5.4: Buccinator Myomucosal Flap
- Page ID
- 15457
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
BUCCINATOR MYOMUCOSAL FLAP
Johan Fagan
The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible and versatile flap well suited to reconstructing soft tissue defects of the oral cavity, oropharynx and nasal septum. Unlike most free flaps, it provides mucosal cover, as opposed to skin cover, and is sensate. The donor site can usually be closed primarily without causing deformity or scarring. The flap is about 5 mm thick, and comprises buccal mucosa, submucosa and buccinator muscle, with the feeding vessels and vascular plexus.
Relevant Anatomy
Buccinator muscle
The buccinator muscle is a thin, quadrilateral muscle in the cheek. It originates from the outer surfaces of the alveolar processes of the maxilla and mandible. Posteriorly it arises from the pterygomandibular raphe. Anteriorly it inserts into the orbicularis oris muscle. Laterally it is related to the ramus of the mandible, the masseter and medial pterygoid muscles, the buccal fat pad and the buccopharyngeal fascia. Medially, it is covered by the submucosa and mucosa of the cheek. It is part of the pharyngealbuccal-orbicularis sphincter system and functions to facilitate whistling, sucking, propelling food during mastication and voiding the buccal cavity.
Blood supply (Figure 1)
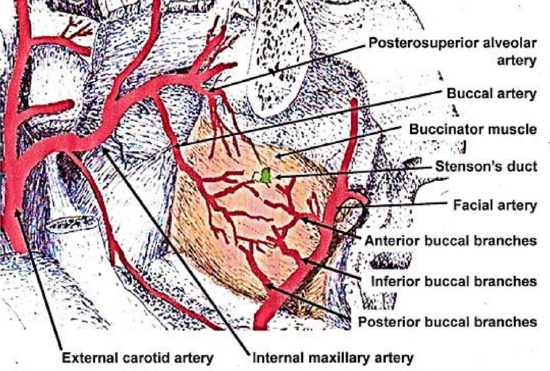
Figure 1: Blood supply of buccinator muscle, demonstrating vascular plexus
The buccal, facial and posterosuperior alveolar arteries provide the main blood supply to the muscle. These arteries form an extensive vascular anastomotic plexus on the lateral surface of the muscle and within its fibers.
The buccal artery is a branch of the internal maxillary artery and supplies the posterior half of the muscle. It courses anteroinferiorly under the lateral pterygoid muscle to reach the posterior half of the muscle, where it anastomoses with the posterior buccal branch of the facial artery.
The facial artery hooks around the inferior margin of the mandible at the anterior edge of the masseter muscle, and supplies numerous branches to the buccinator muscle, the largest of which is the posterior buccal artery that supplies the posterior half of the muscle. The facial artery also gives off 1-3 inferior buccal branches to supply the inferior half of the muscle, and then continues in an anterosuperior direction to give off 3-5 small, anterior buccal branches to the anterior half of the muscle. The posterosuperior alveolar artery is a branch of the internal maxillary artery and provides 2 small branches that enter the muscle posterosuperiorly. The infraorbital artery gives off a few small branches which enter it anterosuperiorly. Venous drainage occurs via the pterygoid plexus and internal maxillary vein. It lies posterior, superior and superficial to the buccinator muscle and drains into the buccal vein via the deep facial vein. Anteriorly, the deep facial vein drains into the facial vein proper.
Innervation
Mucosal sensory innervation is by the long buccal nerve, a branch of the maxillary division of the trigeminal nerve, which courses with the buccal branch of the internal maxillary artery. Motor innervation of the buccinator muscle is via the temporal and cervical divisions of the facial nerve laterally in the buccal fat pad.
Parotid duct
The duct pierces the buccinator muscle opposite the 2nd upper molar, slightly above the center of the muscle, and should be identified and preserved when raising the flap.
Elevation of flap
A flap as large as 7 x 5 cm may be raised. The extent is limited by the parotid duct posterosuperiorly, the oral commissure anteriorly and the pterygomandibular raphe posteriorly. It may be based posteriorly (buccal artery), or anteriorly (facial artery) or superiorly (facial artery).
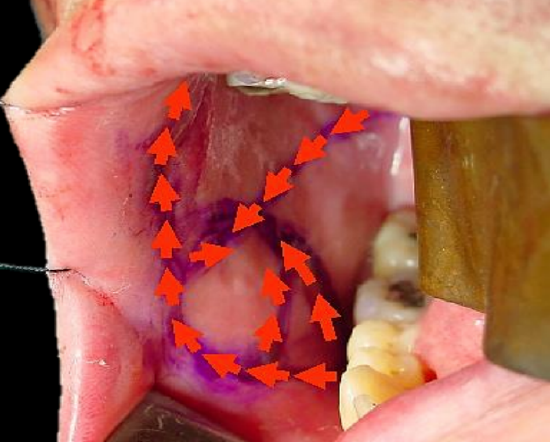
Figure 2: Vessels mapped out with handheld Doppler probe
Although not essential, a handheld Doppler can be used to map out the facial artery and the buccal artery before raising the flap (Figure 2). If a Doppler is not used, then care has to be taken to place the initial incisions so as not to separate the vessels from the flap.
The buccal mucosa and the buccinator muscle are incised to the level of the buccopharyngeal fascia, and the flap elevated, generally in an anterior to posterior direction. The flap is elevated in the loose areolar plane between the buccinator muscle and the buccopharyngeal fascia.
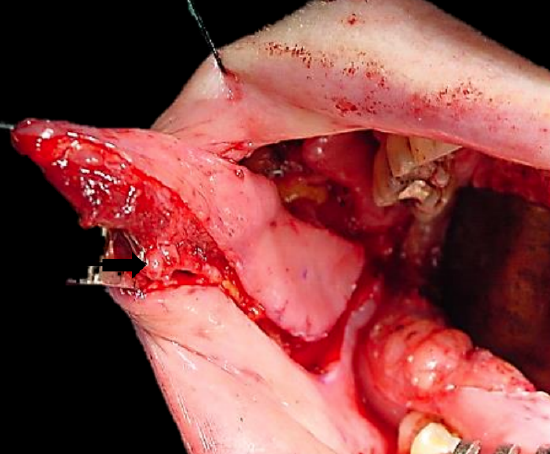
Figure 3: Flap elevation commences after identifying artery (Black arrow)
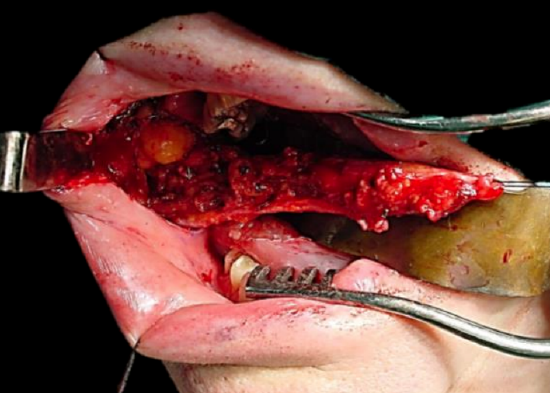
Figure 4: Flap elevated keeping artery in view
The artery that the flap will be based on is identified, and dissection proceeds between the artery and the buccopharyngeal fascia, directed towards the origin of the vascular pedicle, keeping the vessel in full view, using dissecting scissors (Figures 3, 4). Preservation of the buccopharyngeal fascia prevents herniation of buccal fat and avoids injury to branches of the facial nerve. Minor bleeding vessels are coagulated with bipolar electrocautery.
The flap is rotated to fill the soft tissue defect. The mucosa and muscle are generally not divided where the flap is pedicled. The pedicle may however be isolated to facilitate rotation, and to create a ‘buccinator myomucosal neurovascular island pedicle flap’. If the pedicle must cross the alveolus e.g. to reach the floor of mouth, then care has to be taken that the pedicle does not interpose between the molar teeth, as this may interfere with mastication and might injure the pedicle. In such cases some teeth may need to be extracted to create space for the pedicle, or an island flap must be created; alternatively, the vascular pedicle may be divided after a delay of a few weeks. Due to the elasticity of the buccal mucosa, the donor site can generally be closed primarily with vicryl absorbable sutures.
Posteriorly Based Buccinator Flap
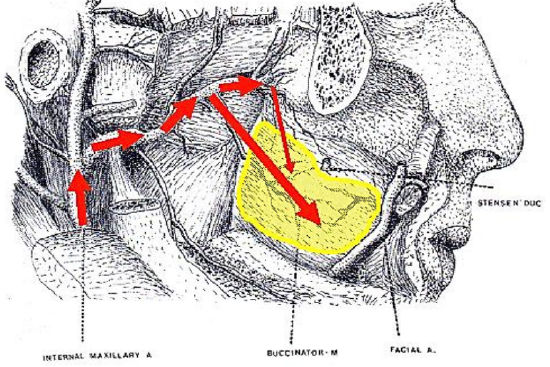
Figure 5: Blood supply of posteriorly based buccinator flap
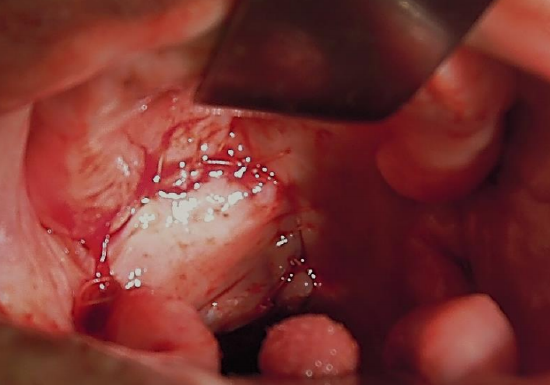
Figure 6: Posteriorly based flap used to reconstruct soft palate and tonsil fossa
This flap can be rotated to reconstruct defects of the oropharynx (soft palate, base of tongue, tonsil fossa), lateral floor of mouth, and lateral tongue. It is based posteriorly on the buccal artery and buccal venous plexus (Figures 5, 6).
Once the course of the buccal artery has been identified with Doppler ultrasound, the buccal mucosa and the buccinator muscle are incised to the level of the buccopharyngeal fascia, and the flap elevated in an anterior-to-posterior direction up to the pterygomandibular raphe where the neurovascular bundle enters the flap. The mucosa at the posterior end of the flap may also be divided from the underlying muscle and freed of its insertion to the pterygomandibular raphe and passed through a short tunnel under the pterygomandibular ligament.
Anteriorly Based Buccinator Flap
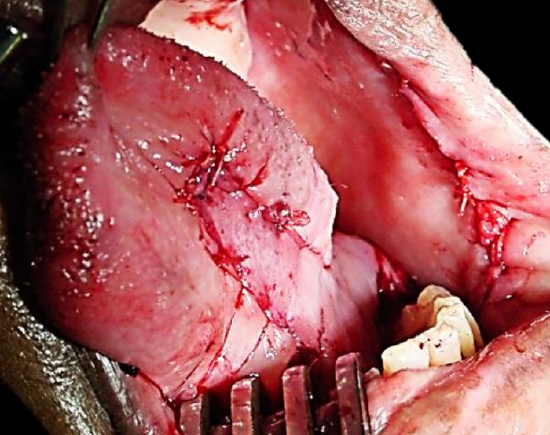
Figure 7: Flap for anterior floor of mouth
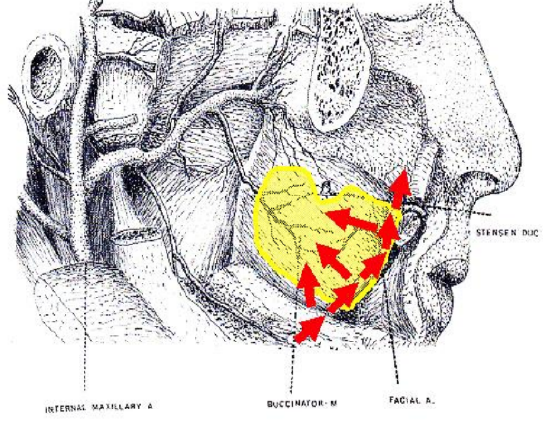
Figure 8: Blood supply of anteriorly based buccinator flap
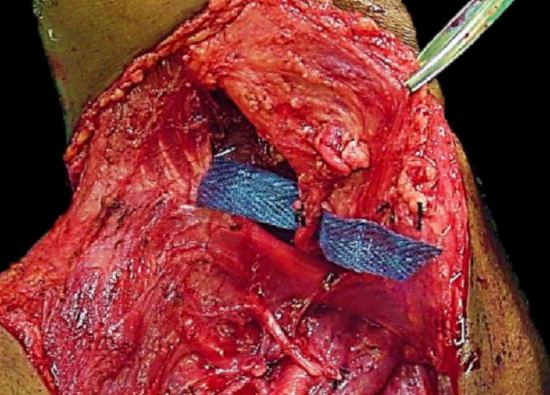
Figure 9: Preserved facial artery
The anteriorly based flap is well suited to reconstructing soft tissue defects of the inferior alveolus, lateral and anterior floor of mouth and oral tongue and lower lip (Figure 7). It is based anteroinferiorly on the inferior and posterior buccal branches of the facial artery (Figure 8). It is however essential that the facial artery be preserved when dissecting Level 1b of the neck. This requires division and ligation of branches of the facial artery where it passes through or alongside the submandibular salivary gland (Figure 9).
The mucosa and the buccinator muscle are incised just posterior (approx. 1 cm) to the commissure of the mouth, and the facial artery is identified in the cheek. The artery is ligated and divided superiorly. The dissection continues in a plane lateral to the vessels, as the flap is raised from front-to-back, and from superiorly-to-inferiorly.
Superiorly Based Buccinator Flap
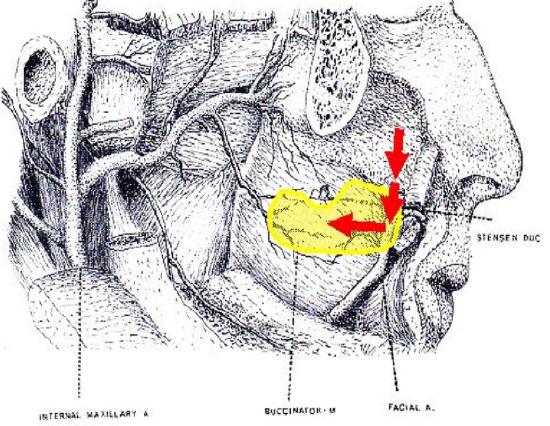
Figure 10: Blood supply of superiorly based buccinator flap
This is a reversed-flow flap based on the facial artery and its anterior buccal branches (Figure 10).
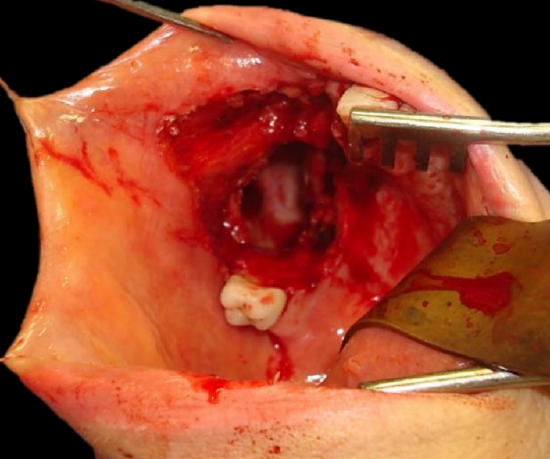
Figure 11a: Defect into antrum following alveolectomy
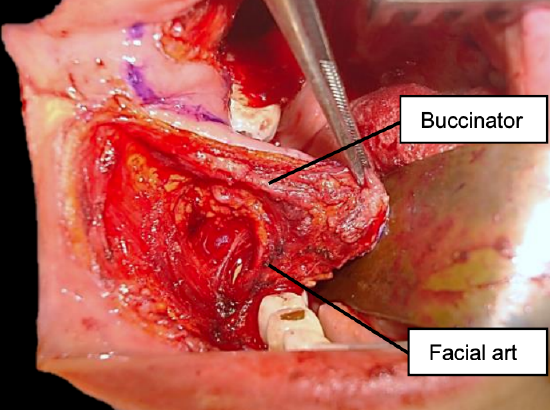
Figure 11b: Elevating flap after mapping facial artery with Doppler (purple line)
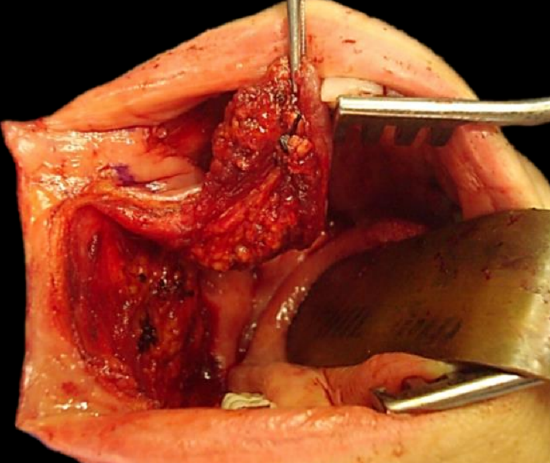
Figure 11c: Superiorly based pedicle with facial artery ligated at level of mandible
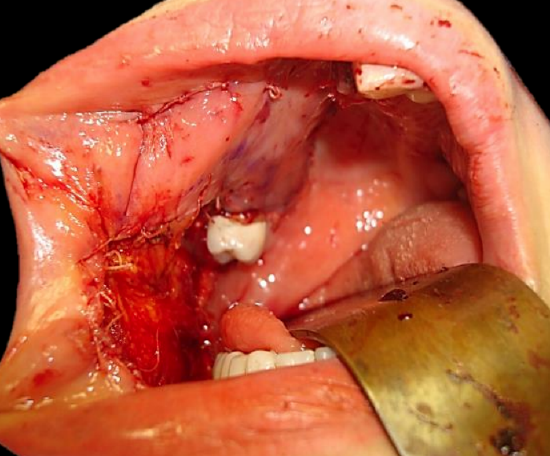
Figure 11d: Flap inset to cover antral palatal defect
It can be used for soft tissue defects of the hard palate and superior alveolus (Figure 11a), including oroantral and oronasal fistulae, as well as for nasal nasal septal defects.
Dissection is commenced at the anterior/inferior margin of the flap, where the facial artery is identified and ligated; the flap is then elevated in a superior direction and inset with vicryl sutures. If the donor defect cannot be completely closed, then it is left open to mucosalise (Figures 11b-d).
Benefits of buccinator flap
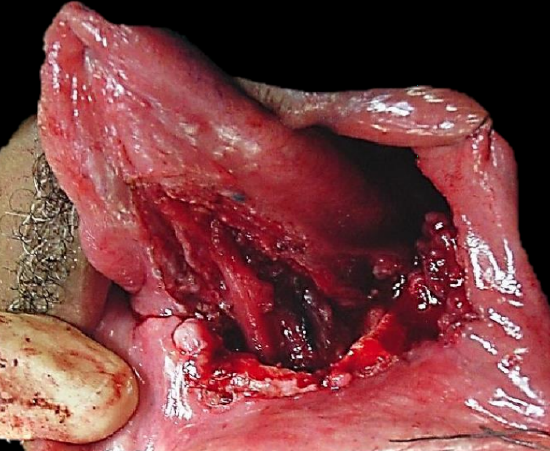
Figure 12a: Defect following anterolateral floor of mouth resection and marginal mandibulectomy
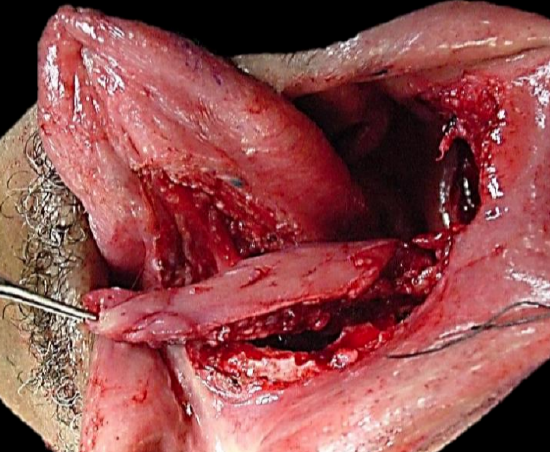
Figure 12b: Elevation of flap
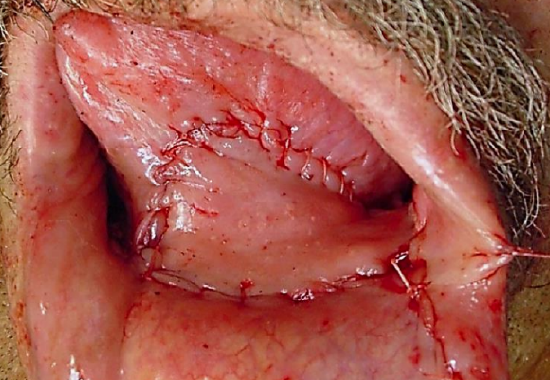
Figure 12c: Inset of flap
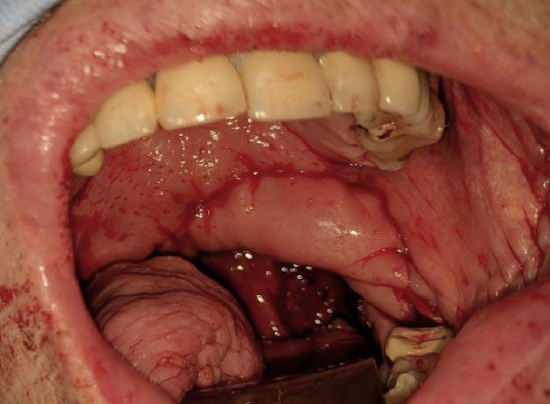
Figure 13: Soft palate and tonsil fossa defect reconstructed with buccinator flap
The buccinator flap is a versatile flap that can be used to reconstruct a variety of defects. It is very reliable, simple and quick to raise, replaces mucosa with mucosa, is sensate, and has very little donor site morbidity. It is remarkably elastic and malleable and can be stretched to conform to complexly shaped defects and is an excellent alternative to radial free forearm flaps for reconstruction of small and moderate sized defects of the oral cavity (Figures 12 a, b, c) and oropharynx (Figure 13).
Useful reference
Van Lierop A, Fagan JJ. Buccinator myomucosal flap: Clinical results and review of anatomy, surgical technique and applications. J Laryngol Otol, 2008; 122: 181-7
Other flaps described in The Open Access Atlas of Otolaryngology Head & Neck Operative Surgery
- Pectoralis major flap
- Buccal fat pad flap
- Nasolabial flap
- Temporalis muscle flap
- Deltopectoral flap
- Paramedian forehead flap
- Upper and lower trapezius flaps
- Cervicofacial flaps
- Submental artery island flap
- Supraclavicular flap
- Latissimus dorsi flap
- Local flaps for facial reconstruction
- Radial free forearm flap
- Free fibula flap
- Rectus abdominis flap
- Anterolateral free thigh flap
- Thoracodorsal artery scapular tip (TDAST) flap
- Principles and technique of microvascular anastomosis for free tissue transfer flaps in head and neck reconstructive surgery
Author & Editor
Johan Fagan MBChB, FCS(ORL), MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za


