascular pedicle
- Efficient if a myocutaneous skin/latissimus muscle paddle is part of the reconstructive plan
- Advantagous if a series of paddles are to be harvested that includes the circumflex scapular system, as the pedicle and the associated skin paddles are easier to expose in a single surgical field
- Favored if the descending branch of the thoracodorsal artery is going to harvested with preservation of the transverse portion of the thoracodorsal nerve
Posterior approach
- More difficult but more direct
- An advantage for harvesting a thoracodorsal perforator flap
- Good choice if scapular tip is sole donor paddle
- Good choice if direct cutaneous branch of thoracodorsal artery or a perforator of thoracodorsal artery is anticipated with the harvest
Raising the Bone Paddle: Anterior Approach
- Mark out an incision 1.5 cm anterior to the midaxillary line from a level just below the tip of the scapula tip to the axilla. In the axilla, it is better to angle the incision to run parallel to the relaxed axillary skin tension folds (Figure 6)
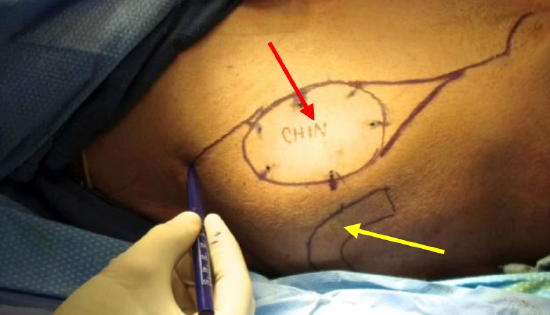
Figure 9: Patient is turned to left side axilla on right of picture and harvesting on the left thorax. The yellow arrow points to the bone paddle template. The latissimus muscle is in contact with and anterior to the scapula. The skin paddle (red arrow) is over the primary angiosome. The skin paddle overlies the latissimus muscle. The location of the skin paddle as shown in the figure is helpful for perforator dissection. If a longer pedicle to the skin paddle is desired, then the skin paddle can be elevated in a position that is just inferior to the scapular tip along the midaxillary line
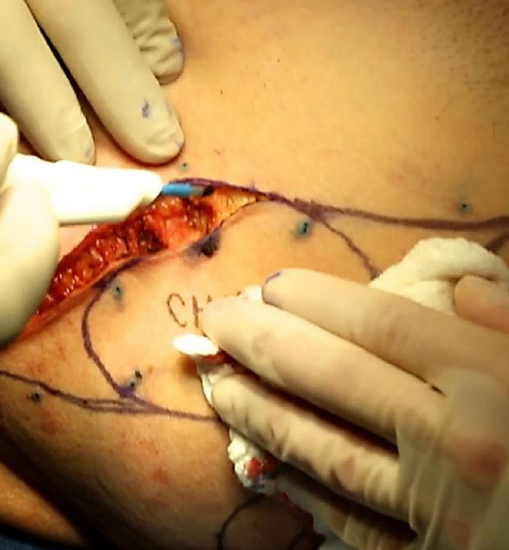
Figure 10: Dissection of the myocutaneous donor paddle; with an anterior approach, the skin paddle is dissected first
- Commence the incision inferiorly to verify the location of the anterior border of the latissimus muscle to confirm that the surface marking has been made in the correct location (Figure 10)
- Once the location of the latissimus muscle has been confirmed, extend the incision up to the axilla
- Critical point: It is important to understand that the incision crosses the expected location of the thoracodorsal pedicle. Therefore, once the anterior border of the latissimus is identified at the level of the scapular tip, dissect just superficial to the medial aspect (the side closest to the thorax) of the latissimus muscle until the thoracodorsal pedicle is seen penetrating the muscle
- Once the thoracodorsal pedicle has been identified, trace it toward the axilla. The thoracodorsal nerve is a good landmark and speeds up the dissection
- Retract the latissimus muscle to open the space around the pedicle
- The pedicle is in a pocket of areolar tissue; therefore, gentle finger dissection will improve the efficiency of the dissection
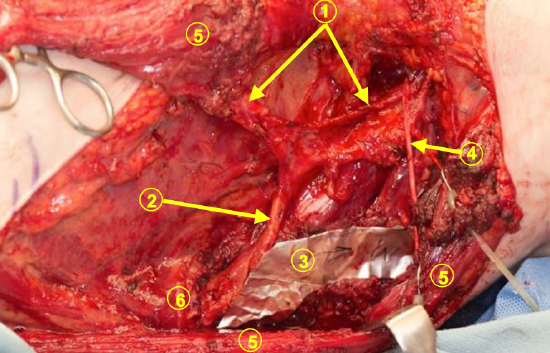
Figure 11: A different patient with more extensive bone harvest. The patient’s axilla is at the right of the picture, and the harvest is on the left thorax. The skin paddle (superiorly) has been dissected and the remaining latissimus muscle (5) is retracted at the lower edge of the photo. The thoracodorsal artery (1) can be seen supplying the latissimus muscle. The angular branch (2) can be seen supplying the scapular tip (3 = template of bone paddle, 4 = thoracodorsal nerve, 6 = serratus branch)
- It is important to skeletonize the thoracodorsal pedicle and the branch(es) to the serratus muscle before any major branches are clipped because the branching pattern of the angular branch to the scapular tip is variable (Figure 11)
- The angular branch arises within 1.5 cm of the branch point of the serratus artery. The angular branch may arise from the thoracodorsal branch (the main pedicle) or it may arise from the serratus branch. The serratus branch comes off the thoracodorsal branch before it terminates in the latissimus muscle and after the circumflex scapular branch (Figure 11)
- Key point: The angular branch arises within 1.5 cm of the serratus pedicle branch point. The angular artery and the angular vein may arise separately (but in close proximity) to the thoracodorsal branch and the serratus branch
- Locate the angular branch. First identify the anterior border of the scapular tip. This area can be seen by retracting the latissimus muscle. Generally, the artery can be seen running along the anterior border of the scapula and can be traced back to the area around the branch point of the serratus branch from the thoracodorsal pedicle
- Key point: Fully dissect the angular branch before transecting any branches greater than 1 mm. The angular branch is variable and circuitous and is vulnerable to transection before the course of the branch has been identified in its entirety
- Uncommonly, if the angular branch is not easily seen along the anterior border of the scapula:
- Dissect anteriorly, leaving a cuff of fat over the serratus about 1.5 cm anterior to the scapular tip. Dissect layer-by-layer through fascia and fat
- If the angular branch is still not seen, move superiorly staying well anterior to the scapula until the dissection is taken up to the thoracodorsal pedicle. As this space is carefully opened the branch to the scapular tip is seen coming off the serratus or the thoracodorsal pedicle
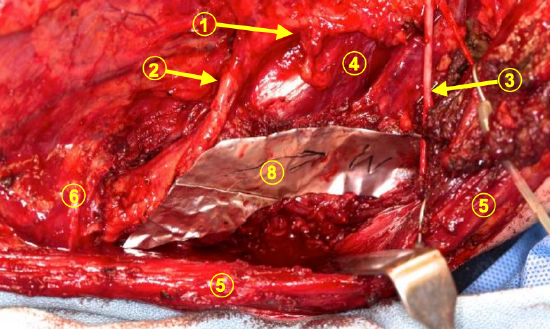
Figure 12: The teres major is transected. Both the angular branch (inferiorly) and the circumflex scapular branch (superiorly) are shown supplying the muscle (1 = thoracodorsal artery, 2 = angular artery, 3 = thoracodorsal nerve, 4 = subscapular muscle, 5 = latissimus muscle, 6 = serratus branch, 8 = bone paddle template
- After the pedicle has been identified, mobilize it by transecting the branches to the tissues that are not part of the donor system (Figure 12)
- Mark out the segment of bone that is to osteotomized into the skin paddle (Figure 12)
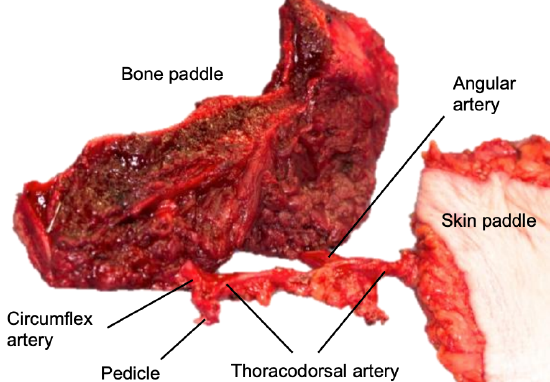
Figure 13: The bone paddle is the lateral border of the scapula with scapular tip. The skin paddle is a myocutaneous paddle based on the descending branch of the thoracodorsal artery
- If muscle is not needed for the reconstruction, it should be harvested with the bone in moderation. A cuff of about 7 mm should be left on the scapular tip to ensure adequate vascular supply (Figure 13)
- Should additional muscle be required for the reconstruction, then teres major, infraspinatus, or serratus can be harvested
- Caveat: Verify that the muscle has adequate blood supply for the planned reconstruction prior to transecting the pedicle and transferring the flap to the recipient site
Raising Bone Paddle: Posterior Approach
- Mark out the incision that is placed just posterior to the posterior edge of the latissimus muscle to a position just below the scapular tip
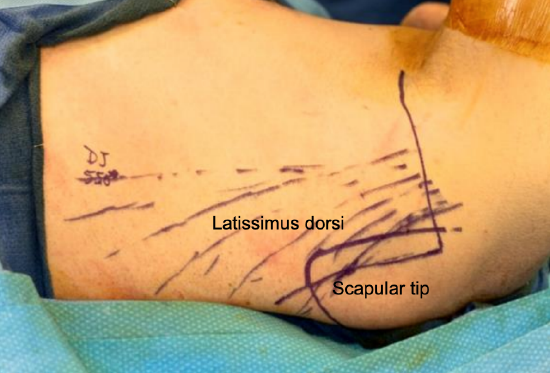
Figure 14: The scapular tip is marked out first, then the midaxillary line, followed by the expected location of the latissimus muscle
- Then mark an incision into the axilla that crosses the posterior axillary fold into the axilla and parallels the relaxed axillary skin tension lines (Figure 14)
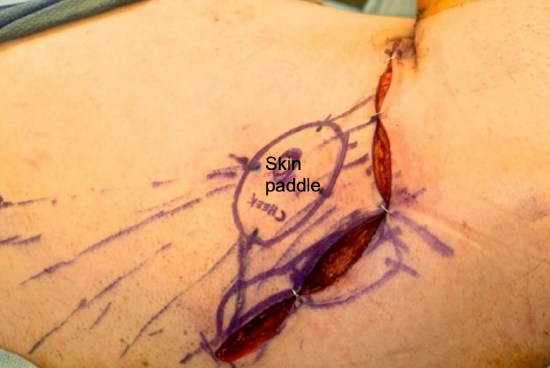
Figure 15: A perforator has been located during the deep dissection and confirmed with Doppler. The skin is loosely reapproximated so that the donor skin paddle size can be matched to the size of the recipient site
- This incision is designed so that perforators can be picked up at the anterior edge of the latissimus muscle for design of a thoracodorsal artery perforator flap (Figure 15)
- The size of the skin paddle and the option to use perforators from the transverse branch of the latissimus pedicle, will result in a different incision location. A perforator that is suitable for a perforator based cutaneous skin paddle is not always present
- Difficult step: It can be difficult to separate the teres major muscle from the latissimus muscle because the fibers may not be separated by an areolar layer. To assist with separation, increase the size of the operative field to identify the latissimus closer to its insertion and closer to its origin (Figure 13)
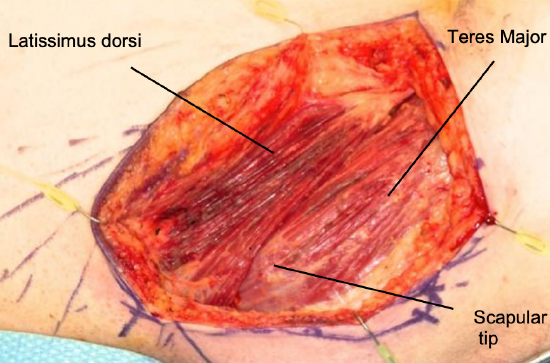
Figure 16: Separation of latissimus muscle from teres major muscle
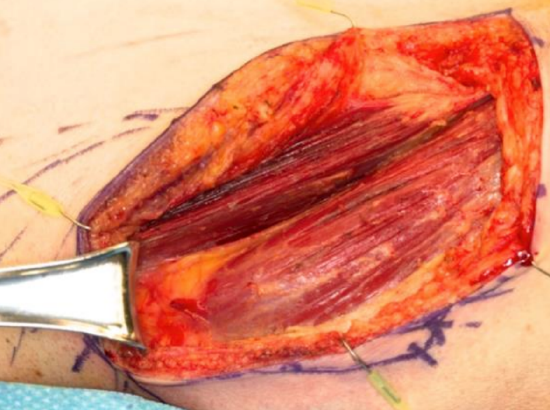
Figure 17: Retraction of latissimus muscle inferiorly to expose scapular tip
- To harvest the scapular tip bone paddle, retract the superior edge of the latissimus muscle inferiorly and anteriorly to expose the scapular tip (Figure 17)
- Sometimes a perpendicular incision needs to be made in the superior aspect of the latissimus muscle over the scapular tip so that the tip can be visualized
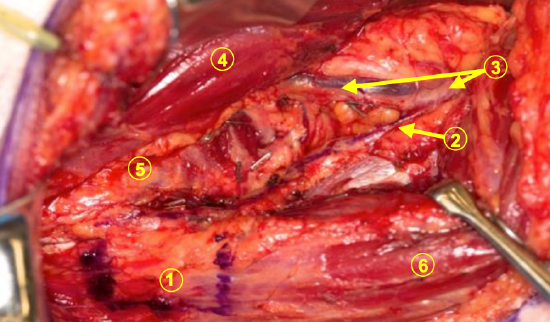
Figure 18: The planned bone paddle is marked out in blue ink just proximal to the scapular tip (1). The angular artery (2) is seen traveling from the thoracodorsal artery (3) down to a location just anterior to the bone paddle. Because this is a posterior approach, the latissimus dorsi muscle (4) is seen retracted along the upper aspect of the photo (5 = Serratus branch, 6 = Teres major muscle)
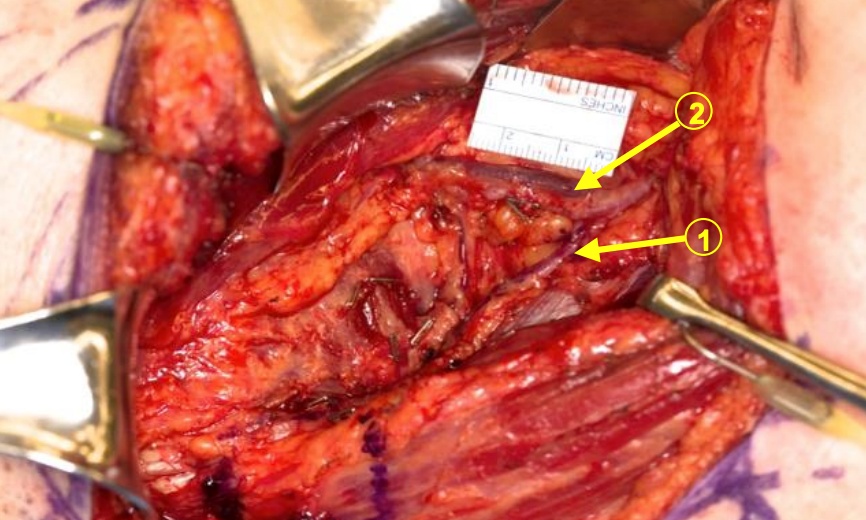
Figure 19: The ruler shows the angular branch (1) coming off the thoracodorsal artery (2) and vein 1.5 cm proximal to the serratus artery and vein
- Key point: Look for the angular branch right on the scapular tip as it passes onto the serratus muscle insertion (Figure 18).
- Follow the angular branch up to the thoracodorsal branch or the serratus branch (Figure 19)
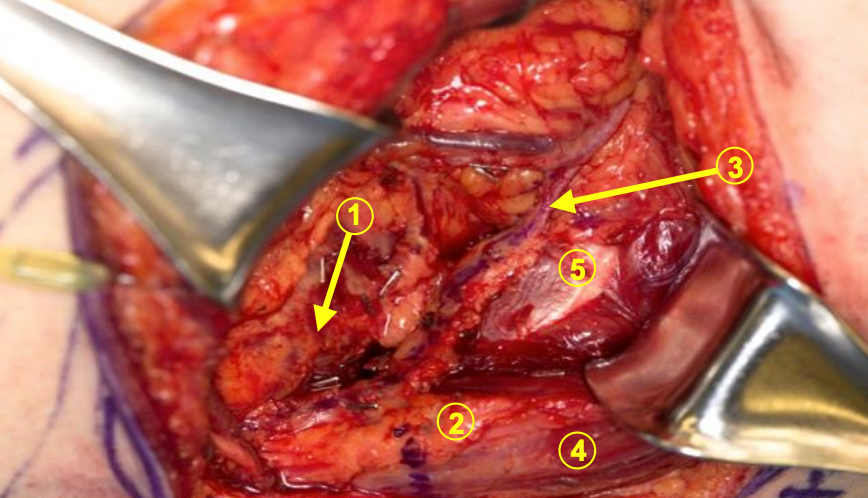
Figure 20: The serratus branch has been clipped (1), and the scapula (2) is being rotated off the thorax with a retractor. The dissected angular artery (3) to the scapular tip is well demonstrated (4 = teres major muscle, 5 = infraspinatus muscle)
- If the angular branch cannot be seen at the tip, do not dissect the fat immediately adjacent to the scapular tip because critical perforators from the angular branch can be injured as they pass to the scapular tip
- A better decision may be to transition to the anterior approach
- Alternatively, one can do a more time consuming and difficult dissection as follows: Move the dissection anteriorly leaving a cuff of fat on the anterior aspect of the scapular tip and stay on the fascia on the medial aspect of the latissimus muscle. Once the dissection is 1.5 cm anterior to the scapular tip, dissect through the fascia and fat layer-by-layer. If the angular branch is not seen, move superiorly, staying well anterior to the scapula until the dissection is taken up to under the teres major. As this space is carefully opened the branch to the scapular tip or the thoracodorsal artery is revealed (Figure 17).
- If the posterior approach does not reveal the pedicle, the dissection can still default to the anterior approach because this provides a larger surgical field and is its easier to landmark the latissimus and serratus pedicles
- Mobilize the pedicle by dissecting towards the axilla
- The thoracodorsal nerve is a helpful guide for opening the space and should be preserved
- Muscle transection and bone paddle harvest are performed in the same manner as with the anterior approach (Figures 21-23)
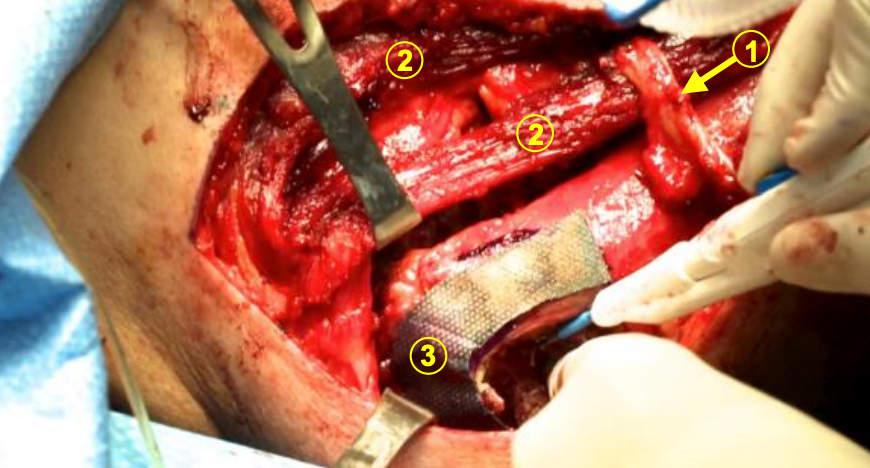
Figure 21: The patient’s axilla is at the right, and the harvest is on the left thorax. The serratus has been cut to help retract the scapular tip from the thorax to aid dissection. The infraspinatus muscle is being cut in preparation for the osteotomy. The = thoracodorsal artery (1) is shown traveling to the mobilized skin paddle that is under the surgeon’s right hand (2 = latissimus muscle, 3 = bone paddle)
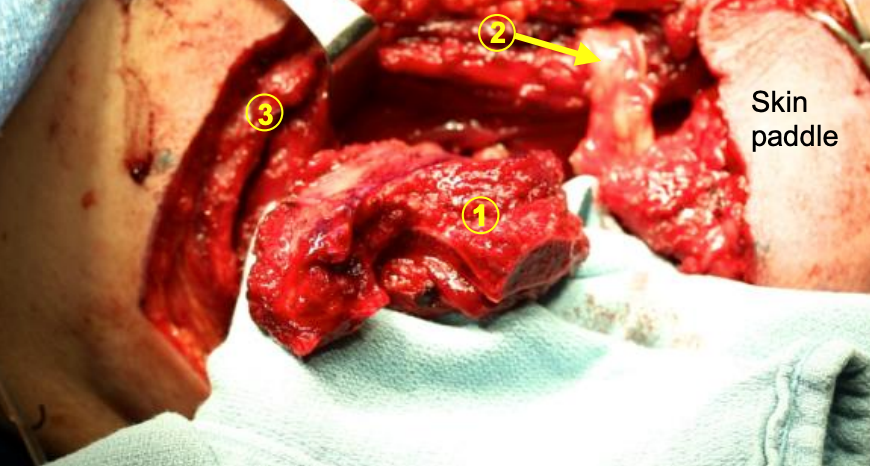
Figure 22: The osteotomized scapular tip (1) is shown in preparation for an axial inset for an anterior mandibular defect. A reciprocating saw with a long triangular blade is used for scapular tip osteotomies. Because of the curved shape of the scapula, hold the edge of the scapula with a thumb and 2nd finger to gauge the width of the bone that is being osteotomized (2 = thoracodorsal artery, 3 = latissimus muscle)
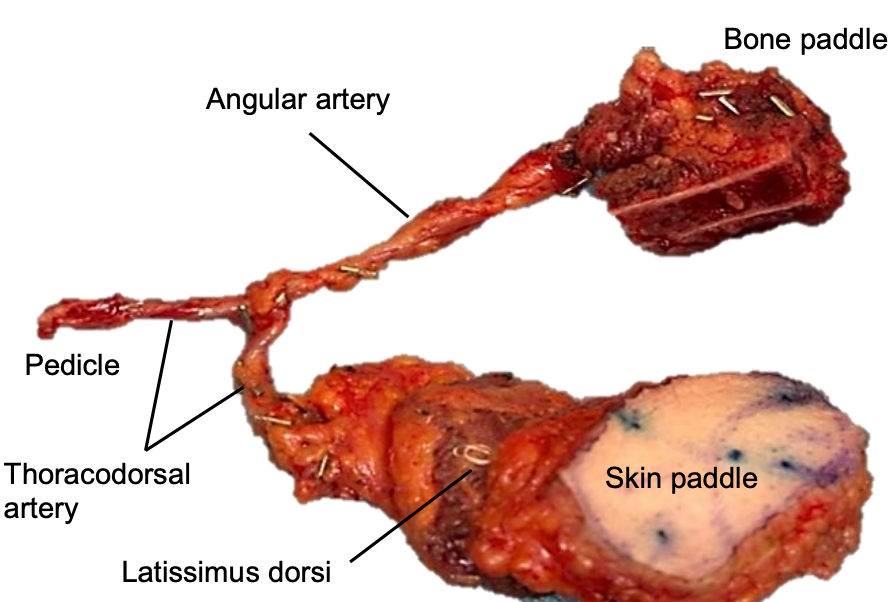
Figure 23: A chimeric segment of scapula adjacent to the scapular tip based on the angular branch and a 2nd skin paddle with a plug of muscle. This was inset into a defect that included the infraorbital rim and the cheek skin
Closure and wound drainage
Muscle closure should be performed with the shoulder in full abduction. The rotator cuff muscles should not be closed under tension and the serratus muscle should be reattached to the remaining distal end of the scapula.
The donor site is prone to seroma if the skin is loose after wound closure. Place drains in an inferior (dependent) location in the donor site. On occasion, patient may be discharged from hospital with drains in place until drainage is <20 mL per day.
Postoperative Care
- Start a passive range of movement early
- For the first 3-7 days the donor site is painful with movement
- A large skin paddle harvest with tight closure can limit mobility
- Introduce active range of motion exercises within 1-2 weeks
- There will be some associated moderate pain with this early program. It is important for the patient to know that they will not be pain free when starting the program
- The program is a combination of passive and active range of motion that would be performed after rotator cuff surgery and strengthening after neck dissection
Reconstructive Applications of Scapular Tip Bone Paddle
- The scapular tip is very versatile because of its 3-dimensional shape that is very similar to the size and shape of many head and neck bone defects 2
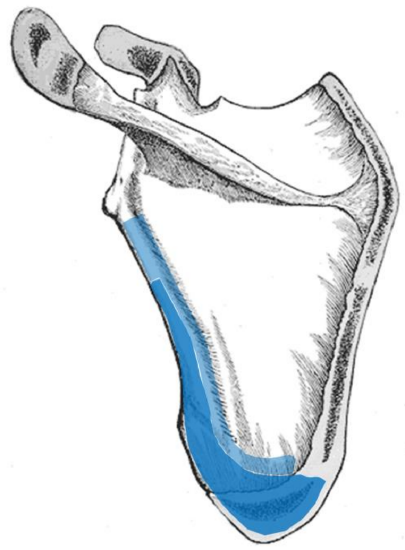
Figure 24: The maximum size of scapular harvest based on the angular branch. Darker blue indicates more reliable vascularity
- The scapular tip and lateral border of the scapula can be harvested based on the angular branch (Figure 24)
- If the angular branch inserts very distally on the scapular tip the bone of the lateral border of the scapula adjacent to the lip of the glenoid fossa in the expected location of the circumflex scapular artery may be inadequately perfused. In such cases the circumflex scapular should be harvested to supply this bone segment
- It also has a long pedicle that makes this donor site useful for vessel-poor necks or when the reconstruction is in the midor upper face 2.
- In addition, because of the multiple branches in the scapular subsystem there is a variety of skin paddle, muscle paddle, innervated muscle paddle, and bone paddle options that provide enough options that a second free flap donor site can be avoided
Maxillary Reconstruction
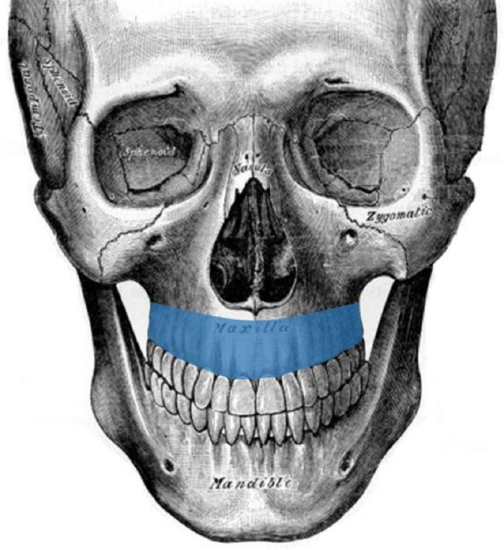
Figure 25: The most common use of a scapular tip transplant is a transverse insertion to replace part of, or the entire infrastructure of the maxilla
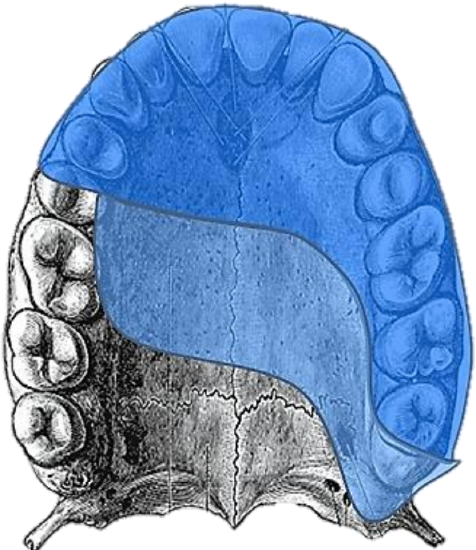
Figure 26: Total infrastructure palate
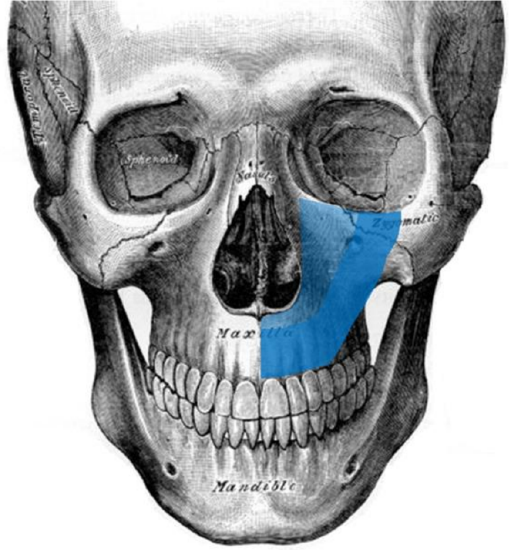
Figure 27: Hemimaxillectomy; the scapula is in a coronal orientation and is used to reconstruct alveolus and orbital rim
- Axial orientation is used for partial or total infrastructure maxillary reconstruction 1,9,10,15-17 (Figures 25, 26)
- A coronal orientation is used for hemimaxillectomy defects up to and including the infraorbital rim 5,9 (Figure 27)
Oral Cavity Reconstruction
- Sagittal orientation is used for most hemimandibulectomy reconstructions 7
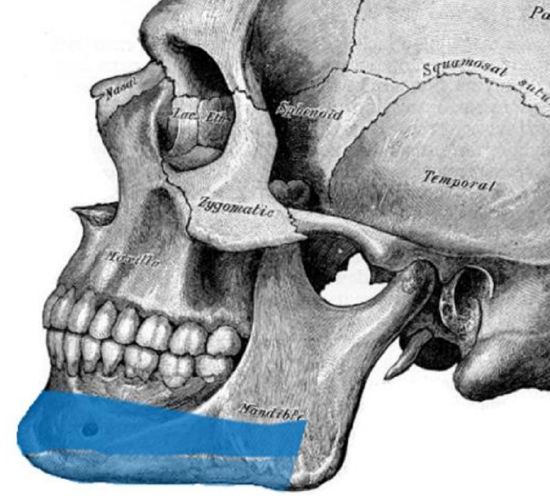
Figure 28: Hemimandible reconstruction with ipsilateral scapula. With this orientation the vascular pedicle is in a location that is less conducive to implants
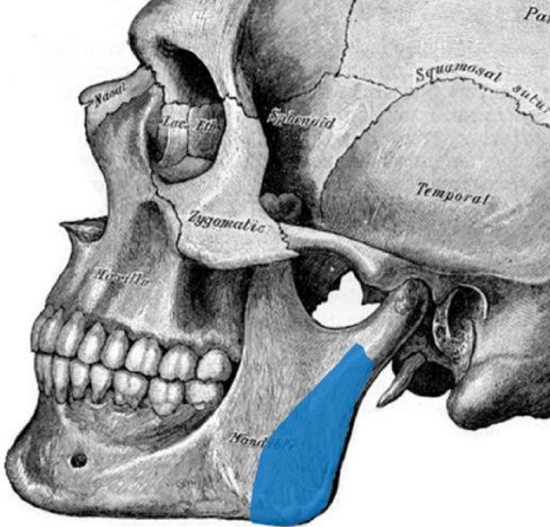
Figure 29: Angle and ramus reconstruction
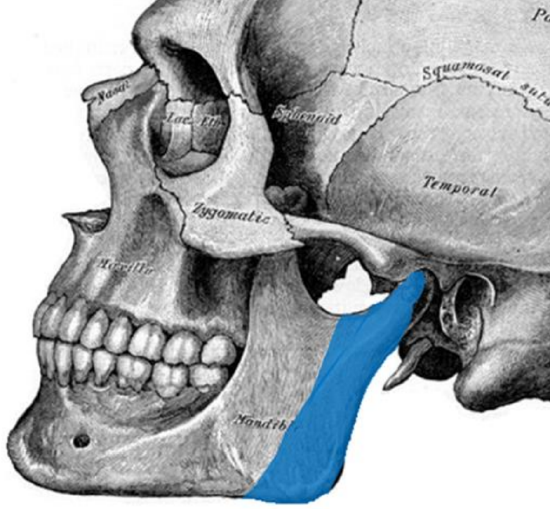
Figure 30: Condyle and ramus reconstruction
- The chest CT can be preoperatively to see if the contour matches a fit that would allow for inset without osteotomy (Figure 28)
- Sagittal orientation is used for the angle and ramus up-to-and-including the condyle of the mandible 12 (Figures 29, 30). The pedicle exits anteriorly or inferiorly. The tip of the scapula is used for reconstruction of the condyle
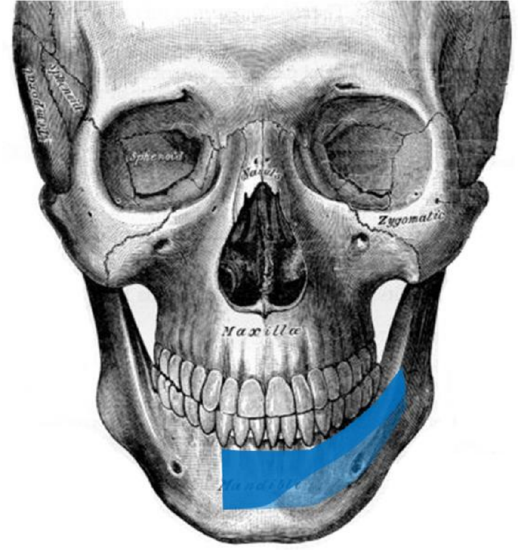
Figure 31: Partial symphysis and anterior body ipsilateral scapula reconstruction
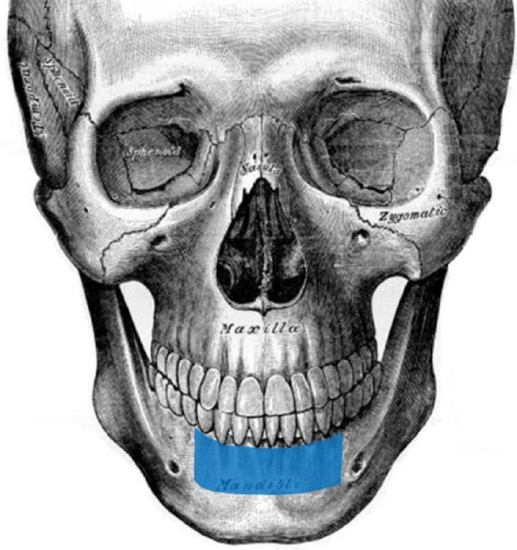
Figure 32: Bilateral symphysis and anterior body reconstruction
- Axial orientation for the reconstruction of a portion of the symphysis and anterior body of the mandible (Figure 31)
- Axial orientation for anterior symphysis defect of the mandible. The tip of the scapula does not fit the mandibular symphysis as well as with the maxilla but depending on the shape of the donor scapula, the fit can be adequate (Figure 32). This approach works well for large anterior composite resection of the oral cavity that includes the tongue because the bone requirements are less sophisticated
Orbital Reconstruction
- Use the natural curve of the scapular tip 19-21
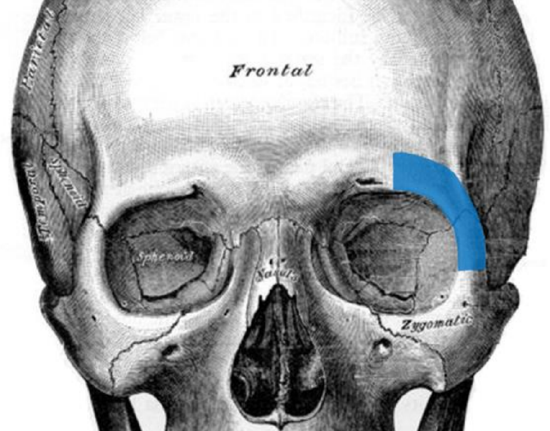
Figure 33: Lateral orbital rim reconstruction
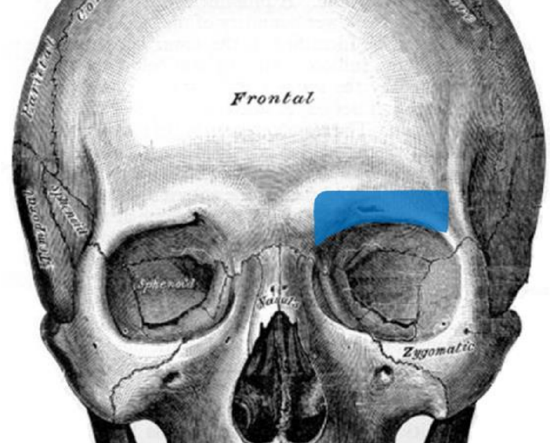
Figure 34: Supraorbital rim reconstruction
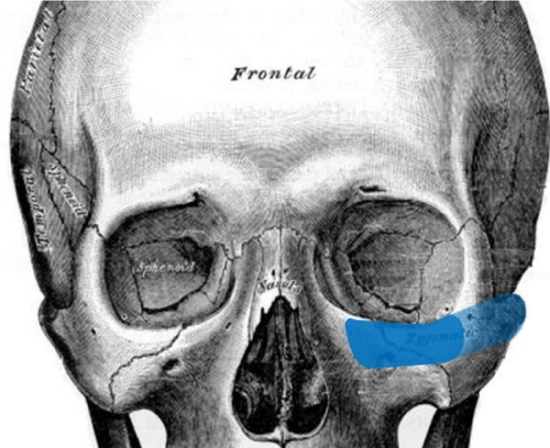
Figure 35: Infraorbital rim reconstruction
- Make a template of the missing segment of orbit and find the best match to this curve on the tip of the scapula (Figure 33)
- For reconstruction of the orbital rim use a short segment (Figure 34)
- For reconstruction of the orbital rim and orbital floor with an intact orbit. Use a small fragment of free bone or a MEDPORE orbital floor prosthesis (Figure 35)
Cricoid Reconstruction
- This is a very advanced reconstruction
- The curved scapular segment is 3 mm wide and must be covered with vascularized muscle 22
- The inset is difficult because vascularity of the scapular segment is required
Suitability for Implants
Implants can be used in the craniofacial skeleton (orbit) or the oral cavity (maxilla or mandible). Although it is possible to implant the scapula 23, there are several barriers and as a result, patients are infrequently implanted.
There are a number of barriers to implantation: the bone must be in a location that facilitates an occlusal plane; the implants should be placed prior to radiation to reduce implant failures; soft tissue reconstruction has to result in an implantable alveolar subunit; and the tongue must be able to reach around the front of the prosthetic to clear food during mastication.
It is important to note that implant-borne prostheses can cover critical sensate tissue and/or impair tongue mobility. As a result, the long-term use of implant borne prostheses is limited because many patients can eat more efficiently with a softer diet without an implant borne prosthesis. The most frequent area of success with implant use is in the maxilla because the bone placement is more straightforward, the prosthesis does not impair tongue function or cover a critical sensate area. Of course, if the bone is placed prior to radiation, it will not be suitable for implantation. Implants can be placed around the orbit to retain an orbital prosthesis but most often, instead of a prosthesis, the orbit is filled with soft tissue and this achieves patient acceptance 19.
Summary
The thoracodorsal artery scapular tip flap is the osseous (bone) component of the latissimus dorsi flap. The donor material is extremely flexible, and presents many possible combinations of skin, muscle and bone paddles that makes this arterial donor system valuable for head and neck reconstruction. In addition, the thoracodorsal arterial system can be combined with the circumflex scapular artery system (both arteries arise from the subscapular system or are directly adjacent to one another) to further increase the skin paddle and bone paddle options. Although not always ideal, this flap may be used to reconstruct almost all defects in the head and neck.
References
- Uglešić V, Virag M, Varga S, Knežević P, Milenović A. Reconstruction following radical maxillectomy with flaps supplied by the subscapular artery. J Craniomaxillofac Surg. 2000;28(3):53-60
- Chepeha D, Khariwala S, Chanowski E, Zumsteg J, Malloy K, Moyer J, Prince M, Sacco A, Lee J. Thoracodorsal artery scapular tip autogenous transplant: vascularized bone with a long pedicle and flexible soft tissue. Arch Otolaryngol Head Neck Surg. 2010;136(10):958-64
- Sullivan M, Carroll W, Baker S, Cromp ton R, Smith-Wheelock M. The free scapular flap for head and neck reconstruction. Am J Otolaryngol. 1990; 11(5):318-27
- Urken M, Bridger A, Zur K, Genden E. The scapular osteofasciocutaneous flap: a 12-year experience. Arch Otolaryngol Head Neck Surg. 2001; 127(7):862-9
- Brown J, Bekiroglu F, Shaw R. Indications for the scapular flap in reconstructions of the head and neck. Br J Oral Maxillofac Surg. 2010;48(5):331-7
- Seneviratne S, Duong C, Taylor G. The angular branch of the thoracodorsal artery and its blood supply to the inferior angle of the scapula: an anatomical study. Plast Reconstr Surg. 1999; 104(1):85-4
- Dowthwaite S. Theurer J. Belzile M, Fung K, Franklin J, Nichols A, Yoo J. Comparison of fibular and scapular osseous free flaps for oromandibular reconstruction: a patient-centered approach to flap selection. JAMA Otolaryngol Head Neck Surg. 2013;139(3): 285-92
- Yoo J, Dowthwaite S, Fung K, Franklin J, Nichols A. "A new angle to mandibular reconstruction: the scapular tip free flap. Head Neck. 2013;35(7):980-6
- Clark J, Vesely M, Gilbert R. Scapular angle osteomyogenous flap in postmaxillectomy reconstruction: defect, reconstruction, shoulder function, and harvest technique. Head Neck-J Sci Spec, 2008; 30(1):10-20
- Miles B, Gilbert RW. Maxillary reconstruction with the scapular angle osteomyogenous free flap. Arch Otolaryngol Head Neck Surg. 2011;137(11):1130-5
- Stevens J, Rosko A, Marchiano E, Haring C, Chinn S, Malloy K, Prince M, Casper K, Moyer J, Chepeha D, Stucken C, Spector M. The Spider Limb Positioner in subscapular system free flaps. Oral Oncol. 2018; 85:24-8
- Seitz A, Papp S, C. Papp Maurer H. The anatomy of the angular branch of the thoracodorsal artery. Cells Tissues Organs. 1999;164(4):227-36
- Rowsell A, Davies D, Eizenberg N, Taylor G. The anatomy of the subscapular-thoracodorsal arterial system: study of 100 cadaver dissections. Br J Plast Surg.1984;37(4):574-6
- Wagner A, Bayles S. The angular branch: maximizing the scapular pedicle in head and neck reconstruction. Arch Otolaryngol Head Neck Surg. 2008;134(11):1214-7
- Kakibuchi M, Fujikawa M, Hosokawa K, Hikasa H, Kuwae K, Kawai K, Sakagami M. Functional reconstruction of maxilla with free latissimus dorsiscapular osteomusculocutaneous flap. Plast Reconstr Surg. 2002;109(4):1238- 44
- Hanasono M, Skoracki R. The scapular tip osseous free flap as an alternative for anterior mandibular reconstruction. Plast Reconstr Surg, 2010;125(4):164e6e
- Pagedar N, Gilbert R, Chan H, Daly M, Irish J, Siewerdsen J. Maxillary reconstruction using the scapular tip free flap: a radiologic comparison of 3D morphology. Head Neck. 2012;34(10):1377-82
- Chanowski E, Casper K, Eisbruch A, Heth J, Marentette L, Prince M, Moyer J, Chepeha D. Restoration of the orbital aesthetic subunit with the thoracodorsal artery system of flaps in patients undergoing radiation therapy. J Neurol Surg B Skull. 2013;74(5) 279-85
- Chanowski E, Casper K, Eisbruch A, Heth J, Marentette L, Prince M, Moyer J, Chepeha D. Restoration of the orbital aesthetic subunit with the thoracodorsal artery system of flaps in patients undergoing radiation therapy. J Neurol Surg B Skull. 2013;74(5):279-85
- Chepeha D, Wang S, Marentette L, Bradford C, Boyd C, Prince M, Teknos T. Restoration of the orbital aesthetic subunit in complex midface defects. Laryngoscope. 2004;114(10):1706-13
- Moyer J, Chepeha D, Prince M, Teknos T. Microvascular reconstruction of the orbital complex. Facial Plast Surg Clin N Am. 2009;17(2):225-37
- Chanowski E, Haxer M, Chepeha D. Microvascular cricoid cartilage reconstruction with the thoracodorsal artery scapular tip autogenous transplant. Laryngoscope. 2012;122(2). 282-5
- Blumberg JM, Walker P, Johnson S, Johnson B, Yu E, Lacasse MC, Lam DK, Rittenberg B, Yao CM, Chepeha D, de Almeida JR. Mandibular reconstruction with the scapula tip free flap. Head Neck. 2019; doi: 10.1002/ hed.25702. [Epub ahead of print]
Other flaps described in The Open Access Atlas of Otolaryngology Head & Neck Operative Surgery
- Pectoralis major flap
- Buccinator myomucosal flap
- Buccal fat pad flap
- Nasolabial flap
- Temporalis muscle flap
- Deltopectoral flap
- Paramedian forehead flap
- Upper and lower trapezius flaps
- Cervicofacial flaps
- Submental artery island flap
- Supraclavicular flap
- Latissimus dorsi flap
- Local flaps for facial reconstruction
- Radial free forearm flap
- Free fibula flap
- Rectus abdominis flap
- Anterolateral free thigh flap
- Principles and technique of microvascular anastomosis for free tissue transfer flaps in head and neck reconstructive surgery
Author
Professor Douglas Chepeha MD, MSCPH, FRCSC, FACS
Head & Neck Oncology, Reconstructive Microsurgery
Universtiy Health Network, Princess
Margaret Hospital
Department of Otolaryngology-Head & Neck Surgery
University of Toronto
Toronto, Ontario, Canada
douglas.chepeha@uhn.ca
Acknowledgements
Carolyn Barsoum BSc
University of Manatoba
Winnipeg, Manitoba, Canada
carolyn.barsoum@uhn.ca
Feben Alemu BSc
University of Toronto
Toronto, Ontario, Canada
feben.alemu@uhn.ca
Editor
Johan Fagan MBChB, FCS (ORL), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za


